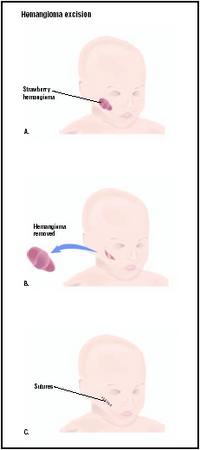
Hemangioma excision
Definition
Hemangioma excision is the use of surgical techniques to remove benign tumors made up of blood vessels that are often located within the skin. Strawberry hemangiomas are often called strawberry birthmarks. Hemangioma surgery involves the removal of the abnormal growth in a way that minimizes both physical and psychological scarring of the patient.
Purpose
Almost all hemangiomas will undergo a long, slow regression, known as involution, without treatment. The end result of involution is potentially worse than the scarring that would occur with surgery. Thus, surgical intervention is commonly indicated only if the growth of the tumor is life threatening or highly problematic from a medical or psychosocial point of view. For example, tumor growths that affect the ability of the eye to see, the ear to hear, or the passage of air in and out of the lungs are frequently candidates for surgical treatment. Tumors that have ulcerated are also common candidates for surgical treatment. Surgery after involution can be used to remove remaining scar tissue.
Although controversial, some surgeons also recommend surgery before or during the involution process, in an attempt to minimize the final cosmetic deformity. Small lesions that are in areas that can be excised without cosmetic or functional risk are particularly well-suited to early surgical treatment.
Demographics
Hemangiomas are the most common tumor of infancy, occurring in approximately 10–12% of all white children and are nearly twice as common in premature infants. For unknown reasons, the occurrence in children of black or Asian background is much lower, approximately 0.8–1.4%. The tumors have been reported to be from two to six times more common in females than in males. The great majority of these tumors are located in the head and neck, with the remaining appearing throughout the body, including internally.
At present, an estimated 60% of patients with hemangiomas require some form of corrective surgery sometime during recovery from the tumor surgery. The remaining 40% rely on the spontaneous involution process to resolve the lesion, although complete return to normalcy is extremely rare.
Description
Hemangiomas undergo a characteristic set of stages during the tumor development. Approximately 30% are present at birth, with the remainder appearing within the first few weeks of life, often beginning as a well-demarcated pale spot that becomes more noticeable when the child cries. The tumors are highly variable in presentation and range from flat, reddish areas known as superficial hemangiomas, to those that are bluish in color and located further under the skin, and are known as deep hemangiomas.
During the first six to 18 months of life, hemangiomas undergo a stage where they grow at an excessive rate in size due to abnormal cell division. The final size of the tumors can range from tiny, hardly noticeable red areas to large, disfiguring growths. In almost all hemangiomas, a long, slow involution process that follows the proliferation stage can take years to complete. Among the first signs of the involution process is a deepening of the red color of the tumor, a graying of the surface, and the appearance of white spots. In general, 50% of all hemangiomas are completely involuted by age five, and 75–90% have completed the process by age seven.
Once a decision to treat a hemangionma with surgery is made, the exact technique to be utilized must also be determined. The most commonly used technique for small lesions is very straightforward and involves removing the abnormal vascular tissue with a lenticular, or lens-shaped excision, that results in a linear scar. Recently, some surgeons have been advocating the use of an elliptical, circular, or irregular incision shapes, followed by a purse-string-type closure. This technique does result in a scar having radial (starshaped) ridges that can take several weeks to flatten. However, the overall result is a shorter scar that can be followed up by removal, using the lenticular excision technique.
Larger, more extensive lesions may require angiography , a process that maps the path of the vessels feeding the lesion, and embolization, the deliberate blocking of these blood vessels using small particles of inert material. This process is followed by complete removal of the abnormal tissue.
Depending on the size and nature of the tumor, the excision surgery can be done on an outpatient or inpatient basis. For very small lesions, local anesthetic may be sufficient, but for the great majority, general anesthesia is necessary to keep the patient comfortable.
Diagnosis/Preparation
Initial correct diagnosis of the hemangioma is necessary for effective treatment. Generally, hemangiomas are
Aftercare
Aftercare for a hemangioma excision involves wound care and maintenance such as changing of bandages.
Risks
The greatest risk of hemangioma excision is bleeding during the operation, as these tumors are comprised of abnormal blood vessels. Surgeons often utilize special surgical tools to reduce this risk, including thermoscalpels (an electrically heated scapel) and electrocauteries (a tool that stops bleeding using an electrical charge).
A second risk of the surgery is recurrence of the tumor, that is, an incomplete excision of the abnormally growing tissue. Surgery may also result in scarring that is at least as noticeable as what would remain after involution, if not more so. Patients and their caregivers should carefully consider this possibility when deciding to undergo surgical treatment for hemangiomas.
Other risks of the surgery are very low, and include those that accompany any surgical procedure, such as reactions to anesthesia and possible infections of the incision.
Normal results
Completely normal appearance after surgery is very rare. However, for significantly disfiguring tumors or those that impact physical function, the surgical scar may be preferable to the presence of the tumor.
Morbidity and mortality rates
Morbidity and mortality resulting from this surgery is close to zero, particularly because of the new surgical techniques and tools that prevent intra-operative bleeding of the tumor.
Alternatives
Several alternatives to surgical excision include observation ("watchful waiting"), treatment with steroids during the proliferation stage to shrink the tumor and speed the involution process, and laser surgery techniques to alter the appearance of the tumor. Commonly, a combination of these treatment methods, including surgery, will be used to tailor a therapeutic approach for a patient's particular tumor.
Resources
books
DuFresne, Craig R. "The Management of Hemangiomas and Vascular Malformations of the Head and Neck." In Plastic Surgery: Indications, Operations, and Outcomes, Volume 2, edited by Craig A. Vander Kolk, et al. St. Louis, MO: Mosby, 2000.
Waner, Milton, and James Y. Suen. Hemangiomas and Vascular Malformations of the Head and Neck. New York: Wiley-Liss, 1999.
periodicals
Mulliken, John B., Gary F. Rogers, and Jennifer J. Marler. "Circular Excision of Hemangioma and Purse-String Closure: The Smallest Possible Scar." Plastic and Reconstructive Surgery 109 (April 15, 2002): 1544.
organizations
American Society of Plastic Surgeons. 444 E. Algonquin Rd. Arlington Heights, IL 60005. (800) 475-2784. http://www.plasticsurgery.org .
Vascular Birthmark Foundation. P.O. Box 106, Latham, NY 12110. (877) VBF-LOOK (daytime) and (877) VBF-4646 (evenings and weekends). http://www.birthmark.org .
other
Sargent, Larry A. "Hemangiomas. " In Tennessee Craniofacial Center Monographs, 2000 [cited March 23, 2003] http://www.erlanger.org/craniofacial/book .
Michelle Johnson, MS,JD
WHO PERFORMS THE PROCEDURE AND WHERE IS IT PERFORMED?
The procedure is generally performed by plastic surgeons and, except for extremely small lesions, is done on an inpatient basis in a hospital operating room .
QUESTIONS TO ASK THE DOCTOR
- What is the predicted cosmetic outcome of the surgery and how does this compare to the outcome after involution?
- What are the risks of the surgery and how does this compare with the risks of continuing to observe the tumor?
- Is treatment of this hemangionma using steroids a possibility?
- Are laser techniques a viable option for this tumor?
Is it better to have it removed as at her age? it has shrunk about as much as it's going to. It was about the size of a quarter and red until she was about 10 or 11 years old.
This is a very recent discovery so ask your doctor about it or do a search with beta blockers to see some of the results.
I was born with the tumor itself but my mum always said it was never really noticeable until i was about 2 years old... I was on steroids which was supposed to control the tumor, but didn't actually work so i went into surgery.
I got it removed when i was 6 years old at Great Ormand Street Hospital, they helped me through so much.
I'm 16 years old now but still always get sharp pains and throbbing in my neck and cheek area where the tumor was, i mean its bearable because it happens several times throughout the day, but it is very painful for me and i'm not sure what to do? Advice would be nice. Thank you
Can u send me full details about this disease and the SPECIAL CARE to be taken, treatments,etc.
i have a 1 year old baby she has an hemongioma on her right face near eye.
how can we cure pls help. hope we will get a positive response.
thanka
mamta
In my right side of neck side so please suggest
Me what to do
My Daughter also had similar kind of bump on her eyebrow like this. We went to our GP and she suggested a Surgeon for us. We took her to the surgeon when she was three months old. The Surgeon had a look at my baby and he told it is a dermoid cyst and needs a surgery. Then I came back to my GP and told baby needs surgery. She to told to wait until she turns 6 months to proceed with the surgery. Once she turned 6 months we went to the Surgeon had an appointment for surgery and Surgery was over. After surgery, the surgeon came to us and told it is not a dermoid Cyst as expected by him, it is something else. They sent it to a lab for investigation. After two weeks for follow-up and he told us it is Hemangioma. And then I started investigating about this and found your blog. I really feel sad for my baby. I cry every time when I see her. Such a small baby has undergone a surgery which could be solved without a surgery. Now, I have a doubt whether they followed a right procedure for hemangioma removal as they never expected this during the surgery. Now, I'm worried much because the surgery should not cause any other kind of problems to the baby, I wanted to know will there be any side effects or any other problems will rise up if we do surgery for Hemangioma. Please someone help me in this.
Please mail me further steps / your guidance to my id aiswaryasekar@gmail.com
Very painful, I am uninsured, and surgery is financially out of the question at this time. It appears to be growing at a fast pace, I keep lotion on it, as it dries out, it sounds like people are living with this condition for yrs, mine is very painful, I will be eligible for Medicare next yr. I will look into having it taken off the, if I live that long.
Kindly suggest me what we will do,I am so worry about the same.
we are looking for your kind response
Thank you so much.
Have a good day
Please suggest me how this remove from her face please help me.