Angiography
Definition
Angiography is the x-ray (radiographic) study of the blood vessels. An angiogram uses a radiopaque substance, or contrast medium, to make the blood vessels visible under x ray. The key ingredient in most radiographic contrast media is iodine. Arteriography is a type of radiographic examination that involves the study of the arteries.
Purpose
Angiography is used to detect abnormalities, including narrowing (stenosis) or blockages in the blood vessels (called occlusions) throughout the circulatory system and in some organs. The procedure is commonly used to identify atherosclerosis; to diagnose heart disease; to evaluate kidney function and detect kidney cysts or tumors; to map renal anatomy in transplant donors; to detect an aneurysm (an abnormal bulge of an artery that can rupture leading to hemorrhage), tumor, blood clot, or arteriovenous malformations (abnormal tangles of arteries and veins) in the brain; and to diagnose problems with the retina of the eye. It is also used to provide surgeons with an accurate vascular "map" of the heart prior to open-heart surgery, or of the brain prior to neurosurgery . Angiography may be used after penetrating trauma, like a gunshot or knife wound, to detect blood vessel injury; it may be used to check the position of shunts and stents placed by physicians into blood vessels.
Precautions
Patients with kidney disease or injury may suffer further kidney damage from the contrast media used for angiography. Patients who have blood-clotting problems, have a known allergy to contrast media, or are allergic to iodine may also not be suitable candidates for an angiography procedure. Newer types of contrast media classified as non-ionic are less toxic and cause fewer side effects than traditional ionic agents. Because x rays carry risks of ionizing radiation exposure to the fetus, pregnant women are also advised to avoid this procedure.
Description
Angiography requires the injection of a contrast medium that makes the blood vessels visible to x ray. The contrast medium is injected through a procedure known as arterial puncture. The puncture is usually made in the groin area, armpit, inside elbow, or neck.
Patients undergoing an angiogram are advised to stop eating and drinking eight hours prior to the procedure. They must remove all jewelry before the procedure and change into a hospital gown. If the arterial puncture is to be made in the armpit or groin area, shaving may be required. A sedative may be administered to relax the patient for the procedure. An IV (intravenous) line is also inserted into a vein in the patient's arm before the procedure begins, in case medication or blood products are required during the angiogram or complications arise.
Prior to the angiographic procedure, patients are briefed on the details of the test, the benefits and risks, and the possible complications involved, and asked to sign an informed consent form.
The site is cleaned with an antiseptic agent and injected with a local anesthetic. Then, a small incision is made in the skin to help the needle pass. A needle containing a solid inner core called a stylet is inserted through the incision and into the artery. When the radiologist has punctured the artery with the needle, the stylet is removed and replaced with another long wire called a guide wire. It is normal for blood to spurt out of the needle before the guide wire is inserted.
The guide wire is fed through the outer needle into the artery to the area that requires angiographic study. A fluoroscope displays a view of the patient's vascular system and is used to direct the guide wire to the correct location. Once it is in position, the needle is then removed, and a catheter is threaded over the length of the guide wire until it to reaches the area of study. The guide wire is then removed, and the catheter is left in place in preparation for the injection of the contrast medium.
Depending on the type of angiographic procedure being performed, the contrast medium is either injected by hand with a syringe or is mechanically injected with an automatic injector, sometimes called a power injector, connected to the catheter. An automatic injector is used frequently because it is able to deliver a large volume of contrast medium very quickly to the angiographic site. Usually a small test injection is made by hand to confirm that the catheter is in the correct position. The patient is told that the injection will start, and is instructed to remain very still. The injection causes some mild to moderate discomfort. Possible side effects or reactions include headache, dizziness, irregular heartbeat, nausea, warmth, burning sensation, and chest pain, but they usually last only momentarily. To view the area of study from different angles or perspectives, the patient may be asked to change positions several times, and subsequent contrast medium injections may be administered. During any injection, the patient or the imaging equipment may move.
Throughout the injection procedure, radiographs (xray pictures) or fluoroscopic images are obtained. Because of the high pressure of arterial blood flow, the contrast medium dissipates through the patient's system quickly and becomes diluted, so images must be obtained in rapid succession. One or more automatic film changers may be used to capture the required radiographic images. In many imaging departments, angiographic images are captured digitally, obviating the need for film changers. The ability to capture digital images also makes it possible to manipulate the information electronically allowing for a procedure known as digital subtraction angiography (DSA). Because every image captured is comprised of tiny picture elements called pixels, computers can be used to manipulate the information in ways that enhance diagnostic information. One common approach is to electronically remove or (subtract) bony structures that otherwise would be superimposed over the vessels being studied, hence the name digital subtraction angiography.
Once the x rays are complete, the catheter is slowly and carefully removed from the patient. Manual pressure is applied to the site with a sandbag or other weight for 10 to 20 minutes to allow for clotting to take place and the arterial puncture to reseal itself. A pressure bandage is then applied.
Most angiograms follow the general procedures outlined above, but vary slightly depending on the area of the vascular system being studied. A variety of common angiographic procedures are outlined below:
Cerebral angiography
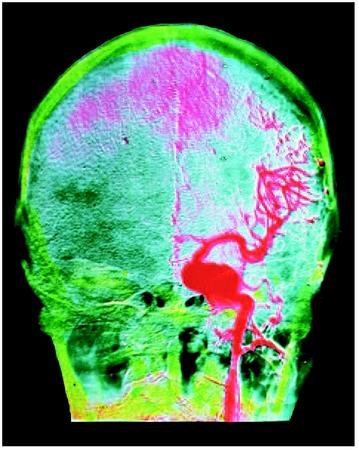
Cerebral angiography is used to detect aneurysms, stenosis, blood clots, and other vascular irregularities in the brain. The catheter is inserted into the femoral or carotid artery, and the injected contrast medium travels through the blood vessels in the brain. Patients frequently experience headache, warmth, or a burning sensation in the head or neck during the injection portion of the procedure. A cerebral angiogram takes two to four hours to complete.
Coronary angiography
Coronary angiography is administered by a cardiologist with training in radiology or, occasionally, by a radiologist. The arterial puncture is typically made in the femoral artery, and the cardiologist uses a guide wire and catheter to perform a contrast injection and x-ray series on the coronary arteries. The catheter may also be placed in the left ventricle to examine the mitral and aortic valves of the heart. If the cardiologist requires a view of the right ventricle of the heart or of the tricuspid or pulmonic valves, the catheter is inserted through a large vein and guided into the right ventricle. The catheter also serves the purpose of monitoring blood pressures in these different locations inside the heart. The angiographic procedure takes several hours, depending on the complexity of the procedure.
Pulmonary angiography
Pulmonary, or lung, angiography is performed to evaluate blood circulation to the lungs. It is also considered the most accurate diagnostic test for detecting a pulmonary embolism. The procedure differs from cerebral and coronary angiography in that the guide wire and catheter are inserted into a vein instead of an artery, and are guided up through the chambers of the heart and into the pulmonary artery. Throughout the procedure, the patient's vital signs are monitored to ensure that the catheter doesn't cause arrhythmias, or irregular heartbeats. The contrast medium is then injected into the pulmonary artery where it circulates through the lungs' capillaries. The test typically takes up to 90 minutes and carries more risk than other angiography procedures.
Kidney (renal) angiography
Patients with chronic renal disease or injury can suffer further damage to their kidneys from the contrast medium used in a renal angiogram, yet they often require the test to evaluate kidney function. These patients should be well hydrated with an intravenous saline drip before the procedure, and may benefit from available medications (e.g., dopamine) that help to protect the kidney from further injury associated with contrast agents. During a renal angiogram, the guide wire and catheter are inserted into the femoral artery in the groin area and advanced through the abdominal aorta, the main artery in the abdomen, and into the renal arteries. The procedure takes approximately one hour.
Fluorescein angiography
Fluorescein angiography is used to diagnose retinal problems and circulatory disorders. It is typically conducted as an outpatient procedure. The patient's pupils are dilated with eye drops, and he or she rests the chin and forehead against a bracing apparatus to keep it still. Sodium fluorescein dye is then injected with a syringe into a vein in the patient's arm. The dye travels through the patient's body and into the blood vessels of the eye. The procedure does not require x rays. Instead, a rapid series of close-up photographs of the patient's eyes are taken, one set immediately after the dye is injected, and a second set approximately 20 minutes later once the dye has moved through the patient's vascular system. The entire procedure takes up to one hour.
Celiac and mesenteric angiography
Celiac and mesenteric angiography involves radiographic exploration of the celiac and mesenteric arteries, arterial branches of the abdominal aorta that supply blood to the abdomen and digestive system. The test is commonly used to detect aneurysm, thrombosis, and signs of ischemia in the celiac and mesenteric arteries, and to locate the source of gastrointestinal bleeding. It is also used in the diagnosis of a number of conditions, including portal hypertension and cirrhosis. The procedure can take up to three hours, depending on the number of blood vessels studied.
Splenoportography
A splenoportograph is a variation of an angiogram that involves the injection of contrast medium directly into the spleen to view the splenic and portal veins. It is used to diagnose blockages in the splenic vein and portalvein thrombosis and to assess the patency and location of the vascular system prior to liver transplantation .
Most angiographic procedures are typically paid for by major medical insurance. Patients should check with their individual insurance plans to determine their coverage.
Computerized tomographic angiography (CTA), a new technique, is used in the evaluation of patients with intracranial aneurysms. CTA is particularly useful in delineating the relationship of vascular lesions with bony anatomy close to the skull base. While such lesions can be demonstrated with standard angiography, it often requires studying several projections of the two-dimensional films rendered with standard angiography. CTA is ideal for more anatomically complex skull-base lesions because it clearly demonstrates the exact relationship of the bony anatomy with the vascular pathology. This is not possible using standard angiographic techniques. Once the information has been captured a workstation is used to process and reconstruct images. The approach yields shaded surface displays of the actual vascular anatomy that are three dimensional and clearly show the relationship of the bony anatomy with the vascular pathology.
Angiography can also be performed using MRI ( magnetic resonance imaging ) scanners. The technique is called MRA (magnetic resonance angiography). A contrast medium is not usually used, but may be used in some body applications. The active ingredient in the contrast medium used for MRA is one of the rare earth elements, gadolinium. The contrast agent is injected into an arm vein, and images are acquired with careful attention being paid to the timing of the injection and selection of MRI specific imaging parameters. Once the information has been captured, a workstation is used to process and reconstruct the images. The post-processing capabilities associated with CTA and MRA yield three-dimensional representations of the vascular pathology being studied and can also be used to either enhance or subtract adjacent anatomical structures.
Aftercare
Because life-threatening internal bleeding is a possible complication of an arterial puncture, an overnight stay in the hospital is sometimes recommended following an angiographic procedure, particularly with cerebral and coronary angiography. If the procedure is performed on an outpatient basis, the patient is typically kept under close observation for a period of at six to 12 hours before being released. If the arterial puncture was performed in the femoral artery, the patient is instructed to keep his or her leg straight and relatively immobile during the observation period. The patient's blood pressure and vital signs are monitored, and the puncture site observed closely. Pain medication may be prescribed if the patient is experiencing discomfort from the puncture, and a cold pack is often applied to the site to reduce swelling. It is normal for the puncture site to be sore and bruised for several weeks. The patient may also develop a hematoma at the puncture site, a hard mass created by the blood vessels broken during the procedure. Hematomas should be watched carefully, as they may indicate continued bleeding of the arterial puncture site.
Angiography patients are also advised to have two to three days of rest after the procedure in order to avoid placing any undue stress on the arterial puncture site. Patients who experience continued bleeding or abnormal swelling of the puncture site, sudden dizziness, or chest pain in the days following an angiographic procedure should seek medical attention immediately.
Patients undergoing a fluorescein angiography should not drive or expose their eyes to direct sunlight for 12 hours following the procedure.
Risks
Because angiography involves puncturing an artery, internal bleeding or hemorrhage are possible complications of the test. As with any invasive procedure, infection of the puncture site or bloodstream is also a risk, but this is rare.
A stroke or heart attack may be triggered by an angiogram if blood clots or plaque on the inside of the arterial wall are dislodged by the catheter and form a blockage in the blood vessels, or if the vessel undergoes temporary narrowing or spasm from irritation by the catheter. The heart may also become irritated by the movement of the catheter through its chambers during pulmonary and coronary angiographic procedures, and arrhythmias may develop.
Patients who develop an allergic reaction to the contrast medium used in angiography may experience a variety of symptoms, including swelling, difficulty breathing, heart failure, or a sudden drop in blood pressure. If the patient is aware of the allergy before the test is administered, certain medications can be administered at that time to counteract the reaction.
Angiography involves minor exposure to radiation through the x rays and fluoroscopic guidance used in the procedure. Unless the patient is pregnant, or multiple radiological or fluoroscopic studies are required, the dose of radiation incurred during a single procedure poses little risk. However, multiple studies requiring fluoroscopic exposure that are conducted in a short time period have been known to cause skin necrosis in some individuals. This risk can be minimized by careful monitoring and documentation of cumulative radiation doses administered to these patients, particularly in those who have therapeutic procedures performed along with the diagnostic angiography.
Normal results
The results of an angiogram or arteriogram depend on the artery or organ system being examined. Generally, test results should display a normal and unimpeded flow of blood through the vascular system. Fluorescein angiography should result in no leakage of fluorescein dye through the retinal blood vessels.
Abnormal results of an angiogram may display a narrowed blood vessel with decreased arterial blood flow (ischemia) or an irregular arrangement or location of blood vessels. The results of an angiogram vary widely by the type of procedure performed, and should be interpreted by and explained to the patient by a trained radiologist.
Resources
books
Baum, Stanley and Michael J. Pentecost, eds. Abrams' Angiography. 4th ed. Philadelphia: Lippincott-Raven, 1996.
LaBergem Jeanne, ed. Interventional Radiology Essentials. 1st ed. Philadelphia: Lippincott Williams & Wilkins, 2000.
Ziessman, Harvey, ed. The Radiologic Clinics of North America, Update on Nuclear Medicine Philadelphia: W. B. Saunders Company, September 2001.
other
Food and Drug Administration. Public Health Advisory: Avoidance of Serious X-Ray-Induced Skin Injuries to Patients During Fluoroscopically Guided Procedures. September 30, 1994. Rockville, MD: Center for Devices and Radiological Health, FDA, 1994.
Radiological Society of North America CMEJ. Renal MR Angiography. April 1, 1999 [cited June 27, 2003]. http://ej.rsna.org/ej3/0091-98.fin/mainright.html .
Stephen John Hage, AAAS, RT(R), FAHRA Lee Alan Shratter, MD
Thanks.
Thanks a lot!
Another general question...What is teh name oof the drug they admminister in the ER if one has a strok or a blood clot affecting the heart? Besides medication is there a procedure for going in and extracting a clot? thanks
headache,body trembling and feeling very cold are these symptoms normal.i had to go back to the hospital wereby they gave me drips to stop nausea and headache,it did help me but my headache
still continues,wat should i do.IS IT A POSSIBLE FOR ME TO GET ANOTHER ANEUrsym,and is it herediatery
plz reply as i am very concerned
many tnx
rabia shaik
this mixed up fuzzy feeling clears up! Thank you so much Patrick.
If allergy is unknown and the pt is fearful could Benadryl and steroid be given preventively?