Laminectomy
Definition
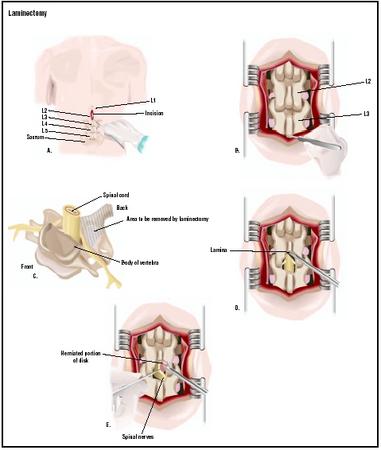
A laminectomy is a surgical procedure in which the surgeon removes a portion of the bony arch, or lamina, on the dorsal surface of a vertebra, which is one of the bones that make up the human spinal column. It is done to relieve back pain that has not been helped by more conservative treatments. In most cases a laminectomy is an elective procedure rather than emergency surgery . A laminectomy for relief of pain in the lower back is called a lumbar laminectomy or an open decompression.
Purpose
Structure of the spine
In order to understand why removal of a piece of bone from the arch of a vertebra relieves pain, it is helpful to have a brief description of the structure of the spinal column and the vertebrae themselves. In humans, the spine comprises 33 vertebrae, some of which are fused together. There are seven vertebrae in the cervical (neck) part of the spine; 12 vertebrae in the thoracic (chest) region; five in the lumbar (lower back) region; five vertebrae that are fused to form the sacrum; and four vertebrae that are fused to form the coccyx, or tail-bone. It is the vertebrae in the lumbar portion of the spine that are most likely to be affected by the disorders that cause back pain.
The 24 vertebrae that are not fused are stacked vertically in an S-shaped column that extends from the tail-bone below the waist up to the back of the head. This column is held in alignment by ligaments, cartilage, and muscles. About half the weight of a person's body is carried by the spinal column itself and the other half by the muscles and ligaments that hold the spine in alignment. The bony arches of the laminae on each vertebra form a canal that contains and protects the spinal cord. The spinal cord extends from the base of the brain to the upper part of the lumbar spine, where it ends in a collection of nerve fibers known as the cauda equina, which is a Latin phrase meaning "horse's tail." Other nerves branching out from the spinal cord pass through openings formed by adjoining vertebrae. These openings are known as foramina (singular, foramen).
Between each vertebra is a disk that serves to cushion the vertebrae when a person bends, stretches, or twists the spinal column. The disks also keep the foramina between the vertebrae open so that the spinal nerves can pass through without being pinched or damaged. As people age, the intervertebral disks begin to lose moisture and break down, which reduces the size of the foramina between the vertebrae. In addition, bone spurs may form inside the vertebrae and cause the spinal canal itself to become narrower. Either of these processes can compress the spinal nerves, leading to pain, tingling sensations, or weakness in the lower back and legs. A lumbar laminectomy relieves pressure on the spinal nerves by removing the disk, piece of bone, tumor, or other structure that is causing the compression.
Causes of lower back pain
The disks and vertebrae in the lower back are particularly vulnerable to the effects of aging and daily wear and tear because they bear the full weight of the upper body, even when one is sitting quietly in a chair. When a person bends forward, 50% of the motion occurs at the hips, but the remaining 50% involves the lumbar spine. The force exerted in bending is not evenly divided among the five lumbar vertebrae; the segments between the third and fourth lumbar vertebrae (L3-L4) and the fourth and fifth (L4-L5) are most likely to break down over time. More than 95% of spinal disk operations are performed on the fourth and fifth lumbar vertebrae.
Specific symptoms and disorders that affect the lower back include:
- Sciatica. Sciatica refers to sudden pain felt as radiating from the lower back through the buttocks and down the back of one leg. The pain, which may be experienced as weakness in the leg, a tingling feeling, or a "pins and needles" sensation, runs along the course of the sciatic nerve. Sciatica is a common symptom of a herniated disk.
- Spinal stenosis. Spinal stenosis is a disorder that results from the narrowing of the spinal canal surrounding the spinal cord and eventually compressing the cord. It may result from hereditary factors, from the effects of aging, or from changes in the pattern of blood flow to the lower back. Spinal stenosis is sometimes difficult to diagnose because its early symptoms can be caused by a number of other conditions and because the patient usually has no history of back problems or recent injuries. Imaging studies may be necessary for accurate diagnosis.
- Cauda equina syndrome (CES). Cauda equina syndrome is a rare disorder caused when a ruptured disk, bone fracture, or spinal stenosis put intense pressure on the cauda equina, the collection of spinal nerve roots at the lower end of the spinal cord. CES may be triggered by a fall, automobile accident, or penetrating gunshot injury. It is characterized by loss of sensation or altered sensation in the legs, buttocks, or feet; pain, numbness, or weakness in one or both legs; difficulty walking; or loss of control over bladder and bowel functions. Cauda equina syndrome is a medical emergency requiring immediate treatment . If the pressure on the nerves in the cauda equina is not relieved quickly, permanent paralysis and loss of bladder or bowel control may result.
- Herniated disk. The disks between the vertebrae in the spine consist of a fibrous outer part called the annulus and a softer inner nucleus. A disk is said to herniate when the nucleus ruptures and is forced through the outer annulus into the spaces between the vertebrae. The material that is forced out may put pressure on the nerve roots or compress the spinal cord itself. In other cases, the chemicals leaking from the ruptured nucleus may irritate or inflame the spinal nerves. More than 80% of herniated disks affect the spinal nerves associated with the L5 vertebra or the first sacral vertebra.
- Osteoarthritis (OA). OA is a disorder in which the cartilage in the hips, knees, and other joints gradually breaks down, allowing the surfaces of the bones to rub directly against each other. In the spine, OA may result in thickening of the ligaments surrounding the spinal column. As the ligaments increase in size, they may begin to compress the spinal cord.
Factors that increase a person's risk of developing pain in the lower back include:
- Hereditary factors. Some people are born with relatively narrow spinal canals and may develop spinal stenosis fairly early in life.
- Sex. Men are at greater risk of lower back problems than women, in part because they carry a greater proportion of their total body weight in the upper body.
- Age. The intervertebral disks tend to lose their moisture content and become thinner as people get older.
- Occupation. Jobs that require long periods of driving (long-distance trucking; bus, taxi, or limousine operation) are hard on the lower back because of vibrations from the road surface transmitted upward to the spine. Occupations that require heavy lifting (nursing, child care, construction work, airplane maintenance) put extra stress on the lumbar vertebrae. Other high-risk occupations include professional sports, professional dance, assembly line work, foundry work, mining, and mail or package delivery.
- Lifestyle. Wearing high-heeled shoes, carrying heavy briefcases or shoulder bags on one side of the body, or sitting for long periods of time in one position can all throw the spine out of alignment.
- Obesity. Being overweight, particularly if the extra pounds are concentrated in the abdomen, adds to the strain on the muscles and ligaments that support the spinal column.
- Trauma. Injuries to the back from contact sports, falls, criminal assaults, or automobile accidents may lead to misalignment of the vertebrae or a ruptured disk. Traumatic injuries may also trigger the onset of cauda equina syndrome.
Demographics
Pain in the lower back is a chronic condition that has been treated in various ways from the beginnings of human medical practice. The earliest description of disorders affecting the lumbar vertebrae was written in 3000 B.C . by an ancient Egyptian surgeon. In the modern world, back pain is responsible for more time lost from work than any other cause except the common cold. Between 10% and 15% of workers' compensation claims are related to chronic pain in the lower back. It is estimated that the direct and indirect costs of back pain to the American economy range between $75 and $80 billion per year.
In the United States, about 13 million people seek medical help each year for the condition. According to the Centers for Disease Control, 14% of all new visits to primary care doctors are related to problems in the lower back. The CDC estimates that 2.4 million adults in the United States are chronically disabled by back pain, with another 2.4 million temporarily disabled. About 70% of people will experience pain in the lower back at some point in their lifetime; on a yearly basis, one person in every five will have some kind of back pain.
Back pain primarily affects the adult population, most commonly people between the ages of 45 and 64. It is more common among men than women, and more common among Caucasians and Hispanics than among African Americans or Asian Americans.
Description
A laminectomy is performed with the patient under general anesthesia, usually positioned lying on the side or stomach. The surgeon begins by making a small straight incision over the damaged vertebra.
The surgeon next uses a retractor to spread apart the muscles and fatty tissue overlying the spine. When the laminae have been reached, the surgeon cuts away part of the bony arch in order to expose the ligamentum flavum, which is a band of yellow tissue attached to the vertebra that helps to support the spinal column and closes in the spaces between the vertebral arches. The surgeon then cuts an opening in the ligamentum flavum in order to reach the spinal canal and expose the compressed nerve. At this point the cause of the compression (herniated disk, tumor, bone spur, or a fragment of the disk that has separated from the remainder) will be visible.
Bone spurs, if any, are removed in order to enlarge the foramina and the spinal canal. If the disk is herniated, the surgeon uses the retractor to move the compressed nerve aside and removes as much of the disk as necessary to relieve pressure on the nerve. The space that was occupied by the disk will be filled eventually by new connective tissue.
If necessary, a spinal fusion is performed to stabilize the patient's lower back. A small piece of bone taken from the hip is grafted onto the spine and attached with metal screws or plates to support the lumbar vertebrae.
Following completion of the spinal fusion, the surgeon closes the incision in layers, using different types of sutures for the muscles, connective tissues, and skin. The entire procedure takes one to three hours.
Diagnosis/Preparation
Diagnosis
The differential diagnosis of lower back pain is complicated by the number of possible causes and the patient's reaction to the discomfort. In many cases the patient's perception of back pain is influenced by poor-quality sleep or emotional issues related to occupation or family matters. A primary care doctor will begin by taking a careful medical and occupational history, asking about the onset of the pain as well as its location and other characteristics. Back pain associated with the lumbar spine very often affects the patient's ability to move, and the muscles overlying the affected vertebrae may feel sore or tight. Pain resulting from heavy lifting usually begins within 24 hours of the overexertion. Most patients who do not have a history of chronic pain in the lower back feel better after 48 hours of bed rest with pain medication and either a heating pad or ice pack to relax muscle spasms.
If the patient's pain is not helped by rest and other conservative treatments, he or she will be referred to an orthopedic surgeon for a more detailed evaluation. An orthopedic evaluation includes a physical examination , neurological workup, and imaging studies. In the physical examination, the doctor will ask the patient to sit, stand, or walk in order to see how these functions are affected by the pain. The patient may be asked to cough or to lie on a table and lift each leg in turn without bending the knee, as these maneuvers can help to diagnose nerve root disorders. The doctor will also palpate (feel) the patient's spinal column and the overlying muscles and ligaments to determine the external location of any tender spots, bruises, thickening of the ligaments, or other structural abnormalities. The neurological workup will focus on the patient's reflexes and the spinal nerves that affect the functioning of the legs. Imaging studies for lower back pain typically include an x ray study and CT scan of the lower spine, which will reveal bone deformities, narrowing of the intervertebral disks, and loss of cartilage. An MRI may be ordered if spinal stenosis is suspected. In some cases the doctor may order a myelogram, which is an x ray or CT scan of the lumbar spine performed after a special dye has been injected into the spinal fluid.
Lower back pain is one of several common general medical conditions that require the doctor to assess the possibility that the patient has a concurrent psychiatric disorder. Such diagnoses as somatization disorder or pain disorder do not mean that the patient's physical symptoms are imaginary or that they should not receive surgical or medical treatment. Rather, a psychiatric diagnosis indicates that the patient is allowing the back pain to become the central focus of life or responding to it in other problematic ways. Some researchers in Europe as well as North America think that the frequency of lower back problems in workers' disability claims reflect emotional dissatisfaction with work as well as physical stresses related to specific jobs.
Preparation
Most hospitals require patients to have the following tests before a laminectomy: a complete physical examination; complete blood count (CBC) ; an electrocardiogram (EKG); a urine test; and tests that measure the speed of blood clotting.
Aspirin and arthritis medications should be discontinued seven to 10 days before a laminectomy because they thin the blood and affect clotting time. Patients should provide the surgeon and anesthesiologist with a complete list of all medications, including over-the-counter and herbal preparations, that they take on a regular basis.
The patient is asked to stop smoking at least a week before surgery and to take nothing by mouth after midnight before the procedure.
Aftercare
Aftercare following a laminectomy begins in the hospital. Most patients will remain in the hospital for one to three days after the procedure. During this period the patient will be given fluids and antibiotic medications intravenously to prevent infection. Medications for pain will be given every three to four hours, or through a device known as a PCA (patient-controlled anesthesia). The PCA is a small pump that delivers a dose of medication into the IV when the patient pushes a button. To get the lungs back to normal functioning, a respiratory therapist will ask the patient to do some simple breathing exercises and begin walking within several hours of surgery.
Aftercare during the hospital stay is also intended to lower the risk of a venous thromboembolism (VTE), or blood clot in the deep veins of the leg. Prevention of VTE involves medications to thin the blood and wearing compression stockings or boots.
Most surgeons prefer to see patients one week after surgery to remove stitches and check for any postoperative complications. Patients should not drive or return to work before their checkup. A second follow-up examination is usually done four to eight weeks after the laminectomy.
Patients can help speed their recovery by taking short walks on a daily basis; avoiding sitting or standing in the same position for long periods of time; taking brief naps during the day; and sleeping on the stomach or the side. They may take a daily bath or shower without needing to cover the incision. The incision should be carefully patted dry, however, rather than rubbed.
Risks
Risks associated with a laminectomy include:
- bleeding
- infection
- damage to the spinal cord or other nerves
- weakening or loss of function in the legs
- blood clots
- leakage of spinal fluid resulting from tears in the dura, the protective membrane that covers the spinal cord
- worsening of back pain
Normal results
Normal results depend on the cause of the patient's lower back pain; most patients can expect considerable relief from pain and some improvement in functioning. There is some disagreement among surgeons about the success rate of laminectomies, however, which appears to be due to the fact that the operation is generally done to improve quality of life—cauda equina syndrome is the only indication for an emergency laminectomy. Different sources report success rates between 26% and 99%, with 64% as the average figure. According to one study, 31% of patients were dissatisfied with the results of the operation, possibly because they may have had unrealistic expectations of the results.
Morbidity and mortality rates
The mortality rate for a lumbar laminectomy is between 0.8% and 1%. Rates of complications depend partly on whether a spinal fusion is performed as part of the procedure; while the general rate of complications following a lumbar laminectomy is given as 6–7%, the rate rises to 12% of a spinal fusion has been done.
Alternatives
Conservative treatments
Surgery for lower back pain is considered a treatment of last resort, with the exception of cauda equina syndrome. Patients should always try one or more conservative approaches before consulting a surgeon about a laminectomy. In addition, most health insurers will require proof that the surgery is necessary, since the average total cost of a lumbar laminectomy is $85,000.
Some conservative approaches that have been found to relieve lower back pain include:
- Analgesic or muscle relaxant medications. Analgesics are drugs given to relieve pain. The most commonly prescribed pain medications are aspirin or NSAIDs. Muscle relaxants include methocarbamol, cyclobenzaprine, or diazepam.
- Epidural injections. Epidural injections are given directly into the space surrounding the spinal cord. Corticosteroids are the medications most commonly given by this route, but preliminary reports indicate that epidural injections of indomethacin are also effective in relieving recurrent pain in the lower back.
- Rest. Bed rest for 48 hours usually relieves acute lower back pain resulting from muscle strain.
- Appropriate exercise . Brief walks are recommended as a good form of exercise to improve blood circulation, particularly after surgery. In addition, there are several simple exercises that can be done at home to strengthen the muscles of the lower back. A short pamphlet entitled Back Pain Exercises may be downloaded free of charge from the American Academy of Orthopedic Surgeons (AAOS) web site.
- Losing weight. People who are severely obese may wish to consider weight reduction surgery to reduce the stress on their spine as well as their heart and respiratory system.
- Occupational modifications or change. Lower back pain related to the patient's occupation can sometimes be eased by taking periodic breaks from sitting in one position; by using a desk and chair proportioned to one's height; by learning to use the muscles of the thighs when lifting heavy objects rather than the lower back muscles; and by maintaining proper posture when standing or sitting. In some cases the patient may be helped by changing occupations.
- Physical therapy. A licensed physical therapist can be helpful in identifying the patient's functional back problems and planning a course of treatment to improve flexibility, strength, and range of motion.
- Osteopathic manipulative treatment (OMT). Osteopathic physicians (DOs) receive the same training in medicine and surgery as MDs; however, they are also trained to evaluate postural and spinal abnormalities and to perform several different manual techniques for relief of back pain. An article published in the New England Journal of Medicine in 1999 reported that OMT was as effective as physical therapy and standard medication in relieving lower back pain, with fewer side effects and lower health care costs. OMT is recommended in the United Kingdom as a very low-risk treatment that is more effective than bed rest or mild analgesics.
- Transcutaneous electrical nerve stimulation (TENS). TENS is a treatment technique developed in the late 1960s that delivers a mild electrical current to stimulate nerves through electrodes attached to the skin overlying a painful part of the body. It is thought that TENS works by stimulating the production of endorphins, which are the body's natural painkilling compounds.
Surgical alternatives
The most common surgical alternative to laminectomy is a minimally invasive laminotomy and/or microdiscectomy. In this procedure, which takes about an hour, the surgeon makes a 0.5-in (1.3-cm) incision in the lower back and uses a series of small dilators to separate the layers of muscle and fatty tissue over the spine rather than cutting through them with a scalpel. A tube-shaped retractor is inserted to expose the part of the lamina over the nerve root. The surgeon then uses a power drill to make a small hole in the lamina to expose the nerve itself. After the nerve has been moved aside with the retractor, a small grasping device is used to remove the herniated portion or fragments of the damaged spinal disk.
The advantages of these minimally invasive procedures are fewer complications and a shortened recovery time for the patient. The average postoperative stay is three hours. In addition, 90% of patients are pleased with the results.
Complementary and alternative (CAM) approaches
Two alternative methods of treating back disorders that have been shown to help many patients are acupuncture and chiropractic. Chiropractic is based on the belief that the body has abilities to heal itself provided that nerve impulses can move freely between the brain and the rest of the body. Chiropractors manipulate the segments of the spine in order to bring them into proper alignment and restore the nervous system to proper functioning. Many are qualified to perform acupuncture as well as chiropractic adjustments of the vertebrae and other joints. Several British and Swedish studies have reported that acupuncture and chiropractic are at least as effective as other conservative measures in relieving pain in the lower back.
Movement therapies, including yoga, tai chi, and gentle stretching exercises, may be useful in maintaining or improving flexibility and range of motion in the spine. A qualified yoga instructor can work with the patient's doctor before or after surgery to put together an individualized set of beneficial stretching and breathing exercises. The Alexander technique is a type of movement therapy that is often helpful to patients who need to improve their posture.
See also Disk removal .
Resources
books
American Psychiatric Association. "Somatoform Disorders." In Diagnostic and Statistical Manual of Mental Disorders. 4th ed. Revised text. Washington, DC: American Psychiatric Association, 2000.
"Low Back Pain." In The Merck Manual of Diagnosis and Therapy , edited by Mark H. Beers, MD, and Robert Berkow, MD. Whitehouse Station, NJ: Merck Research Laboratories, 1999.
"Nerve Root Disorders." In The Merck Manual of Diagnosis and Therapy , edited by Mark H. Beers, MD, and Robert Berkow, MD. Whitehouse Station, NJ: Merck Research Laboratories, 1999.
"Osteoarthritis." In The Merck Manual of Diagnosis and Therapy , edited by Mark H. Beers, MD, and Robert Berkow, MD. Whitehouse Station, NJ: Merck Research Laboratories, 1999.
Pelletier, Kenneth R., MD. "Acupuncture." In The Best Alternative Medicine . New York: Simon & Schuster, 2002.
Pelletier, Kenneth R., MD. "Chiropractic." In The Best Alternative Medicine . New York: Simon & Schuster, 2002.
periodicals
Aldrete, J. A. "Epidural Injections of Indomethacin for Post-laminectomy Syndrome: A Preliminary Report." Anesthesia and Analgesia 96 (February 2003): 463–468.
Braverman, D. L., J. J. Ericken, R. V. Shah, and D. J. Franklin. "Interventions in Chronic Pain Management. 3. New Frontiers in Pain Management: Complementary Techniques." Archives of Physical Medicine and Rehabilitation 84 (March 2003) (3 Suppl 1): S45–S49.
Carlsson, C. P., and B. H. Sjolund. "Acupuncture for Chronic Low Back Pain: A Randomized Placebo-Controlled Study with Long-Term Follow-Up." Clinical Journal of Pain 17 (December 2001): 296–305.
Harvey, E., A. K. Burton, J. K. Moffett, and A. Breen. "Spinal Manipulation for Low-Back Pain: A Treatment Package Agreed to by the UK Chiropractic, Osteopathy and Physiotherapy Professional Associations." Manual Therapy 8 (February 2003): 46–51.
Hurwitz, E. L., H. Morgenstern, P. Harber, et al. "A Randomized Trial of Medical Care With and Without Physical Therapy and Chiropractic Care With and Without Physical Modalities for Patients with Low Back Pain: 6-Month Follow-Up Outcomes from the UCLA Low Back Pain Study." Spine 27 (October 15, 2002): 2193–2204.
Nasca, R. J. "Lumbar Spinal Stenosis: Surgical Considerations." Journal of the Southern Orthopedic Association 11 (Fall 2002): 127–134.
Pengel, H. M., C. G. Maher, and K. M. Refshauge. "Systematic Review of Conservative Interventions for Subacute Low Back Pain." Clinical Rehabilitation 16 (December 2002): 811–820.
Sleigh, Bryan C., MD, and Ibrahim El Nihum, MD. "Lumbar Laminectomy." eMedicine . August 8, 2002 [cited May 3, 2003]. http://www.emedicine.com/aaem/topic500.htm .
Wang, Michael Y., Barth A. Green, Sachin Shah, et al. "Complications Associated with Lumbar Stenosis Surgery in Patients Older Than 75 Years of Age." Neurosurgical Focus 14 (February 2003): 1–4.
organizations
American Academy of Neurological and Orthopedic Surgeons (AANOS). 2300 South Rancho Drive, Suite 202, Las Vegas, NV 89102. (702) 388-7390. http://www.aanos.org .
American Academy of Neurology. 1080 Montreal Avenue, Saint Paul, MN 55116. (800) 879-1960 or (651) 695-2717. http://www.aan.com .
American Academy of Orthopedic Surgeons (AAOS). 6300 North River Road, Rosemont, IL 60018. (847) 823-7186 or (800) 346-AAOS. http://www.aaos.org .
American Chiropractic Association. 1701 Clarendon Blvd., Arlington, VA 22209. (800) 986-4636. http://www.amerchiro.org .
American Osteopathic Association (AOA). 142 East Ontario Street, Chicago, IL 60611. (800) 621-1773 or (312) 202-8000. http://www.aoa-net.org .
American Physical Therapy Association (APTA). 1111 North Fairfax Street, Alexandria, VA 22314. (703)684-APTA or (800) 999-2782. http://www.apta.org .
National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS) Information Clearinghouse. National Institutes of Health, 1 AMS Circle, Bethesda, MD 20892. (301) 495-4484. TTY: (301) 565-2966. http://www.niams.nih.gov .
other
American Academy of Orthopedic Surgeons (AAOS). Back Pain Exercises. March 2000 [cited May 5, 2003]. http://www.orthoinfo.aaos.org .
American Physical Therapy Association. Taking Care of Your Back. 2003 [cited May 4, 2003]. http://www.apta.org/Consumer/ptandyourbody/back .
Waddell, G., A. McIntosh, A. Hutchinson, et al. Clinical Guidelines for the Management of Acute Low Back Pain . London, UK: Royal College of General Practitioners, 2000.
Rebecca Frey, Ph.D.
WHO PERFORMS THE PROCEDURE AND WHERE IS IT PERFORMED?
A lumbar laminectomy is performed by an orthopedic surgeon or a neurosurgeon. It is performed as an inpatient procedure in a hospital with a department of orthopedic surgery . Minimally invasive laminotomies and microdiscectomies are usually performed in outpatient surgery facilities.
QUESTIONS TO ASK THE DOCTOR
- What conservative treatments would you recommend for my lower back pain?
- How much time should I allow for conservative therapies to demonstrate effectiveness before considering surgery?
- Am I a candidate for a laminotomy and microdiscectomy?
- How many laminectomies have you performed?
Thanks for your opinion
PLEASE LET ME KNOW IF THE CIGARETE WILL HARM THE FUNSION OF THE LAMINECTOMY AFTER THE FACT.
THANK YOU IN ADVANCE FOR YOUR ATTENTION ON THIS MATTER.
Thank you,
Cynthia Engdahl
I still had pain. Even worse than before some off time. Lump on area of incision.
Dr sent me to get a MRI. They said I have a blood clot on the area that he remove bone to open up spine.
What does this mean. Dr is out of town.
Roy
Thanking you in advance, for your anticipated response and taking the time to answer and straighting me out!!
?do you think its early or what do you think went wrong
?do you have any ideas or advise for me
Hi mildred cope go see other doctor u need that. have 2nd even 3rd or 4th opinion to make u feel better. so far im happy with my operation. i even ask my doctor today if when i can go back to running and swimming and he said yes but in a moderate way like brisk walking not running and swimming is still the best exercise to our condition. i wish u well and wish to help u.
I want an actual description of what can happen, will vertebrae brake, slip out of alignment, will my spinal cord slip out of its channel. will damage be irreversible or cause me to be paralyzed?
My Mom is operated on 9th May for 4th and 5th vertebra. She was having sever left pain and numberness for few weeks. Now that is fine and now she were having sever soreness,burning feeling at the foot and because of that she was not able to walk as well. Please advice
Her lung capacity 29 persent and her discs completely compressed. She has been in ICU since tuesday in terrible pain.awaiting medical aid auth, dont want to pay prostesus. Motivation send through. What will the risk be of any complications? And what would the succesrate be on diagnoses on operation?? (Surgeon advised that above disc sections are competly compressed and condition very far.) Will the surgery relieve the pain and numbness?? Is the operation a good option toe relieve pain and numbness and to strenghten the body Spesialist advised no other option she will be paralysed for life if dont do the surgergy. PLEASE ADVISE
Any advice, information or comment is welcome.
Regards, Arthur
It's painful but tolerable
On Sunday the pain of leg cramps and spasms is intolerable. I can not move my leg cause it tightens so hard it twists and the best is when you try to sit or get off the toilet. When does this go away?? Help
Thank you very much for your response.