Cerebral aneurysm repair
Definition
Cerebral aneurysm repair involves corrective treatment of an abnormal blood-filled sac formed by localized expansion of an artery or vein within the brain. These sacs tend to form at the juncture between a primary vessel and a branch. If the vessel involved is an artery, the lesion is also known as a berry aneurysm because of its round, berry-like appearance.
Purpose
The purpose of the surgical treatment of cerebral aneurysms is to isolate the weakened vessel area from the blood supply. This is commonly done through the strategic placement of small, surgical clips to the neck of the lesion. Thus, the aneurysm becomes isolated from the normal circulation without damaging adjacent vessels or their branches and shrinks in size to become undetectable, a process known as aneurysm obliteration.
Demographics
Cerebral, or brain, aneurysms occur in about 2% of the American population. An estimated 15–33% of these patients have more than one aneurysm present. Occurrence of certain other medical conditions appears to increase the chances of developing aneurysms. These conditions include polycystic kidneys, systemic lupus erythematosus (SLE or lupus), and Ehlers-Danlos syndrome (EDS), a genetic disease that affects collagen, which is a primary component of connective tissue. Aneurysms in children are very rare, strongly suggesting that the condition develops, enlarges, and becomes symptomatic over a person's lifetime.
Other less frequent causes of aneurysms are infectious material from the heart, trauma, brain tumor, and brain arteriovenous malformation (AVM), a defect of the brain's circulatory system that results in the abnormal direct movement of blood from the arteries to the veins of the brain. The average age of cerebral aneurysm rupture is in the fifth decade of life and occurs more often in women than men by a slight margin. Environmental factors known to increase the chances of aneurysm development and rupture are cigarette smoking, excess alcohol consumption, and atherosclerotic heart disease. Some families have a definite genetic predisposition; in such families, aneurysms may run as high as 10%.
Diagnosis/Preparation
Cerebral aneurysms become apparent in two general ways: from rupture followed by bleeding within the brain, or from enlargement and compression on surrounding critical brain structures, which leads to symptoms. The most life-threatening presentation is bleeding and is often described clinically as subarachnoid hemorrhage (SAH), a term derived from the anatomic area of the brain that becomes contaminated with blood when an aneurysm ruptures. The surface of the brain is covered by three thin membranous layers, or meninges, called the dura mater, the pia mater, and the arachnoid. The dura mater adheres to the skull, while the pia mater adheres to the brain. The arachnoid lies between the other two meninges. The space between the pia mater and the arachnoid is known as the subarachnoid space and is normally filled with cerebrospinal fluid. SAH occurs when blood leaks into this space, contaminating the cerebrospinal fluid. About half of all SAH result from a ruptured cerebral aneurysm.
Clinically, the rupture causes the sudden explosive onset of a very severe headache that patients describe as the worst headache of their life. Other symptoms can include
Rupture of a cerebral aneurysm is an emergency situation. About 10% of people with SAH die within the first day, and without treatment, 25% succumb within the next three months. More than half of those who survive have significant neurological damage. Partial paralysis, weakness, or numbness may linger or be permanent, as may vision and speech problems.
When SAH is suspected, a computerized tomography (CT) scan is performed to confirm the diagnosis by visualizing the bleeding. The aneurysm itself is only rarely seen using this test. CT scanning is positive (detects the bleeding) in more than 90% of patients within the first 24 hours after the event, and for more than 50% within the first week. As time goes on, however, the bleeding becomes harder and harder to detect using this imaging method. If no bleeding is detected, a second test that could be performed is a lumbar puncture (LP), which involves drawing cerebrospinal fluid through a needle from the lower back of the patient. If SAH has occurred, the collected cerebrospinal fluid will contain blood and could be discolored yellow, caused by the presence of breakdown products of the blood cells. Other more sophisticated tests can also be performed to confirm the presence of blood and its breakdown products in the sample.
The definitive test for a cerebral aneurysm is a fluoroscopic angiogram, as it can often directly document the aneurysm, particularly its location and size. This procedure involves the placement of fluorescent material into the vein or artery of concern that increases the contrast between vessels and surrounding tissue so that their path can be clearly seen. The vessel is accessed through the insertion of a catheter in the femoral (leg) artery and threading it through the heart and into the blood vessels of the brain. A microcatheter is threaded through the larger one and used to deliver the contrast material to the precise location of the suspected aneurysm. Digital subtraction removes the bony structures from the image and leaves only the vessels. Generally, when SAH is suspected, a full cerebral angiogram that studies all four of the major cerebral arteries is performed. Modern angiograms are able to identify 85% of all cerebral aneurysms, with another 10% visible upon a second test seven to 10 days later. If this test is negative, magnetic resonance imagining (MRI), which is in some ways a more sensitive test, is often recommended.
If an aneurysm presents without rupture, some symptoms include seizures, double vision, progressive blindness in one eye, numbness on one side of the face, difficulty speaking, or, occasionally, hydrocephalus (accumulation of cerebrospinal fluid in the brain). Because of the sensitivity of available scanning techniques (particularly MRI), many aneurysms are discovered even before symptoms develop. This raises the issue of whether non-ruptured, asymptomatic aneurysms should be surgically treated.
Many health professionals view an unruptured aneurysm as a potential time bomb. In general, there is a 3% per year cumulative risk of rupture once an aneurysm is identified, or stated another way, about 0.5–0.75% of all aneurysms rupture each year. Each rupture brings with it the very high probability of serious neurological damage or even death. Furthermore, there are certain aneurysms that rupture more commonly than others, and environmental factors such as smoking and high blood pressure contribute to these events. However, all other things being equal, research indicates that by 10 years after diagnosis, there is an approximately 30% chance the aneurysm will rupture. Yet, the surgery itself carries significant risk. Whether or not to treat an unruptured aneurysm is a difficult decision and should be made only after careful consideration of the many influencing factors.
After diagnosis with a cerebral aneurysm, a patient will be put on strict bed rest and receive medication to avoid complications, keep blood pressure under control, and for pain relief.
Description
The exact timing for surgical treatment of cerebral aneurysms is historically a controversial subject in neurosurgery and is dependent on many factors including patient age, aneurysm size, aneurysm location, density of SAH, and whether the patient is comatose. Research indicates that early treatment, within the first 48 hours after hemorrhage, is generally associated with better outcomes, particularly because of the reduction of two serious complications of rupture: re-bleeding and vasospasm.
Re-bleeding is the most important cause of death if a patient survives the initial bleed and will happen in approximately 50% of all patients with a ruptured aneurysm who do not undergo surgical treatment. The peak occurrence of re-bleeding is within the first few days after rupture. About 60% of patients who re-bleed die.
The second major cause of death after rupture is vasospasm, a condition where the arteries at the base of the brain become irritated and constrict so tightly that blood cannot flow to critical brain regions. This spasm may result in further brain damage or induce re-bleeding, and much of the medical treatment after the aneurysm ruptures and prior to surgical treatment is designed to prevent this complication.
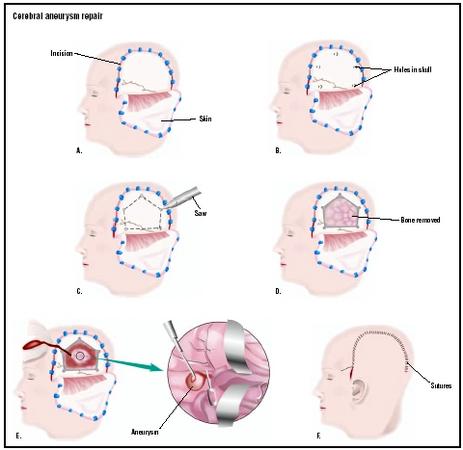
The procedure itself begins with general anesthesia of the patient and shaving of the area of the skull where the craniotomy , or opening of the skull bone, will occur. The exact position of the opening depends on the approach that the neurosurgeon will use to reach the aneurysm. The approach varies with the exact location of the aneurysm within the brain's cardiovascular system.
Once the bone flap is removed, the various layers of tissue are cut away to expose the brain. Blocking brain tissue is gently retracted back to expose the area containing the abnormal vessel formation. Surgical techniques performed through a microscope are then utilized to dissect the aneurysm away from the feeding vessels and expose the neck to receive the clip. Clips are manufactured in various types, sizes, shapes, and lengths to accommodate the needs for the various positions, shapes, and sizes of aneurysms. Clips are made of different kinds of materials, with titanium being popular because the material will not interfere with later magnetic resonance imaging (MRI) testing.
The clip is placed on the neck of the aneurysm in order to isolate it from the normal circulation. Careful clip placement will stop the flow of blood into the aneurysm, causing it to deflate or obliterate. Proper placement causes aneurysm obliteration and avoids damage to the adjacent vessels or their branches. Once the clip is in place, the brain tissue is carefully lowered back into place, the various layers sutured closed, and the bone flap is reseated for healing. The skin and other outer layers are also sutured closed. Bandages protect the area during healing.
Aftercare
Many times a postoperative angiogram is performed to confirm good clip placement, total obliteration of the aneurysm, and continued blood flow through the neighboring vessels. Because of the unpredictable nature of vessel behavior and the individual structure of each aneurysm, unexpected findings are seen in approximately 19% of postoperative angiograms. Patients stay in the hospital an average of 9.3 days after this procedure.
Risks
A major risk during surgery is a second rupture of the aneurysm during the procedure. Intraoperative rupture is very serious and associated with an approximately 30–35% morbidity and mortality of the patient. It is particularly dangerous if it occurs during the administration of the anesthesia or the opening of the dura mater because there will be a delay before the surgeon can control the bleeding.
Although much rarer than without surgical treatment, re-bleeding can occur even after surgery, particularly with improper placement of the clip. If too close to the parent vessel, the clip can block blood flow and promote brain damage in that area. If it is too far away from the parent vessel, a condition known as an aneurysmal rest can develop that will swell and rupture later. This rebleeding can also be described as a stroke, and occurs in between 1% and 10% of surgical patients.
Again rarer than without treatment, patients having their aneurysm clipped can also develop vasospasm after the procedure. The presence of vasospasm increases the occurrence of re-bleeding as well, making it a particularly dangerous complication. Treatments for vasospasm include giving medications that relax the smooth muscles in vessel walls, administering intravenous fluids to increase blood volume, or using drugs to increase blood pressure. In some cases, it may be necessary to open the vessel with a balloon catheter, a procedure called angioplasty . Angioplasty carries with it its own significant risks, including the formation of blood clots and rupture of the artery, and is effective only in some cases.
Other risks of the surgical treatment of cerebral aneurysms include neurological damage over and above what had occurred with the rupture. Special surgical procedures such as the use of temporary clips on the parent vessel, reduction of the patient's blood pressure, and administration of drugs that increase the brain tissue's ability to survive without oxygen are some techniques that minimize the amount of damage. Hypothermia (reduction of the patient's temperature during surgery) is sometimes also utilized to reduce the chance of this risk.
As this surgery involves opening of the cranium (skull), the procedure carries an increased risk of infection of brain and spinal tissues. This surgery also has all the risks of any other invasive procedure, such as infection at the incision site, and risks associated with anesthesia.
Normal results
If the postoperative angiogram indicates the clip has been properly placed, the aneurysm has been totally obliterated, and vasospasm is avoided, most patients do extremely well. However, the results of the surgery are always limited by the amount of neurological damage that occurred with the rupture itself, as much of the damage is nonreversible with current treatment methods. This issue is not a consideration with elective repair of a pre-rupture aneurysm.
Morbidity and mortality rates
Despite advances in microsurgery , anesthetic techniques, and critical care, the morbidity and mortality rates of SAH remains high at 25–35% and 40–50%, respectively. Age and neurologic status on hospital admission continue to be the best predictors of outcome.
In contrast, the operative mortality rate for elective clipping is close to 0, with morbidity ranging between 0% and 10%, especially if the surgeon is experienced in the procedure and utilizes the latest microsurgical techniques. In this situation, morbidity is most closely related to aneurysm size and location. Generally, elective clipping of an unruptured aneurysm is associated with better outcomes than ruptured aneurysms because the brain has not been damaged by the SAH prior to the procedure.
Alternatives
A promising new alternative to open surgery is the use of inventional neuroradiology to treat aneurysms. The greatest advantages to this technique are that it is less invasive and requires less recovery time in most patients. This technique is also more effective than craniotomy for certain positions of aneurysms or for patients that have complicating conditions that would make them unable to tolerate the stress of the more traditional surgery. The decision of whether an aneurysm should be treated surgically with a clip or through inventional neuroradiological techniques should be made as a team by the neurosurgeon and the endovascular radiologist.
Inventional neuroradiology, also known as endovascular neuroradiology, utilizes fluoroscopic angiography , described as a diagnostic imaging technique. Besides delivering the contrast material, the catheter can be used to place small coils, known as Gugliemlimi detachable coils, within the neck of the aneurysm using a delivery wire. Once the coil has been maneuvered into place, an electrical charge is sent through the delivery wire. This charge disintegrates the stainless steel of the coil, separating it from the delivery wire, which is removed from the body, leaving the coil. Anywhere from one to 30 coils may be necessary to block the neck of the aneurysm from the normal circulation and obliterate it, as occurs with the clip procedure. Although more research is needed to compare the two procedures, recent results indicate that intervention surgery for ruptured aneurysms may be safer than the traditionally more invasive procedure and may increase the chances of survival without disability after SAH.
Resources
books
Aldrich, E. Francois, et al. "Neurosurgery." In Textbook of Surgery, edited by Courtney m. Townsend. Philadelphia: W.B. Saunders Company, 2001.
Hoff, Julian T. and Michael F. Boland. "Neurosurgery." In Principles of Surgery, Vol. 2, edited by Seymour I. Schwartz. New York: McGraw-Hill, 1999.
periodicals
"International Subarachnoid Aneurysm Trial (ISAT) of Neurosurgical Clipping versus Endovascular Coiling in 2143 Patients with Ruptured Intracranial Aneurysms: A Randomised Trial." The Lancet 360, no. 9342 (October 2002): 1267.
Pope, Wendi L. "Cerebral Vessel Repair with Coils & Glue." Nursing (July 2002): 47–49.
organizations
American Association of Neurological Surgeons. http://www.aans.org .
American Society of Interventional and Therapeutic Neuroradiology. http://www.asitn.org .
other
Greenberg, Mark S. Handbook of Neurosurgery, 1997 [cited March 1, 2003]. http://www.grgraphics.com/site/HBNS/chapters/SAH/SAH_001.html .
Michelle Johnson, MS, JD
WHO PERFORMS THE PROCEDURE AND WHERE IS IT PERFORMED?
Surgical repair of cerebral aneurysms is performed by neurosurgeons who specialize in this procedure. It is performed in a hospital. Inventional radiology is performed by an endovascular radiologist and is also performed in a hospital.
QUESTIONS TO ASK THE DOCTOR
- What are the risks of treatment of my aneurysm?
- What are the chances of recovery using this surgical treatment method?
- What are the risks if the aneurysm is left to heal on its own?
- What are the specific characteristics of my aneurysm and how does this affect the decision to treat the problem?
- Is inventional radiology a possible means of treating my aneurysm?
Thank you,
Alex Barron
My sister is healthy, she jogs and works; is married with two lovely children and of course; the love of my life.
What can we expect?
Lillian Fritsch
Thank you.
God Bless.
My wife who had this procedure done last year has had a check up done last week and the consultant said they will just keep an eye on how the bleeding is progressing.
I am not happy with this and I feel that the aneurysm should be topped up with extra coiling before something more serious happens.
Can anyone answer my question please?
When The aneurysm rupture I fell and hit the back of my head on a marble floor. I continue to have pain in the back of my head and it has nee and the last week. I think I injured the back of my brain when I fell. Any advice would be appreciated.
Many thanks
Is there a place where I can go to discuss my issues on this?
Sally
I want to know how well he will improve. Will he be able to move his leg and hand. Will he get back his speech