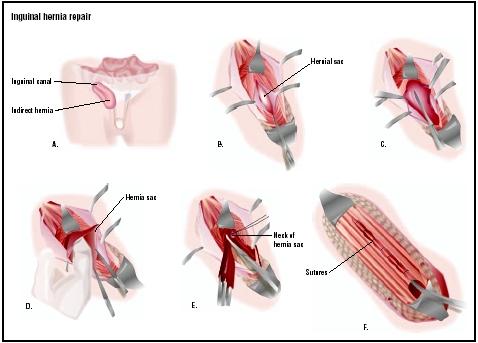
Inguinal hernia repair
Definition
Inguinal hernia repair, also known as herniorrhaphy, is the surgical correction of an inguinal hernia. An inguinal hernia is an opening, weakness, or bulge in the lining tissue (peritoneum) of the abdominal wall in the groin area between the abdomen and the thigh. The surgery may be a standard open procedure through an incision large enough
Purpose
Inguinal hernia repair is performed to close or mend the weakened abdominal wall of an inquinal hernia.
Demographics
The majority of hernias occur in males. Nearly 25% of men and only 2% of women in the United States will develop inguinal hernias. Inguinal hernias occur nearly three times more often in African American adults than in Caucasians. Among children, the risk of groin hernia is greater in premature infants or those of low birth weight. Indirect inguinal hernias will occur in 10–20 children in every 1,000 live births.
Description
About 75% of all hernias are classified as inguinal hernias, which are the most common type of hernia occurring in men and women as a result of the activities of normal living and aging. Because humans stand upright, there is a greater downward force on the lower abdomen, increasing pressure on the less muscled and naturally weaker tissues of the groin area. Inguinal hernias do not include those caused by a cut (incision) in the abdominal wall (incisional hernia). According to the National Center for Health Statistics, about 700,000 inguinal hernias are repaired annually in the United States. The inguinal hernia is usually seen or felt first as a tender and sometimes painful lump in the upper groin where the inguinal canal passes through the abdominal wall. The inguinal canal is the normal route by which testes descend into the scrotum in the male fetus, which is one reason these hernias occur more frequently in men.
Hernias are divided into two categories: congenital (from birth), also called indirect hernias, and acquired, also called direct hernias. Among the 75% of hernias classified as inguinal hernias, 50% are indirect or congenital hernias, occurring when the inguinal canal entrance fails to close normally before birth. The indirect inguinal hernia pushes down from the abdomen and through the inguinal canal. This condition is found in 2% of all adult males and in 1–2% of male children. Indirect inguinal hernias can occur in women, too, when abdominal pressure pushes folds of genital tissue into the inquinal canal opening. In fact, women will more likely have an indirect inguinal hernia than direct. Direct or acquired inguinal hernias occur when part of the large intestine protrudes through a weakened area of muscles in the groin. The weakening results from a variety of factors encountered in the wear and tear of life.
Inguinal hernias may occur on one side of the groin or both sides at the same or different times, but occur most often on the right side. About 60% of hernias found in children, for example, will be on the right side, about 30% on the left, and 10% on both sides. The muscular weak spots develop because of pressure on the abdominal muscles in the groin area occurring during normal activities such as lifting, coughing, straining during urination or bowel movements, pregnancy, or excessive weight gain. Internal organs such as the intestines may then push through this weak spot, causing a bulge of tissue. A congenital indirect inguinal hernia may be diagnosed in infancy, childhood, or later in adulthood, influenced by the same causes as direct hernia. There is evidence that a tendency for inguinal hernia may be inherited.
A direct and an indirect inguinal hernia may occur at the same time; this combined hernia is called a pantaloon hernia.
A femoral hernia is another type of hernia that appears in the groin, occurring when abdominal organs and tissue press through the femoral ring (passageway where the major femoral artery and vein extend from the leg into the abdomen) into the upper thigh. About 3% of all hernias are femoral, and 84% of all femoral hernias occur in women. These are not inquinal hernias, but they can sometimes confuse the diagnosis of inguinal hernias because they curve over the inguinal area. They are more often accompanied by intestinal obstruction than inguinal hernias.
Because inguinal hernias do not heal on their own and can become larger or twisted, which may close off the intestines, the prevailing medical opinion is that hernias must be treated surgically when they cause pain or limit activity. Protruding intestines can sometimes be pushed back temporarily into the abdominal cavity, or an external support (truss) may be worn to hold the area in place until surgery can be performed. Sometimes, other medical conditions complicate the presence of a hernia by adding constant abdominal pressure. These conditions, including chronic coughing, constipation, fluid retention, or urinary obstruction, must be treated simultaneously to reduce abdominal pressure and the recurrence of hernias after repair. A relationship between smoking and hernia development has also been shown. Groin hernias occur more frequently in smokers than nonsmokers, especially in women. A hernia may become incarcerated, which means that it is trapped in place and cannot slip back into the abdomen. This causes bowel obstruction, which may require the removal of affected parts of the intestines ( bowel resection ) as well as hernia repair. If the herniated intestine becomes twisted, blood supply to the intestines may be cut off (intestinal ischemia) and the hernia is said to be strangulated, a condition causing severe pain and requiring immediate surgery.
Surgical procedures
In open inguinal hernia repair procedures, the patient is typically given a light general anesthesia of short duration. Local or regional anesthetics may be given to some patients. Open surgical repair of an indirect hernia begins with sterilizing and draping the inguinal area of the abdomen just above the thigh. An incision is made in the abdominal wall and fatty tissue removed to expose the inguinal canal and define the outer margins of the hole or weakness in the muscle. The weakened section of tissue is dissected (cut and removed) and the inguinal canal opening is sutured closed (primary closure), making sure that no abdominal organ tissue is within the sutured area. The exposed inguinal canal is examined for any other trouble spots that may need reinforcement. Closing the underlayers of tissue (subcutaneous tissue) with fine sutures and the outer skin with staples completes the procedure. A sterile dressing is then applied.
An open repair of a direct hernia begins just as the repair of an indirect hernia, with an incision made in the same location above the thigh, just large enough to allow visualization of the hernia. The surgeon will look for and palpate (touch) the bulging area of the hernia and will reduce it by placing sutures in the fat layer of the abdominal wall. The hernial sac itself will be closed, as in the repair of the indirect hernia, by using a series of sutures from one end of the weakened hernia defect to the other. The repair will be checked for sturdiness and for any tension on the new sutures. The subcutaneous tissue and skin will be closed and a sterile dressing applied.
Laparoscopic procedures are conducted using general anesthesia. The surgeon will make three tiny incisions in the abdominal wall of the groin area and inflate the abdomen with carbon dioxide to expand the surgical area. A laparoscope, which is a tube-like fiber-optic instrument with a small video camera attached to its tip, will be inserted in one incision and surgical instruments inserted in the other incisions. The surgeon will view the movement of the instruments on a video monitor, as the hernia is pushed back into place and the hernial sac is repaired with surgical sutures or staples. Laparoscopic surgery is believed to produce less postoperative pain and a quicker recovery time. The risk of infection is also reduced because of the small incisions required in laparoscopic surgery.
The use of surgical (prosthetic) steel mesh or polypropylene mesh in the repair of inguinal hernias has been shown to help prevent recurrent hernias. Instead of the tension that develops between sutures and the skin in a conventionally repaired area, hernioplasty using mesh patches has been shown to virtually eliminate tension. The procedure is often performed in an outpatient facility with local anesthesia and patients can walk away the same day, with little restrictions in activity. Tension-free repair is also quick and easy to perform using the laparoscopic method, although general anesthesia is usually used. In either open or laparoscopic procedures, the mesh is placed so that it overlaps the healthy skin around the hernia opening and then is sutured into place with fine silk. Rather than pulling the hole closed as in conventional repair, the mesh makes a bridge over the hole and as normal healing take place, the mesh is incorporated into normal tissue without resulting tension.
Diagnosis/Preparation
Diagnosis
Reviewing the patient's symptoms and medical history are the first steps in diagnosing a hernia. The surgeon will ask when the patient first noticed a lump or bulge in the groin area, whether or not it has grown larger, and how much pain the patient is experiencing. The doctor will palpate the area, looking for any abnormal bulging or mass, and may ask the patient to cough or strain in order to see and feel the hernia more easily. This may be all that is needed to diagnose an inguinal hernia. To confirm the presence of the hernia, an ultrasound examination may be performed. The ultrasound scan will allow the doctor to visualize the hernia and to make sure that the bulge is not another type of abdominal mass such as a tumor or enlarged lymph gland. It is not usually possible to determine whether the hernia is direct or indirect until surgery is performed.
Preparation
Patients will have standard preoperative blood and urine tests, an electrocardiogram, and a chest x ray to make sure that the heart, lungs, and major organ systems are functioning well. A week or so before surgery, medications may be discontinued, especially aspirin or anticoagulant (blood-thinning) drugs. Starting the night before surgery, patients must not eat or drink anything. Once in the hospital, a tube may be placed into a vein in the arm (intravenous line) to deliver fluid and medication during surgery. A sedative may be given to relax the patient.
Aftercare
The hernia repair site must be kept clean and any sign of swelling or redness reported to the surgeon. Patients should also report a fever, and men should report any pain or swelling of the testicles. The surgeon may remove the outer sutures in a follow-up visit about a week after surgery. Activities may be limited to non-strenuous movement for up to two weeks, depending on the type of surgery performed and whether or not the surgery is the first hernia repair. To allow proper healing of muscle tissue, hernia repair patients should avoid heavy lifting for six to eight weeks after surgery. The postoperative activities of patients undergoing repeat procedures may be even more restricted.
Prevention of indirect hernias, which are congenital, is not possible. However, preventing direct hernias and reducing the risk of recurrence of direct and indirect hernias can be accomplished by:
- maintaining body weight suitable for age and height
- strengthening abdominal muscles through regular exercise
- reducing abdominal pressure by avoiding constipation and the build-up of excess body fluids, achieved by adopting a high-fiber, low-salt diet
- lifting heavy objects in a safe, low-stress way, using arm and leg muscles
Risks
Hernia surgery is considered to be a relatively safe procedure, although complication rates range from 1–26%, most in the 7–12% range. This means that about 10% of the 700,000 inguinal hernia repairs each year will have complications. Certain specialized clinics report markedly fewer complications, often related to whether open or laparoscopic technique is used. One of the greatest risks of inquinal hernia repair is that the hernia will recur. Unfortunately, 10–15% of hernias may develop again at the same site in adults, representing about 100,000 recurrences annually. The risk of recurrence in children is only about 1%. Recurrent hernias can present a serious problem because incarceration and strangulation are more likely and because additional surgical repair is more difficult than the first surgery. When the first hernia repair breaks down, the surgeon must work around scar tissue as well as the recurrent hernia. Incisional hernias, which are hernias that occur at the site of a prior surgery, present the same circumstance of combined scar tissue and hernia and even greater risk of recurrence. Each time a repair is performed, the surgery is less likely to be successful. Recurrence and infection rates for mesh repairs have been shown in some studies to be lower than with conventional surgeries.
Complications that can occur during surgery include injury to the spermatic cord structure; injuries to veins or arteries, causing hemorrhage; severing or entrapping nerves, which can cause paralysis; injuries to the bladder or bowel; reactions to anesthesia; and systemic complications such as cardiac arrythmias, cardiac arrest, or death. Postoperative complications include infection of the surgical incision (less in laparoscopy ); the formation of blood clots at the site that can travel to other parts of the body; pulmonary (lung) problems; and urinary retention or urinary tract infection.
Normal results
Inguinal hernia repair is usually effective, depending on the size of the hernia, how much time has gone by between its first appearance and the corrective surgery, and the underlying condition of the patient. Most first-time hernia repair procedures will be one-day surgeries, in which the patient will go home the same day or in 24 hours. Only the most challenging cases will require an overnight stay. Recovery times will vary, depending on the type of surgery performed. Patients undergoing open surgery will experience little discomfort and will resume normal activities within one to two weeks. Laparoscopy patients will be able to enjoy normal activities within one or two days, returning to a normal work routine and lifestyle within four to seven days, with the exception of heavy lifting and contact sports.
Morbidity and mortality rates
Mortality related to inguinal hernia repair or postoperative complications is unlikely, but with advanced age or severe underlying conditions, deaths do occur. Recurrence is a notable complication and is associated with increased morbidity, with recurrence rates for indirect hernias from less than 1–7% and 4–10% for direct.
Alternatives
If a hernia is not surgically repaired, an incarcerated or strangulated hernia can result, sometimes involving life-threatening bowel obstruction or ischemia.
Resources
books
Maddern, Guy J. Hernia Repair: Open vs. Laparoscopic approaches. London: Churchill Livingstone, 1997.
organizations
American College of Surgeons (ACS), Office of Public Information. 633 North Saint Clair Street, Chicago, IL 60611-3211. (312) 202-5000. http://www.facs.org .
The National Digestive Diseases Information Clearinghouse (NIDDK). 2 Information Way, Bethesda, MD 20892-3570. http://www.niddk.nih.gov/health/digest/nddic.htm .
other
"Focus on Men's Health: Hernia." MedicineNet Home Jan. 2003. http://www.medicinenet.com .
"Inguinal Hernia." Healthwise, Inc. February 2001. http://www.laurushealth.com/library. .
L. Lee Culvert
WHO PERFORMS THE PROCEDURE AND WHERE IS IT PERFORMED?
Inguinal hernia repair is performed in a hospital operating room or one-day surgical facility by a general surgeon who may specialize in hernia surgery.
QUESTIONS TO ASK THE DOCTOR
- What procedure will be performed to correct my hernia?
- What is your experience with this procedure? How often do you perform this procedure?
- Why must I have the surgery now rather than waiting?
- What are my options if I do not have the surgery?
- How can I expect to feel after surgery?
- What are the risks involved in having this surgery?
- How quickly will I recover? When can I return to school or work?
- What are my chances of having another hernia?
1. if the previous operation note, if available, says there is no indirect sac.
2. if the previous operation note is not mentioning anything abou an indirect sac.
3. if, during exploration the sac is a complete one.
4. if, the cord appears "virgin".
If the sac is thick at the summit, if it has fat along with it all along, or if the note says that the "indirect sac excised" then only I will consider it as a true recurrence.
Regarding the problem raised by Christine Gaubart, I wish to add that this is not an uncommon complication. This swelling is due to the cremasteric muscle getting contracted at the root of the scrotum when one has explored the cord for indirect sac.If the cremasteric muscle is excised in toto or carefully repaired over the cord this complication can be prevented.
Thanks.
Many thanks
Diane
Alonso
Thanks a lot for preparing this document so clearly.
thanks, mildred yu
This is a great piece of writing. It truly is. I have scoured the web for this information. This should be at the top of ALL hernia searches.
Nothing was missed. But it is rather a shock that so many people get hernias. I got a hernin lifting a heavy object. My hernis is small and I pop it back in. But it has changed my sex life. How can I have sex with a hernia? Nobody talks about this. When I take off my hernia belt to have a shower I have to press my belly to keep it in. I am very sad. But also this: If I continue to control it, keep thin, and take care of my body, MUST I still have a hernia operation?
THis is a great article. It really is!
Well, done.
This is a great piece of writing. It truly is. I have scoured the web for this information. This should be at the top of ALL hernia searches.
Nothing was missed. But it is rather a shock that so many people get hernias. I got a hernin lifting a heavy object. My hernis is small and I pop it back in. But it has changed my sex life. How can I have sex with a hernia? Nobody talks about this. When I take off my hernia belt to have a shower I have to press my belly to keep it in. I am very sad. But also this: If I continue to control it, keep thin, and take care of my body, MUST I still have a hernia operation?
THis is a great article. It really is!
Well, done.
I have learned that you should never sleep in your hernia belt. This is because the tight-belt pinches you back nerve when you lie down flat. And this is really worrying and super painful. But now I have told you, I think you can avoid it, although I am not a doctor. Also you have to wash your hernia belt every day or you begin to smell of urine, although you don't know it.
Also, sorry about my spelling.
chris Addlestone Surrey
Curious,
Erin
My 10 week old son is going to be having surgery to repair an indirect hernia in a few days, and needless to say, I'm a very nervous for him. Having information, and knowing what to expect helps out a little though.
Thanks all
Antibiotics are given; does that mean probiotics (nutritional supplement) should be curtailed?
Yours,
Laurence
is it true that there is a possibility that after a hernia surgery, there is a less chance of having a baby?
I had hernia surgery before a week but there is something hard thing in my ball.
I'm very afraid. Pls tell me something pls pls pls
The article is amazing...but as a human nature thing one is always more concerned about her or himself.
I had an indirect inguinal hernia repair due to swelled left testicle. Undergone, the surgery already, i was told by the surgeon that it would take 15 days for the swelling to be normal because of fluids to be passed out. Its been 2 months now (8 weeks) but the swelling hasnt gone. Though it has reduced but its not completly gone and i am having a little pain on the groin area again.
Require help for this.
Thanks
under 50 lbs ok ? but I do more pulling and pushing during the time
I use my floor machine. getting it in to my van of course use a ramp ?
Thank You