Cystocele repair
Definition
A cystocele is the protrusion or prolapse of the bladder into the vagina. A number of surgical interventions are available to treat cystoceles.
Purpose
A prolapse occurs when an organ falls out of its normal anatomical position. The pelvic organs normally have tissue (muscle, ligaments, etc.) holding them in place. Certain factors, however, may cause those tissues to weaken, leading to prolapse of the organs. A cystocele may be the result of a central or lateral (side) defect. A central defect occurs when the bladder protrudes into the center of the anterior (front) wall of the vagina due to a defect in the pubocervical fascia (fibrous tissue that separates the bladder and vagina). The pubocervical fascia is also attached on each side to tough connective tissue called the arcus tendineus; if a defect occurs close to this attachment, it is called a lateral or paravaginal defect. A central and lateral defect may be present simultaneously. The location of the defect determines what surgical procedure is performed.
Factors that are linked to cystocele development include age, repeated childbirth, hormone deficiency, menopause, constipation, ongoing physical activity, heavy lifting, and prior hysterectomy . Symptoms of bladder prolapse include stress incontinence (inadvertent leakage of urine with physical activity), urinary frequency, difficult urination, a vaginal bulge, vaginal pressure or pain, painful sexual intercourse, and lower back pain. Urinary incontinence is the most common symptom of a cystocele.
Surgery is generally not performed unless the symptoms of the prolapse have begun to interfere with daily life. A staging system is used to grade the severity of a cystocele. A stage I, II, or III prolapse descends to progressively lower areas of the vagina. A stage IV prolapse descends to or protrudes through the vaginal opening. Surgery is generally reserved for stage III and IV cystoceles.
Demographics
Approximately 22.7 out of every 10,000 women will undergo pelvic prolapse surgery. The rate is highest among women between 60 and 69 years of age (42 per 10,000); the mean age of patients is 54.6. White women undergo pelvic prolapse surgery at a rate of 19.6 per 10,000 and a mean age of 54.3, while 6.4 per 10,000 African American women have surgery at a mean age of 49.3.
A 2002 study indicated cystocele repair accounts for 8% of all prolapse repair surgeries; in 1997, approximately 18,500 cystocele repairs were performed. Cystocele repair was combined with rectal prolapse repair in 10% of prolapse surgeries, with hysterectomy (surgical removal of the uterus) in 6%, and with both procedures in 16%.
Description
The goals of cystocele repair are to relieve a patient's symptoms, to improve or maintain urinary and sexual function, to return pelvic structures to their original position, and to prevent the formation of new defects. The anatomical structures involved in a cystocele may be approached vaginally, abdominally, or laparoscopically.
Vaginal repair
Anterior colporrhaphy is the most common procedure to repair a central defect. The patient is first given general or regional anesthesia. A speculum is inserted into the vagina to hold it open during the procedure. An incision is made into the vaginal skin and the defect in the underlying fascia is identified. The vaginal skin is separated from the fascia and the defect is folded over
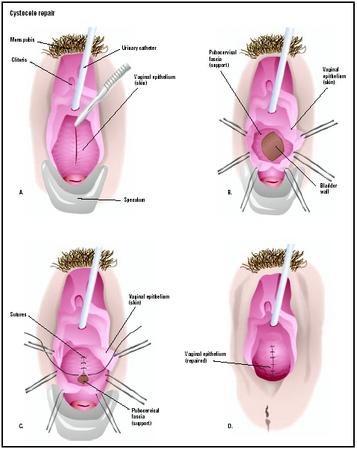
Lateral defects may be repaired vaginally or abdominally. During a vaginal paravaginal repair, the approach and initial incision are similar to anterior colporrhaphy. The defect to the fascia is located and reattached to the arcus tendineus using sutures. The incision may then be stitched closed.
Abdominal and laparoscopic repair
A cystocele caused by a lateral defect may be treated through an abdominal incision made transversely (from side to side) just above the pubic hairline. The space between the pubic bone and bladder is identified and opened and the pubocervical fascia reattached to the arcus tendineus using methods similar to the vaginal paravaginal repair. In some cases, a retropubic colposuspension is performed during the same surgery. Also called a Burch procedure, colposuspension treats urinary incontinence by suspending the bladder neck to nearby ligaments with sutures. Other surgical treatments for incontinence may be combined with paravaginal repair.
A lateral defect may also be repaired by laparoscopy , a surgical procedure in which a laparoscope (a thin, lighted tube) and various instruments are inserted into the abdomen through small incisions. A patient's recovery time following laparoscopic surgery is shorter and less painful than following a traditional laparotomy (a larger surgical incision into the abdominal cavity).
Diagnosis/Preparation
Physical examination is most often used to diagnose a cystocele. A speculum is inserted into the vagina and the patient is asked to strain or sit in an upright position; this increase in intra-abdominal pressure maximizes the degree of prolapse and aids in diagnosis. The physician then inspects the walls of the vagina for prolapse or bulging.
In some cases, a physical examination cannot sufficiently diagnose pelvic prolapse. For example, cystography may be used to determine the extent of a cystocele; the bladder is filled by urinary catheter with contrast medium and then x rayed. Ultrasound or magnetic resonance imaging may also be used to visualize the pelvic structures.
Women who have gone through menopause may be given six weeks of estrogen therapy prior to surgery; this is thought to improve circulation to the vaginal walls and thus improve recovery time. Antibiotics may be administered to decrease the risk of postsurgical infection. An intravenous (IV) line is placed and a Foley catheter is inserted into the bladder directly preceding surgery.
Aftercare
A Foley catheter may remain for one to two days after surgery. The patient is given a liquid diet until normal bowel function returns. The patient also is instructed to avoid activities for several weeks that cause strain on the surgical site; these include lifting, coughing, long periods of standing, sneezing, straining with bowel movements, and sexual intercourse.
Risks
Risks of cystocele repair include potential complications associated with anesthesia, infection, bleeding, injury to other pelvic structures, dyspareunia (painful intercourse), recurrent prolapse, and failure to correct the defect.
Normal results
A woman usually is able to resume normal activities, including sexual intercourse, in about four weeks after the procedure. After successful cystocele repair, symptoms recede, although a separate procedure may be needed to treat stress incontinence.
Morbidity and mortality rates
The risk of cystocele recurrence following surgical repair depends on the procedure used to treat it. Anterior colporrhaphy is associated with a 0–20% rate of recurrence; this rate is higher when colporrhaphy is combined with other surgical procedures. Abdominal paravaginal repair results in a 5% chance of recurrence, while vaginal paravaginal repair has the highest recurrence rate (7–22%).
Alternatives
Surgery is generally reserved for more severe cystoceles. Milder cases may be treated by a number of medical interventions. The physician may recommend that the patient do Kegel exercises, a series of contractions and relaxations of the muscles in the perineal area. These exercises are thought to strengthen the pelvic floor and may help prevent urinary incontinence.
A pessary, a device that is inserted into the vagina to help support the pelvic organs, may be recommeded. Pessaries come in different shapes and sizes and must be fitted to the patient by a physician. Hormone replacement therapy may also be prescribed if the woman has gone through menopause; hormones may improve the quality of the supporting tissues in the pelvis.
Resources
books
Ryan, Kenneth J., et al. Kistner's Gynecology and Women's Health. 7th ed. St. Louis, MO: Mosby, Inc., 1999.
Walsh, Patrick C., et al. Campbell's Urology. 8th ed. Philadelphia: Elsevier Science, 2002.
periodicals
Brown, Jeanette S., L. Elaine Waetjen, Leslee L. Subak, David H. Thom, Stephen Van Den Eeden, and Eric Vittinghoff. "Pelvic Organ Prolapse Surgery in the United States, 1997." American Journal of Obstetrics and Gynecology 186 (April 2002): 712–6.
Cespedes, R. Duane, Cindy A. Cross, and Edward J. McGuire. "Pelvic Prolapse: Diagnosing and Treating Cystoceles, Rectoceles, and Enteroceles." Medscape Women's Health eJournal 3 (1998).
Viera, Anthony, and Margaret Larkins-Pettigrew. "Practice Use of the Pessary." American Family Physician 61 (May 1, 2000): 2719–2726.
organizations
American Board of Obstetrics and Gynecology. 2915 Vine Street, Dallas, TX 75204. (214) 871-1619. http://www.abog.org .
American Urological Association. 1120 North Charles Street, Baltimore, MD 21201. (410) 727-1100. http://www.auanet.org .
other
"Cystocele (Fallen Bladder)." National Kidney and Urologic Diseases Information Clearinghouse. March 2002 [cited April 11, 2003]. http://www.niddk.nih.gov/health/urolog/summary/cystocel .
Miklos, John. "Vaginal Prolapse Relaxation." OBGYN.net . 2002 [cited April 11, 2003]. http://www.obgyn.net/urogyn/urogyn.asp?page=/urogyn/articles/miklos-vagprolapse .
Stephanie Dionne Sherk
WHO PERFORMS THE PROCEDURE AND WHERE IS IT PERFORMED?
Cystocele repair is usually performed in a hospital operating room by a gynecologist, urologist, or urogynecologist. A gynecologist is a medical doctor who specializes in the areas of women's general and reproductive health, pregnancy, and labor and childbirth. A urologist is a medical doctor who specializes in the diagnosis and treatment of diseases of the urinary tract and genital organs. A urogynecologist studies aspects of both fields.
QUESTIONS TO ASK THE DOCTOR
- What defect is causing the cystocele?
- What surgical procedure is recommended for treatment?
- Will other procedures be performed to treat urinary incontinence (e.g. Burch procedure)?
- What nonsurgical alternatives are available?
- How soon after surgery may normal activities be resumed?
thank you
Because I am still "young" and do not have a significant other, a pessary was not what I was interested in. I wanted to get "fixed".
I had cystocele/urethocele surgery last Friday. The OB/GYN said it was pretty bad, I guess as far as the stretching. Nothing was really trying to come out of me, it was just a huge "tube" anteriorly. Bleeding was MINIMAL. Bled maybe a total of 1/4, if that, of a cup the first two days, light spotting afterwards. I'm post surgery 5 days. Pain was so light, I wondered if I even had HAD the surgery. Had to home with a catheter, as I couldn't even pee a drop during recovery. My bladder was the size of a large grapefruit and still couldn't get anything out. The pain of not being able to pee with a swollen bladder was more intense than the surgery. I am 36 years old, still got a long way to see how the outcome will be.
I guess sit-ups ar out totally, period, meaning never again?
what to do to strenghten my lower palvic and ever my stomace,
besides creaglys? that not good enought to work for stomace.
Plus if any one can mail me papers on the rehab they went to
My insurance dom't pay for it. 9790 ogle rd.#3 Brem.Wa.98311
THANKS ,Also my Doc. said I can only have this done twice, what
after that? Am I going to have to carry a bag on my side?
I am totally freak
However amazingly not too bad so far, obviously not sure how much of a difference it is going to make to my symptoms as so early, but the surgery was fairly easy, felt like a painful period, or how tender you feel just after childbirth, not great but very bearable.
I am only 36 and apparently things were pretty bad, I had tried kegels, and trainers to help with them and nothing helped, my gynaecologist said I could have done a million a day and it was never going to put my bladder back where it was and that surgery was pretty much the only option, particularly being so young he didn't think it was a good idea to continue like I was. But just wanted to say that if anyone is worried about the surgery, it is really not too bad, my children are still young so getting others to help as don't want to undo things, but otherwise feel fine.
explains a lot regarding the whole procedure...especially how
to take care of oneself
This site, especially the comments by women who've had this surgery successfully has relieved me a bit. I've had a bad experience with a catheter, so I'm dreading that part. I happened upon a site that scared me a lot, all doom and gloom.
Thanks, folks, for sharing your SUCCESS stories!
Marsha
So if you need the surgery, don't hesitate to get it. Yes, we are all different, but I think a strong mental attitude will overcome anything!!
So if you need the surgery, don't hesitate to get it. Yes, we are all different, but I think a strong mental attitude will overcome anything!!
Also, the catheter came out it the hospital before being discharged - AND I went home with permission to have a regular diet - no restrictions.
The blood loss was minimal (1/4 pad or less, changing about every 3 hours) and has stopped as of this week.
thank you
Thank you
THANKS,
MARY
I hope you have had a reply from someone by now. My husand and I had the same experience. My was the anchor suture from the pro-lapse bladder repair. I went to my OBGNY and he was able to remove the piece of suture that was doing the damage. No more penis trama at our house.
I just found out 2 weeks ago that I have cystocele. I actually hadnt noticed anything at all until a week before that. Saw a Doc who said I need to see urologist to have surgery. He said it was stage 4 although there is nothing coming out of me, its a bulge at the vag opening. Anyway I have a question that is important to me. Is it ok to have sex while waiting for the surgery? I'm not in pain, I can urinate normally, Im just concerned that it will hurt. I feel bad for my hubby and myself for not having sex. Any advice or experiences anyone can share. Thank you. PS I will be 54 and the end of this month.
thank you mary
When I mentioned this to one of my doctor's nurses, she recommended the Fiber Cleanse from Lady Soma products. It was very easy to use; I just take with a glass of water once a day.
Most importantly, this stuff works!! I find it's better to take it on a regular basis, rather than waiting to get constipated and then taking it. I feel good taking it every day because I know it is all natural, and it keeps me nice and regular.
Sorry, had to find some humor in the situation!! As for now, I wouldn't change my decision for anything. I just recommend using a urologist who specializes in this type surgeries. My doctor is the only one in his office trained for it.
After 3 children I felt quite loose and after a short examination by my Gp was given an appointment at the hospital, where after another brief examination I was booked in to have the op. My prolapse was grade 2 so had a bit of a bulge but not too severe. My main concern was feeling loose during sex and not hanging on to tampons for very long which at the age of 37 I felt I would like to get sorted.
My bladder is now very weak (wasn't a problem before) and I have a big scar going through my G spot (imagine my horror when I spoke to the surgeon about this a few months after surgery and he denied the Gspot exists!) I now have no feeling in my vagina, my clitoris has shrivelled and I am completely unable to orgasm, something that I found relatively easy to do before. I have excruciating pain sporadically in my vagina and my sex life is absolutely ruined. I was told before surgery that it may or may not improve my sex life but NEVER told it could make it worse. Im devastated to say the least and just hope with time things will improve. I URGE ANYONE WHO IS CONTEMPLATING HAVING THIS SURGERY TO AVOID IT UNLESS THEY HAVE A REALLY REALLY EXTREME PROLAPSE.
I'm 48 years old and after having 3 kids, began about 5 years ago showing symptoms of cystocele and leaking. Had uterine sling implanted which helped a great deal, but after 4 1/2 years, leaking began again. Also, vaginal bulge grew as bladder begin to protrude into my vagina; exercise and sex both became very uncomfortable. While I'm still "resting", and have a while to go before I'm allowed to have intercourse, and resume "normal" activities, my recovery is going EXTREMELY WELL!!
I spent 1 night in hospital with catheder which was removed before I went home; I was peeing normally. I had virtually no paid, just felt like bad period cramps, which I treated with Motrin, I took NO pain meds at all (tramadol and vicodin prescriptions were given to me; I never filled them). I had NO bleeding. My dr. encouraged me to take a few short walks per day and on the fourth day home, my bowel functions resumed; no pain at all (I have been drinking miralax every day and had been drinking it twice a week prior to surgery).
I advise everyone out there...DO YOUR RESEARCH!. I got 4 "second" opinions; while all of the doctors agreed on my diagnosis, each had a different way of performing the surgery. Do NOT do trans-vaginally; especially when it can it be done laporscopically. Use a urogynocologist, not just a urologist or gynocologist, urogynocologists are specilaists in this field
Find out how ofter your doctor does the procedure and his success rate. Express to him/her your fears and trepidations. Talk to everyone you can about the procedure. Follow your doctor's instructions and dont be shy about asking for help from friends and family at home...this is your body and your chance to heal...enjoy the down time!
While I was very scared and apprehensive, I'm glad I had the surgery as I look forward to going back to my life comfortably and completely.
Would hate to lose my job because someone else has to be employed. Kindly advise if my condition is serious.
It was done with an Epidural and took an hour with 6 hours in recovery where they were checking me very 5 minutes (brilliant care) A catheter was put in until the following morning, when the doctor came to remove the packaging and joked there was a rabbit on the end of it and it went on and on. They let me out that evening and since then I have taken it easy, no lifting etc., I had no bleeding just a slight discharge that a small pad took care of and I have a slight pain in my side which a Paracetamol relieves.
So anyone out there is suffering this complaint please go and have it done, it is well worth it.
You only get one chance to have the procedure done right and turn out well. It is your body that will be changed forever. Bad outcomes are hard to reverse. Choose carefully.
I had anterior repair surgery for a large cysteole seven days ago and the pain is getting worse. I have not lost any blood and am able to wee wig no difficulty just discomfort but thought that by now the pain would be improving . The pain is a burning in my vagina and seems to be worse when lying down. Has anyone else experienced this and I am concerned this is not normal
Has anyone had these four procedures completed at once? What is the success rate? Is it still a 4 to 6 week recovery period? I have the GYN answers - I want to hear from someone who has experienced it ~ many times the answer is different that the docs. Reason being is last year, I was told the procedures were too risky - (I didn't have insurance then) - but this year they aren't?
Thanks so much!
M~
Thanks to everyone for sharing. I have to make my decision soon,but like many I
am also afraid of the consequences of the surgery for the Cystocelle. I was just
Diagnosed Feb 2015.I have gone for 2nd opinion.I am still researching.Good luck
To all including myself.