Skin grafting
Definition
Skin grafting is a surgical procedure in which skin or a skin substitute is placed over a burn or non-healing wound.
Purpose
A skin graft is used to permanently replace damaged or missing skin or to provide a temporary wound covering. This covering is necessary because the skin protects the body from fluid loss, aids in temperature regulation, and helps prevent disease-causing bacteria or viruses from entering the body. Skin that is damaged extensively by burns or non-healing wounds can compromise the health and well-being of the patient.
Demographics
Although anyone can be involved in a fire and need a skin graft, the population groups with a higher risk of fire-related injuries and deaths include:
- children four years old and younger
- adults 65 years and older
- African Americans and Native Americans
- low-income Americans
- persons living in rural areas
- persons living in manufactured homes (trailers) or substandard housing
Description
The skin is the largest organ of the human body. It is also known as the integument or integumentary system because it covers the entire outside of the body. The skin consists of two main layers: the outer layer, or epidermis, which lies on and is nourished by the thicker dermis. These two layers are approximately 0.04–0.08 in (1–2 mm) thick. The epidermis consists of an outer layer of dead cells called keratinocytes, which provide a tough protective coating, and several layers of rapidly dividing cells just beneath the keratinocytes. The dermis contains the blood vessels, nerves, sweat glands, hair follicles, and oil glands. The dermis consists mainly of connective tissue, which is largely made up of a protein called collagen. Collagen gives the skin its flexibility and provides structural support. The fibroblasts that make collagen are the main type of cell in the dermis.
Skin varies in thickness in different parts of the body; it is thickest on the palms and soles of the feet, and thinnest on the eyelids. In general, men have thicker skin than women, and adults have thicker skin than children. After age 50, however, the skin begins to grow thinner again as it loses its elastic fibers and some of its fluid content.
Injuries treated with skin grafts
Skin grafting is sometimes done as part of elective plastic surgery procedures, but its most extensive use is in the treatment of burns. For first or second-degree burns, skin grafting is generally not required, as these burns usually heal with little or no scarring. With third-degree burns, however, the skin is destroyed to its full depth, in addition to damage done to underlying tissues. People who suffer third-degree burns often require skin grafting.
Wounds such as third-degree burns must be covered as quickly as possible to prevent infection or loss of fluid. Wounds that are left to heal on their own can contract, often resulting in serious scarring; if the wound is large enough, the scar can actually prevent movement of limbs. Non-healing wounds, such as diabetic ulcers, venous ulcers, or pressure sores, can be treated with skin grafts to prevent infection and further progression of the wounded area.
Types of skin grafts
The term "graft" by itself commonly refers to either an allograft or an autograft. An autograft is a type of graft
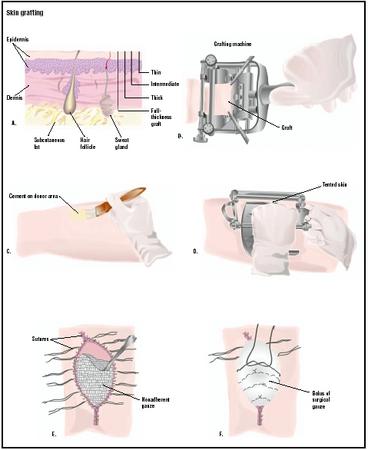
SPLIT-THICKNESS GRAFTS. The most important part of any skin graft procedure is proper preparation of the wound. Skin grafts will not survive on tissue with a limited blood supply (cartilage or tendons) or tissue that has been damaged by radiation treatment. The patient's wound must be free of any dead tissue, foreign matter, or bacterial contamination. After the patient has been anesthetized, the surgeon prepares the wound by rinsing it with saline solution or a diluted antiseptic (Betadine) and removes any dead tissue by débridement. In addition, the surgeon stops the flow of blood into the wound by applying pressure, tying off blood vessels, or administering a medication (epinephrine) that causes the blood vessels to constrict.
Following preparation of the wound, the surgeon then harvests the tissue for grafting. A split-thickness skin graft involves the epidermis and a little of the underlying dermis; the donor site usually heals within several days. The surgeon first marks the outline of the wound on the skin of the donor site, enlarging it by 3–5% to allow for tissue shrinkage. The surgeon uses a dermatome (a special instrument for cutting thin slices of tissue) to remove a split-thickness graft from the donor site. The wound must not be too deep if a split-thickness graft is going to be successful, since the blood vessels that will nourish the grafted tissue must come from the dermis of the wound itself. The graft is usually taken from an area that is ordinarily hidden by clothes, such as the buttock or inner thigh, and spread on the bare area to be covered. Gentle pressure from a well-padded dressing is then applied, or a few small sutures used to hold the graft in place. A sterile nonadherent dressing is then applied to the raw donor area for approximately three to five days to protect it from infection.
FULL-THICKNESS GRAFTS. Full-thickness skin grafts may be necessary for more severe burn injuries. These grafts involve both layers of the skin. Full-thickness autografts are more complicated than partial-thickness grafts, but provide better contour, more natural color, and less contraction at the grafted site. A flap of skin with underlying muscle and blood supply is transplanted to the area to be grafted. This procedure is used when tissue loss is extensive, such as after open fractures of the lower leg, with significant skin loss and underlying infection. The back and the abdomen are common donor sites for full-thickness grafts. The main disadvantage of full-thickness skin grafts is that the wound at the donor site is larger and requires more careful management. Often, a split-thickness graft must be used to cover the donor site.
A composite skin graft is sometimes used, which consists of combinations of skin and fat, skin and cartilage, or dermis and fat. Composite grafts are used in patients whose injuries require three-dimensional reconstruction. For example, a wedge of ear containing skin and cartilage can be used to repair the nose.
A full-thickness graft is removed from the donor site with a scalpel rather than a dermatome. After the surgeon has cut around the edges of the pattern used to determine the size of the graft, he or she lifts the skin with a special hook and trims off any fatty tissue. The graft is then placed on the wound and secured in place with absorbable sutures.
Aftercare
Once a skin graft has been put in place, it must be maintained carefully even after it has healed. Patients who have grafts on their legs should remain in bed for seven to 10 days with their legs elevated. For several months, the patient should support the graft with an Ace bandage or Jobst stocking. Grafts on other areas of the body should be similarly supported after healing to decrease the amount of contracture.
Grafted skin does not contain sweat or oil glands, and should be lubricated daily for two to three months with mineral oil or another bland oil to prevent drying and cracking.
Aftercare of patients with severe burns typically includes psychological or psychiatric counseling as well as wound care and physical rehabilitation, particularly if the patient's face has been disfigured. The severe pain and lengthy period of recovery involved in burn treatment are often accompanied by anxiety and depression. If the patient's burns occurred in combat, a transportation disaster, terrorist attack, or other fire involving large numbers of people, he or she is at high risk of developing post-traumatic stress disorder (PTSD). Doctors treating the survivors of a nightclub fire in Rhode Island in February 2003 gave them anti-anxiety medications within a few days of the tragedy in order to reduce the risk of PTSD.
Risks
The risks of skin grafting include those inherent in any surgical procedure that involves anesthesia. These include reactions to the medications, breathing problems, bleeding, and infection. In addition, the risks of an allograft procedure include transmission of an infectious disease from the donor.
The tissue for grafting and the recipient site must be as sterile as possible to prevent later infection that could result in failure of the graft. Failure of a graft can result from inadequate preparation of the wound, poor blood flow to the injured area, swelling, or infection. The most common reason for graft failure is the formation of a hematoma, or collection of blood in the injured tissues.
Normal results
A skin graft should provide significant improvement in the quality of the wound site, and may prevent the serious complications associated with burns or non-healing wounds. Normally, new blood vessels begin growing from the donor area into the transplanted skin within 36 hours. Occasionally, skin grafts are unsuccessful or don't heal well. In these cases, repeat grafting is necessary. Even though the skin graft must be protected from trauma or significant stretching for two to three weeks following split-thickness skin grafting, recovery from surgery is usually rapid. A dressing may be necessary for one to two weeks, depending on the location of the graft. Any exercise or activity that stretches the graft or puts it at risk for trauma should be avoided for three to four weeks. A one to two-week hospital stay is most often required in cases of full-thickness grafts, as the recovery period is longer.
Morbidity and mortality rates
According to the American Burn Association, there are more than 1 million burn injuries in the United States each year that require medical attention. Approximately one-half of these require hospitalization, and roughly 25,000 of those burn patients are admitted to a specialized burn unit. About 4,500 people die from burns each year in the United States.
In the United States, someone dies in a fire nearly every two hours, on average, and another person is injured every 23 minutes. Approximately half the deaths occur in homes without smoke alarms. In addition to deaths resulting directly from burns, as many as 10,000 Americans die every year of burn-related infections, pneumonia being the most common infectious complication among hospitalized burn patients.
The average size of a burn injury in a patient admitted to a burn center is approximately 14% of the total body surface area. Smaller burns covering 10% of the total body area or less account for 54% of burn center admissions, while larger burns covering 60% or more account for 4% of admissions. About 6% of patients admitted to burn centers do not survive, mostly as a result of having suffered severe inhalation injuries in a fire.
Treatment for severe burns has improved dramatically in the past 20 years. Today, patients can survive with burns covering up to about 90% of the body, although they often face permanent physical impairment.
Alternatives
There has been great progress in the development of artificial skin replacement products in recent years. Although nothing works as well as the patient's own skin, artificial skin products are important due to the limitation of available skin for allografting in severely burned patients. Unlike allographs and xenographs, artificial skin replacements are not rejected by the patient's body and actually encourage the generation of new tissue. Artificial skin usually consists of a synthetic epidermis and a collagen-based dermis. The artificial dermis consists of fibers arranged in a lattice that act as a template for the formation of new tissue. Fibroblasts, blood vessels, nerve fibers, and lymph vessels from surrounding healthy tissue grow into the collagen lattice, which eventually dissolves as these cells and structures build a new dermis. The synthetic epidermis, which acts as a temporary barrier during this process, is eventually replaced with a split-thickness autograft or with an epidermis cultured in the laboratory from the patient's own epithelial cells.
Several artificial skin products are available for burns or non-healing wounds, including Integra®, Dermal Regeneration Template® (from Integra Life Sciences Technology), Apligraft® (Novartis), Transcyte® (Advance Tissue Science), and Dermagraft®. Researchers have also obtained promising results growing or cultivating the patient's own skin cells in the laboratory. These cultured skin substitutes reduce the need for autografts and can reduce the complications of burn injuries. Laboratory cultivation of skin cells may improve the prognosis for severely burned patients with third-degree burns over 50% of their body. The recovery of these patients has been hindered by the limited availability of uninjured skin from their own bodies for grafting. Skin substitutes may also reduce treatment costs and the length of hospital stays. In addition, other research has demonstrated the possibility of using stem cells collected from bone marrow or blood for use in growing skin grafts.
Patients with less severe burns are usually treated in a doctor's office or a hospital emergency room. Patients with any of the following conditions, however, are usually transferred to hospitals with specialized burn units: third-degree burns; partial-thickness burns over 10% of their total body area; electrical or chemical burns; smoke inhalation injuries; or preexisting medical disorders that could complicate management, prolong recovery, or affect mortality. In addition, burned children in hospitals without qualified personnel should be admitted to a hospital with a burn unit. A surgical team that specializes in burn treatment and skin grafts will perform the necessary procedures. The team may include neurosurgeons, ophthalmologists, oral surgeons, thoracic surgeons, psychiatrists, and trauma specialists as well as plastic surgeons and dermatologists.
Resources
books
Beauchamp, Daniel R., M.D., Mark B. Evers, M.D., Kenneth L. Mattox, M.D., et al., eds. Sabiston Textbook of Surgery: The Biological Basis of Modern Surgical Practice , 16th ed. London, UK: W. B. Saunders Co., 2001.
Dipietro, Luisa A., and Aime L. Burns, eds. Wound Healing: Methods and Protocols. Totowa, NJ: Humana Press, 2003.
Herndon, David, ed. Total Burn Care , 2nd ed. London, UK: W. B. Saunders Co., 2001.
Tura, A., ed. Vascular Grafts: Experiment and Modelling , 1st ed. Billerica, MA: WIT Press/Computational Mechanics, 2003.
periodicals
Duenwald, Mary. "Tales from a Burn Unit: Agony, Friendship, Healing." New York Times , March 18, 2003 [June 25, 2003].
Eto, M., H. Hackstein, K. Kaneko, et al. "Promotion of Skin Graft Tolerance Across MHC Barriers by Mobilization of Dendritic Cells in Donor Hemopoietic Cell Infusions." Journal of Immunology 69 (September 1, 2002): 2390-2396.
Latenser, B. A. and Vern A. Kowal. "Paediatric Burn Rehabilitation." Pediatric Rehabilitation 5 (January-March 2002): 3-10.
Losada, F., M.D., Pedro P. Garcia-Luna, M.D., T. Gomez-Cia, M.D., et al. "Effects of Human Recombinant Growth Hormone on Donor-Site Healing in Burned Adults." World Journal of Surgery 26 (January 2002): 2-8.
Revis, Don R., Jr., MD, and Michael B. Seagal, MD. "Skin Grafts, Full-Thickness." eMedicine , May 17, 2002 [cited June 25, 2003]. http://www.emedicine.com/ent/topic48.htm .
Revis, Don R., Jr., MD, and Michael B. Seagal, MD. "Skin Grafts, Split-Thickness." eMedicine , July 20, 2001 [cited June 25, 2003]. http://www.emedicine.com/ent/topic47.htm .
Snyder, R. J., H. Doyle, and T. Delbridge. "Applying Split-Thickness Skin Grafts: A Step-by-Step Clinical Guide and Nursing Implications." Ostomy Wound Management 47 (November 2002): 990-996.
organizations
American Burn Association. 625 N. Michigan Ave., Suite 1530, Chicago, IL 60611. (800) 548-2876. Fax: (312) 642.9130. E-mail: info@ameriburn.org. http://www.ameriburn.org .
American Diabetes Association. 1701 North Beauregard Street, Alexandria, VA 22311. (800) 342-2383. E-Mail: AskADA @diabetes.org. http://www.diabetes.org .
American Society of Plastic Surgeons (ASPS). 444 East Algonquin Road, Arlington Heights, IL 60005. (847) 228-9900. http://www.plasticsurgery.org .
National Institutes of Health, 9000 Rockville Pike, Bethesda, MD 20892. (301) 496-4000. Email: NIHInfo@OD.NIH. GOV. http://www.nih.gov .
Lisa Christenson, PhD Crystal H. Kaczkowski, M.Sc.
QUESTIONS TO ASK THE DOCTOR
Skin grafts are often performed immediately following an accident or fire, and thus preparation may not be possible. If the patient has the opportunity, however, he or she may ask the doctor the following questions:
- Can you explain the process of skin grafting to me?
- Will I be sent to a hospital with a special burn unit?
- How long will I have to stay in the hospital?
- How long will recovery take?
- When will I be able to resume normal activities?
- What will the injured area look like after grafting?
thanks for your time
megan
Sincerely Yours,
Ajante Baltrip
# How long will recovery take?
actually i have acne problem and due to that spots/skin-holes never gone even i had used lots of creams and taken treatment but can anyone suggest me if know any other treatment except skin grafting.
i m too much owrried about my skin problem, please help me. thanks Hina
my brother suffers fr psoriasis and now havs 70% on his body - i wanted to find out mor info on skin grafting as we are virtually the same and im sure we can exchange skin ie take of some of his and put on me and replace with my skin - is there any chance you could perhaps poit me in the right direction or give me some confirmatory medical opinion?
i would be most grateful
half year old. accually hot milk was drawn to my hand accidently. but at that
time my parents were not in position to bear the cost of plastic surgery. thats
why they were doing traditional treatments.BAD LUCK OF MINE.
BUT mamI AM FEELING VERY abbrassed NOW. I CANT WEAR SHORT SLEAVE GARMENTS BECOZ
I HAVE BAD MARKS OF BURN ON MY RIGHT HAND.
SO PLEASE EMAIL ME REGARDING MY QUIRY.
thank you . jen
thanks a lot
King rigards
Natalia
HAS ANYONE OR DOES ANYONE KNOW WHAT HAPPENS, OR SHOULD BE DONE IN THIS SITUATION? The burn I have now, is about the size of a plum.. not quite as big, but nonetheless my graft is burnt thru...
please guide me regarding this issue and best hospital and any side effects if so ? Treatment duration approximately
Regards
Ramesh R
The sweat glands help with maintaining the moisture levels in the skin and temperature regulation so it shouldnt really be a problem as long as you keep moisturising it.
Hyper-pigmentation is what you should be careful of after a few months, you should always have sunsceen on it or the grafts will have a permanant dark tan.
If the graft is still sensitive to touch, i found that a hard scrub with a loofah glove gave the most intense sensation - including pain (painkillers help) - but after a few days to weeks the sensitivity passes.
hope i've been helpful to somebody out there.
Keep on smiling!
tom
Thanks from Dave in Hamilton, Ontario, Canada
I have 3rd degree burns on both my hands,I have done skin grafting but the skin grafting still looks like burns,please advise on how would I get my original skin color back .
Would you recommend having skin grafting done now, if I don't need a knee replacement for maybe 5 years? How long would the skin grafting last? If I waited until I needed the knee replacement can all this be done at the same time?
I appreciate any advise you can give me.
I hope this will help you .
XXOO Maxine
Sick kids hospital surgeons took skin from my buttocks and put on my ankle. This is over 45 years ago and still have the scar on my ankle. Kudos to Surgeons and Nurses back in the 1960's!
TIP - Vitamin E and Sorbelene creme was the best (perfume free of course). And eat lots of veges and drink lots of water!
She sustained 3rd degree burns on her buttucks and down the back of one of her legs. I have tried ofer the years to seek help for palstich surgery/ skin grafting however the medical professionals suggested that we let it go because it was in an area that is not seen and the risk my outway the success.
Now my daughter is an adult and her self esteem is seriously affected by the scars particularly on the back of her legs. The 3rd degree burns is worst o the buttocks. we sincerly desire to help her come up with a solution which may help her get a more cosmetically pleasing look. How much would a procedure cost? and are there less invasive procedures to consider. I am being prayer ful about this. Please send a response as well as any referrals in the Boston, MA area we could consider or at least consult with to start. Thank sin advance for your response. A cry for help to heal the pain.
My query is I met with an accident and my 4 toes were amputated.
Dr.adviced me to change the bandages(dipped in saline) trice daily,there is also an open wound present(it didn't accept the graft).Please suggest me with some thing.
WHAT NEED TO BE DONE AFTER TREATMENT TO BRING THE SKIN TO ITS ORIGINAL CONDITIN?
Please, kindly furnish me with details on procedure, the risks, the care, the duration of the healing process and other necessary things.
Thank you Sir.
Ayelabola Olaniyi
I'm a crime-thriller author and would like permission to use some of the above article in my latest novel in which one of the main characters is carrying out skin grafts on a fire-victim. If you wish, I would include my thanks for your cooperation in the Acknowledgement section of my book.
Kind regards,
Steve Dennison
web: stevedennisonthrillers.com
My operation for excission of a white patch on right cheek was done in NOV 2014 however, the post operation reports showed NAGITIVE FOR MALIGANCY. Dr placed a collagen graft on wound after sugery.
It behaved normal throughout yaer and showed perfect result.but now 10 months later i am having some pain on it and some redness is visible on the graft.
What does it shows...???
Pls help asap..
I met with a road accident 3 months back and had a skin grafting surgery on both my arms. Now that my wounds have healed I would like to know how much time it will take to be normal? And can I hit the gym now? Is there anything I can do for fast recovery from these scars?
Skin graftin how much paid in bangalore general hospital pllese in infrom
Would there have been permanent damage to the nerves? Now in my old age I have a lot of pain in the area of the burns on the chest along the intercostal nerves in-between and above the ribs. Between the skin surface and the ribs to each of the central sides of the breasts. The scarring of the burns is the type which is raised and rough and variant in texture and colour. The pain over the chest is a great bother. It is not deeper or under the ribs and is very uncomfortable.
And then you help me pls say the answer pls pls pls
Pls advice me what should I do. And the possible reason for this disturbance created after 3 years.
Note that the skin generally misbehaves during winter. ( 10- 15 degree Celsius ) but now it's about 20-25 degree temperature
I had skin graft at ankle before 2 week .not the skin very hard. what it mean and how to prevent it???
Thank you
I've been learning about skin grafting for couple of weeks now and I'm interested in the procedure itself. I've been struggling to find info about the preparation of healty and burned skin removal. Are saline solutions the normal method for preparing the area that is to be removed? How does the saline solution affect the skin and which saline slutions are normally used? Is there any other method than using saline solutions for preparation? Are saline solutions used for both healty skin that's going to be relocated and burned skin that's going to be removed? What are the pros and cons of using saline solutions?