Magnetic resonance imaging
Definition
Magnetic resonance imaging (MRI) is a unique and versatile medical imaging diagnostic tool. Using MRI, physicians obtain highly refined images of the body's interior. Strong magnetic fields and pulses of radio waves manipulate the body's natural magnetic, producing images not possible with other diagnostic imaging methods. MRI is particularly useful for imaging the brain and spine, as well as the soft tissues of joints and the interior structure of bones. The entire body can be imaged using MRI, and the technology poses few known health risks.
Purpose
MRI was developed in the 1980s. The latest additions to MRI technology are magnetic resonance angiography (MRA) and magnetic resonance spectroscopy (MRS). MRA studies blood flow, while MRS identifies the chemical composition of diseased tissue and produces color images of brain function. The many advantages of MRI include:
- Detail. MRI creates precise images of the body based on the varying proportions of magnetically polarizable elements in different tissues. Very minor fluctuations in chemical composition can be determined. MRI images have greater subject contrast than those produced with standard x rays, computed tomography (CT), or ultrasound, all of which depend on the differing physical properties of tissues. This contrast sensitivity lets MRI distinguish fine variations in tissues deep within the body. It is particularly useful for spotting and distinguishing diseased tissues (tumors and other lesions) early in their development. Often, physicians prescribe an MRI scan to more fully investigate earlier findings from other imaging techniques.
- Scope. All body parts can be imaged using MRI. Moreover, MRI scans are not adversely affected by bone, gas, or body waste, which can hinder other imaging techniques. (The scans can, however, be degraded by motion such as breathing, heartbeat, and normal bowel activity.) A close series of two-dimensional images can provide a three-dimensional view of a targeted area. Unlike other techniques, MRI can provide images in multiple planes.
- Safety. MRI does not depend on potentially harmful ionizing radiation, as do standard x rays and CT scans . There are no known risks specific to the procedure, other than for people who have metal objects in their bodies.
Physicians sometimes choose other imaging techniques, such as ultrasound scanning, because the MRI process is complex, time-consuming, and costly. The process requires large, expensive, and complicated equipment; a highly trained operator; and a physician specializing in radiology. Generally, MRI is prescribed only when serious symptoms or negative results from other tests indicate a need. In many cases, an alternative imaging procedure is more appropriate for the type of diagnosis needed. However, some diseases such as multiple sclerosis are best imaged by MRI.
Physicians may prescribe an MRI scan of different areas of the body.
-
Brain and head. MRI technology was developed because of the need for
brain imaging. It is one of the few imaging tools that can see through
bone (the skull) and deliver high quality pictures of the brain's
delicate soft tissue structures. MRI may be needed for patients with
symptoms of a brain tumor, stroke, or infection (such as meningitis).
MRI also may be needed when cognitive or psychological symptoms suggest
brain disease (such as Alzheimer's or Huntington's
diseases, or multiple sclerosis), or when developmental retardation
suggests a
birth defect. MRI can also provide pictures of the sinuses and other areas of the head beneath the face.
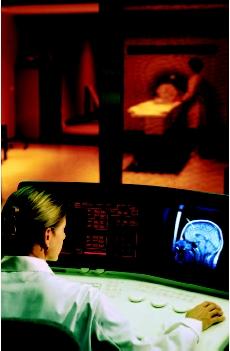 A patient receiving a magnetic resonance imaging (MRI) scan. A technologist monitors the equipment in an adjacent control room. (Will & Deni McIntyre/Photo Researchers, Inc. Reproduced by permission.)
A patient receiving a magnetic resonance imaging (MRI) scan. A technologist monitors the equipment in an adjacent control room. (Will & Deni McIntyre/Photo Researchers, Inc. Reproduced by permission.) - Spine. Spinal problems can cause neck or back pain, or numbness or weakness in the arm or leg. MRI is particularly useful for identifying and evaluating degenerated or herniated intervertebral discs. It can also be used to determine the condition of nerve tissue within the spinal cord.
- Joints. MRI scanning is often used to diagnose and assess joint problems. MRI can provide clear images of the bone, cartilage, ligaments, and tendons that comprise a joint. MRI can be used to diagnose joint damage due to sports, advancing age, or arthritis. It can also be used to diagnose shoulder problems, such as a torn rotator cuff. MRI can detect the presence of an otherwise hidden tumor or infection in a joint, and can be used to diagnose the nature of developmental joint abnormalities in children.
- Skeleton. The properties of MRI that allow it to see though the skull also allow it to view the interior of bones. It can be used to detect bone cancer, inspect the marrow for leukemia and other diseases, assess bone loss (osteoporosis), and examine complex fractures.
- The rest of the body. While CT and ultrasound satisfy most chest, abdominal, and general body imaging needs, MRI may be required to provide more detailed images in certain circumstances, or when repeated scanning is necessary. MRI is also used in cases when the progress of therapy, such as liver cancer treatment, needs to be monitored, and the effect of repeated x ray exposure is a concern.
Description
Magnetic resonance imaging
MRI produces a map of hydrogen atoms distributed in the body. Hydrogen is the simplest element known, the most abundant in biological tissue, and one that can be magnetically polarized. It will align itself within a strong magnetic field, like the needle of a compass. The earth's magnetic field is not strong enough to polarize a person's hydrogen atoms, but the superconducting magnet of an MRI machine can do this. The strength of the earth's magnetic field is approximately 1 gauss. Typical field strength of an MRI unit, with a superconducting magnet, is 1,500 gauss, expressed as 1.5 kilogauss or 1.5 Tesla units. This comprises the "magnetic" part of MRI. There are also low field units with 0.5 Tesla strength, often with open MRI units.
Once a patient's hydrogen atoms have been aligned in the magnet, pulses of very specific radio wave frequencies jolt them out of alignment. The hydrogen atoms alternately absorb and emit radio wave energy, vibrating back and forth between their resting (polarized) state and their agitated (radio pulse) state. This comprises the "resonance" part of MRI. The patient does not detect this process.
The MRI equipment detects the duration, strength, and source location of the signals emitted by the atoms as they relax. This data is translated into an image on a television monitor. The amount of hydrogen in diseased tissue differs from the amount in healthy tissue of the same type, making MRI particularly effective at identifying tumors and other lesions. In some cases, chemical agents such as gadolinium can be injected to improve the contrast between healthy and diseased tissue.
A single MRI exposure produces a two-dimensional image of a slice through the entire target area. A series of these image slices closely spaced (usually less than half an inch [1.25 cm]) provides a virtual three-dimensional view of the area.
Magnetic resonance spectroscopy
Magnetic resonance spectroscopy (MRS) is different from MRI because MRS uses a continuous band of radio wave frequencies to excite hydrogen atoms in a variety of chemical compounds other than water. These compounds absorb and emit radio energy at characteristic frequencies, or spectra, that can be used to identify them. Generally, a color image is created by assigning a hue to each distinctive spectral emission. This comprises the "spectroscopy" part of MRS. MRS is still experimental, and is available in only a few research centers.
Physicians mainly use MRS to study the brain and disorders such as epilepsy, Alzheimer's disease, brain tumors, and the effects of drugs on brain growth and metabolism. The technique is also useful in evaluating metabolic disorders of the muscles and nervous system.
Magnetic resonance angiography
Magnetic resonance angiography (MRA) is a variation on standard MRI. MRA, like other types of angiography, looks specifically at blood flow within the vascular system, without the injection of contrast agents (dye) or radioactive tracers. Standard MRI cannot detect blood flow, but MRA uses specific radio pulse sequences to capture usable signals. The technique is generally used in combination with MRI to obtain images that show both the structure of blood vessels and flow within the brain and head in cases of stroke, suspected blood clot, or aneurysm. In general, MRA is performed without contrast when examining the brain. Intravenous contrast is usually administered when other blood vessels, such as those in the neck, chest, or abdomen are studied.
Procedure
Regardless of the type of MRI planned, or area of the body targeted, the procedure involved is basically the same, and occurs in a special MRI suite. The patient lies back on a narrow table and is made as comfortable as possible. Transmitters are positioned on the body and the cushioned table that the patient is lying on moves into a long tube that houses the magnet. The tube is the length of an average adult lying down, and the tube is narrow and open at both ends. Once the area to be examined has been properly positioned, a radio pulse is applied. Then a two-dimensional image corresponding to one slice through the area is made. The table then moves a fraction of an inch and the next image is made, and so on. Each image exposure takes several seconds, and the entire exam lasts 30–90 minutes. During this time, the patient is not allowed to move. Movement during the scan results in an unclear image.
Depending on the area to be imaged, the radio-wave transmitters are positioned in different locations.
- For the head and neck, a helmet-like hat is worn.
- For the spine, chest, and abdomen, the patient lies down on transmitters known as coils.
- For the knee, shoulder, or other joint, the transmitters are applied directly to the joint.
Additional probes will monitor such vital signs as pulse and respiration.
The process is very noisy and confining. The patient hears a thumping sound for the duration of the procedure. To increase comfort, music supplied via earphones is often provided. Some patients become anxious, or they may panic because they are inside a small, enclosed tube. This is why vital signs are monitored, and the patient and medical team communicate with each other. If a patient has claustrophobia, the physician may prescribe an anti-anxiety drug prior to the procedure. If the chest or abdomen is to be imaged, the patient is asked to hold his or her breath for each exposure. Other instructions may be given as needed.
In many cases, the entire examination will be performed by an MRI operator who is not a physician. However, the supervising radiologist should be available to consult as necessary during the exam, and will view and interpret the results at a later time.
Open MRI units
Many adult patients and, especially children, become extremely claustrophobic when placed inside the confines of a full strength (1.5 Tesla) superconducting magnet. This problem is often severe enough to prevent them from having an MRI scan. In an alternative design, the magnet is comprised of two opposed halves with a large space in between. These units are known as open MRI machines. The advantage is that they can be used for patients who are claustrophobic. The disadvantage is that the field strength of the magnets is lower (usually 0.2–0.5 Tesla) than with standard full-strength machines. Lower strength magnetic fields require more time for image acquisition, increasing the risk of image problems because patients may have difficulty remaining still for longer periods of time.
Preparation
In some cases (such as for MRI brain scanning or MRA), a chemical designed to increase image contrast may be given by the radiologist immediately before the exam. If a patient suffers from anxiety or claustrophobia, drugs may be given to help the patient relax.
The patient must remove all metal objects (i.e., watches, jewelry, eyeglasses, hair clips). Any magnetized objects, such as credit and bank machine cards or audio tapes, should be kept far away from the MRI equipment because they can be erased. The patient cannnot bring a wallet or keys into the MRI machine. He or she may be asked to wear clothing without metal snaps, buckles, or zippers, unless a medical gown is provided. The patient may also be asked to remove any hair spray, hair gel, or cosmetics that could interfere with the scan.
Side effects
The potential side effects of magnetic and electric fields on human health remain a source of debate. In particular, the possible effects on an unborn baby are not well known. Any woman who is, or may be, pregnant should carefully discuss this issue with her physician and radiologist before undergoing a scan.
Chemical agents may be injected to improve the image or allow for the imaging of blood or other fluid flow during MRA. In rare cases, patients may be allergic to or intolerant of these agents, and should not receive them. If chemical agents are to be used, patients should discuss any concerns they have with their physician and radiologist.
As in other medical imaging techniques, obesity greatly interferes with the quality of MRI.
Aftercare
No aftercare is necessary, unless the patient received medication or had a reaction to a contrast agent. Normally, patients can return to their daily activities immediately. If the exam reveals a serious condition that requires more testing or treatment, appropriate information and counseling will be needed.
Precautions
MRI scanning should not be used when there is the potential for an interaction between the strong MRI magnetic field and metal objects that might be imbedded in a patient's body. The force of magnetic attraction on certain types of metal objects (including surgical steel and clips used to pinch off blood vessels) could move them within the body and cause serious injury. The movement would occur when the patient is placed into and out of the magnetic field. Metal may be imbedded in a person's body for several reasons:
- Medical. People with implanted cardiac pacemakers , metal aneurysm clips, or who have had broken bones repaired with metal pins, screws, rods, or plates must inform their radiologist prior to having an MRI scan. Generally, a joint replacement or other orthopedic hardware is not a problem if another part of the body is being scanned.
- Injury. Patients must tell their physicians if they have bullet fragments or other metal pieces in their body from old wounds. The suspected presence of metal, whether from an old or recent wound, should be confirmed before scanning.
- Occupational. People with significant work exposure to metal particles (working with a metal grinder, for example) should discuss this with their physician and radiologist. The patient may need prescan testing—usually a single, standard x ray of the eyes to see if any metal is present.
Normal results
A normal MRI, MRA, or MRS result is one that shows that the patient's physical condition falls within the normal range for the target area scanned.
Generally, MRI is prescribed only when serious symptoms or negative results from other tests indicate a need. There often exists strong evidence of a condition that the scan is designed to detect and assess. Thus, the results will often be abnormal, confirming the earlier diagnosis. At that point, further testing and appropriate medical treatment are needed. For example, if the MRI indicates the presence of a brain tumor, an MRS may be prescribed to determine the type of tumor so that aggressive treatment can begin immediately without the need for a surgical biopsy.
Resources
books
Haaga, John R., et al., eds. Computed Tomography and Magnetic Resonance Imaging of the Whole Body. St. Louis, MO: Mosby, 1994.
Hornak, Ph.D., P. Joseph. The Basics of MRI.
Zaret, Barry L., et al., eds. The Patient's Guide to Medical Tests. Boston: Houghton Mifflin Company, 1997.
periodicals
Jung, H. "Discrimination of Metastatic from Acute Osteoporotic Compression Spinal Fractures with MR Imaging." Radiographics 179 (January/February 2003).
Kevles, Bettyann "Body Imaging." Newsweek Extra Millennium Issue (Winter 97/98): 74–6.
organizations
American College of Radiology. 1891 Preston White Dr., Reston, VA 22091. (703) 648-8900. http://www.acr.org. .
American Society of Radiologic Technologists. 15000 Central Ave. SE, Albuquerque, NM 87123-3917. (505) 298-4500. http://www.asrt.org .
Center for Devices and Radiological Health. United States Food and Drug Administration. 1901 Chapman Ave., Rockville, MD 20857. (301) 443-4109. http://www.fda.gov/cdrh .
other
Smith, Steve. "Brief Introduction to FMRI." FMRIB. 1998. http://www.fmrib.ox.ac.uk/fmri_intro/ .
Stephen John Hage, AAAS, RT-R, FAHRA
Lee A. Shratter, M.D.
Just thought I would share my experience with you.
leisha dishmon
THANKS