Gastrectomy
Definition
Gastrectomy is the surgical removal of all or part of the stomach.
Purpose
Gastrectomy is performed most commonly to treat the following conditions:
- stomach cancer
- bleeding gastric ulcer
- perforation of the stomach wall
- noncancerous polyps
Demographics
Stomach cancer was the most common form of cancer worldwide in the 1970s and early 1980s, and the incidence rates have always shown substantial variation in different countries. Rates are currently highest in Japan and eastern Asia, but other areas of the world have high incidence rates, including Eastern European countries and parts of Latin America. Incidence rates are generally lower in Western Europe and the United States.
Gastrointestinal diseases (including gastric ulcers) affect an estimated 25–30% of the world's population. In the United States, 60 million adults experience gastrointestinal reflux at least once a month, and 25 million adults suffer daily from heartburn, a condition that may evolve into ulcers.
Description
Gastrectomy for cancer
Removal of the tumor, often with removal of the surrounding lymph nodes, is the only curative treatment for various forms of gastric (stomach) cancer. For many patients, this entails removing not only the tumor, but part of the stomach as well. The extent to which lymph nodes should also be removed is a subject of debate, but some studies show additional survival benefits associated with removal of a greater number of lymph nodes.
Gastrectomy, either total or subtotal (also called partial), is the treatment of choice for gastric adenocarcinomas, primary gastric lymphomas (originating in the stomach), and the rare leiomyosarcomas (also called gastric sarcomas). Adenocarcinomas are by far the most common form of stomach cancer and are less curable than the relatively uncommon lymphomas, for which gastrectomy offers good chances of survival.
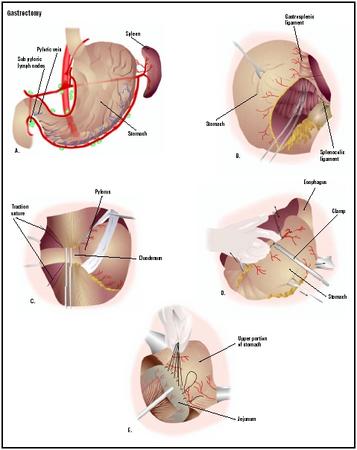
General anesthesia is used to ensure that the patient does not experience pain and is not conscious during the operation. When the anesthesia has taken hold, a urinary catheter is usually inserted to monitor urine output. A thin nasogastric tube is inserted from the nose down into the stomach. The abdomen is cleansed with an antiseptic solution. The surgeon makes a large incision from just below the breastbone down to the navel. If the lower end of the stomach is diseased, the surgeon places clamps on either end of the area, and that portion is excised. The upper part of the stomach is then attached to the small intestine. If the upper end of the stomach is diseased, the end of the esophagus and the upper part of the stomach are clamped together. The diseased part is removed, and the lower part of the stomach is attached to the esophagus.
After gastrectomy, the surgeon may reconstruct the altered portions of the digestive tract so that it may continue to function. Several different surgical techniques are used, but, generally speaking, the surgeon attaches any remaining portion of the stomach to the small intestine.
Gastrectomy for gastric cancer is almost always done using the traditional open surgery technique, which requires a wide incision to open the abdomen. However, some surgeons use a laparoscopic technique that requires only a small incision. The laparoscope is connected to a tiny video camera that projects a picture of the abdominal contents onto a monitor for the surgeon's viewing. The stomach is operated on through this incision.
The potential benefits of laparoscopic surgery include less postoperative pain, decreased hospitalization, and earlier return to normal activities. The use of laparoscopic gastrectomy is limited, however. Only patients with early-stage gastric cancers or those whose surgery is intended only for palliation (pain and symptomatic relief rather than cure) are considered for this minimally invasive technique. It can only be performed by surgeons experienced in this type of surgery.
Gastrectomy for ulcers
Gastrectomy is also occasionally used in the treatment of severe peptic ulcer disease or its complications. While the vast majority of peptic ulcers (gastric ulcers in the stomach or duodenal ulcers in the duodenum) are managed with medication, partial gastrectomy is sometimes required for peptic ulcer patients who have complications. These include patients who do not respond satisfactorily to medical therapy; those who develop a bleeding or perforated ulcer; and those who develop pyloric obstruction, a blockage to the exit from the stomach.
The surgical procedure for severe ulcer disease is also called an antrectomy , a limited form of gastrectomy in which the antrum, a portion of the stomach, is removed. For duodenal ulcers, antrectomy may be combined with other surgical procedures that are aimed at reducing the secretion of gastric acid, which is associated with ulcer formation. This additional surgery is commonly a vagotomy , surgery on the vagus nerve that disables the acid-producing portion of the stomach.
Diagnosis/Preparation
Before undergoing gastrectomy, patients require a variety of such tests as x rays, computed tomography (CT) scans, ultrasonography, or endoscopic biopsies (microscopic examination of tissue) to confirm the diagnosis and localize the tumor or ulcer. Laparoscopy may be done to diagnose a malignancy or to determine the extent of a tumor that is already diagnosed. When a tumor is strongly suspected, laparoscopy is often performed immediately before the surgery to remove the tumor; this method avoids the need to anesthetize the patient twice and sometimes avoids the need for surgery altogether if the tumor found on laparoscopy is deemed inoperable.
Aftercare
After gastrectomy surgery, patients are taken to the recovery unit and vital signs are closely monitored by
Risks
Surgery for peptic ulcer is effective, but it may result in a variety of postoperative complications. Following gastrectomy surgery, as many as 30% of patients have significant symptoms. An operation called highly selective vagotomy is now preferred for ulcer management, and is safer than gastrectomy.
After a gastrectomy, several abnormalities may develop that produce symptoms related to food intake. They happen largely because the stomach, which serves as a food reservoir, has been reduced in its capacity by the surgery. Other surgical procedures that often accompany gastrectomy for ulcer disease can also contribute to later symptoms. These procedures include vagotomy, which lessens acid production and slows stomach emptying; and pyloroplasty , which enlarges the opening between the stomach and small intestine to facilitate emptying of the stomach.
Some patients experience lightheadedness, heart palpitations or racing heart, sweating, and nausea and vomiting after a meal. These may be symptoms of "dumping syndrome," as food is rapidly dumped into the small intestine from the stomach. Dumping syndrome is treated by adjusting the diet and pattern of eating, for example, eating smaller, more frequent meals and limiting liquids.
Patients who have abdominal bloating and pain after eating, frequently followed by nausea and vomiting, may have what is called the "afferent loop syndrome." This is treated by surgical correction. Patients who have early satiety (feeling of fullness after eating), abdominal discomfort, and vomiting may have bile reflux gastritis (also called bilious vomiting), which is also surgically correctable. Many patients also experience weight loss.
Reactive hypoglycemia is a condition that results when blood sugar levels become too high after a meal, stimulating the release of insulin, occurring about two hours after eating. A high-protein diet and smaller meals are advised.
Ulcers recur in a small percentage of patients after surgery for peptic ulcer, usually in the first few years. Further surgery is usually necessary.
Vitamin and mineral supplementation is necessary after gastrectomy to correct certain deficiencies, especially vitamin B 12 , iron, and folate. Vitamin D and calcium are also needed to prevent and treat the bone problems that often occur. These include softening and bending of the bones, which can produce pain and osteoporosis, a loss of bone mass. According to one study, the risk for spinal fractures may be as high as 50% after gastrectomy.
Normal results
Overall survival after gastrectomy for gastric cancer varies greatly by the stage of disease at the time of surgery. For early gastric cancer, the five-year survival rate is as high as 80–90%; for late-stage disease, the prognosis is bad. For gastric adenocarcinomas that are amenable to gastrectomy, the five-year survival rate is 10–30%, depending on the location of the tumor. The prognosis for patients with gastric lymphoma is better, with five-year survival rates reported at 40–60%.
Most studies have shown that patients can have an acceptable quality of life after gastrectomy for a potentially curable gastric cancer. Many patients will maintain a healthy appetite and eat a normal diet. Others may lose weight and not enjoy meals as much. Some studies show that patients who have total gastrectomies have more disease-related or treatment-related symptoms after surgery and poorer physical function than patients who have subtotal gastrectomies. There does not appear to be much difference, however, in emotional status or social activity level between patients who have undergone total versus subtotal gastrectomies.
Morbidity and mortality rates
Depending on the extent of surgery, the risk for postoperative death after gastrectomy for gastric cancer has been reported as 1–3% and the risk of non-fatal complications as 9–18%. Overall, gastric cancer incidence and mortality rates have been declining for several decades in most areas of the world.
Resources
books
"Disorders of the Stomach and Duodenum." In The Merck Manual. Whitehouse Station, NJ: Merck & Co., Inc., 1992.
"Stomach and Duodenum: Complications of Surgery for Peptic Ulcer Disease." In Sleisenger & Fordtran's Gastrointestinal and Liver Disease, edited by Mark Feldman et al. Philadelphia: W. B. Saunders Co., 1998.
periodicals
Fujiwara, M., et al. "Laparoscopy-Assisted Distal Gastrectomy with Systemic Lymph Node Dissection for Early Gastric Carcinoma: A Review of 43 Cases." Journal of the American College of Surgeons 196 (January 2003): 75–81.
Iseki, J., et al. "Feasibility of Central Gastrectomy for Gastric Cancer." Surgery 133 (January 2003): 75–81.
Kim, Y. W., H. S. Han, and G. D. Fleischer. "Hand-Assisted Laparoscopic Total Gastrectomy." Surgical Laparoscopy, Endoscopy & Percutaneous Techniques 13 (February 2003): 26–30.
Kono, K., et al. "Improved Quality of Life with Jejunal Pouch Reconstruction after Total Gastrectomy." American Journal of Surgery 185 (February 2003): 150–154.
organizations
American College of Gastroenterology. 4900-B South 31st St., Arlington, VA 22206. (703) 820-7400. http://www.acg.gi.org .
American Gastroenterological Association (AGA). 4930 Del Ray Avenue, Bethesda, MD 20814. (301) 654-2055. http://www.gastro.org .
Caroline A. Helwick
Monique Laberge, PhD
WHO PERFORMS THE PROCEDURE AND WHERE IS IT PERFORMED?
A gastrectomy is performed by a surgeon trained in gastroenterology, the branch of medicine that deals with the diseases of the digestive tract. An anesthesiologist is responsible for administering anesthesia, and the operation is performed in a hospital setting.
QUESTIONS TO ASK THE DOCTOR
- What happens on the day of surgery?
- What type of anesthesia will be used?
- How long will it take to recover from the surgery?
- When can I expect to return to work and/or resume normal activities?
- What are the risks associated with a gastrectomy?
- How many gastrectomies do you perform in a year?
- Will there be a scar?
how can he survive and what type of life can he exspect.
Your help will be greatly appreciated.
Your help will be greatly appreciated.
the medical report was:
A gastric carcinoma, already metastasized to the extra-perigastric lymph node. Studies showed a small depressed lesion on the lesser curvature of the antrum and histology of the biopsied specimen revealed a well differentiated adenocarcinoma. Under the diagnosis of IIIc type intramucosal carcinoma, partial gastrectomy and wide lymph node dissection was performed. Pathologic study of the resected specimen showed that the cancer cells had invaded the submucosa at an area via a lymphatic vessel and that only lymph node along the common hepatic artery was involved.
if somebody can help me i will appreciate it.
Regards
Helen
in a pt. with a fully removed stomach, what do u expect this pt. will develop regarding his/her RBC count? and when after the operation?
and how do u treat him and why ?
thanks.
Sometimes, leaving well enough alone is the answer. In my case, if I hadn't had a spell of vomiting blood, no one would have known about the cancer. I may survive 15 years going along like I have been and having a relatively good life. Why does western medicine feel they have "to cut stuff out" as the first solution. There are reasons that this happened in the first place(lifestyle and incorrect eating/drinking are foremost) but can't this stuff be treated otherwise with root cause solutions? I am having less & less faith in our North American doctors and their way of treatment - they mostly are closed minded to to other forms of treatment and do not acknowledge or work with other trained practitioners, not only in this situation but with other minor day-to-day problems. I think that the Pharmaceutical companies have them roped -all due to making money and the patients are at their mercy. If there is a cure, nobody can sell drugs and then nobody makes any money!My current situation is making me crazy and anxious(not a good way to go into surgery) and also depressed - like there is no hope. Please give me something to hang onto that is positive and encouraging.
John
DEN ME AND I WANT YOUR OPINION ON THIS.
AN INDIVIDUAL 50 YEARS THAT pale, underweight, say they have undergone a surgery in which he had lost part of the stomach and the chief cells. he ordered laboratory tests which report the following resultados.hemoglobina low colipase activity greatly diminished, parietal cell atrophy.
questions
to be low weight?
as is the digestion and absorption of lipids Why?
protein digestion and intestinal gastric level and is why?
I hope your answer and sorry for the inconvenience
COLOMBIA,BARRANQUILLA
In many ways things eventually (like 2 years) improved. It took about four months to get them to take the feeding peg out. My weight went down to 85 pounds. In December 2008 my doctors worst nightmare happened, I found out I was pregnant(this was so not planned). They told me that I couldn't carry a pregnancy. I felt I had to try and after hearing a heart beat on my husbands birthday on christmas eve, I knew I had to. The strangest thing is that I was so healthy during my pregnancy. I had the best medical care and the insurance company who had been previously denying to pay any claims had to cover me while pregnant. I had iron infusions which I had never heard of. My specialist said that a womans digestive system slows during pregnancy so I was finally aborbing nutrients and taking lots of vitamins. I carried her to 38weeks and was induced giving birth to a perfect healthy little girl who just turned two. She is my miracle and makes me laugh every day even when some of those days are not so good.
Unfortunately the reactive hypoglycemia has returned and I have to be very careful or I will have seizures. I have just recently been hospitalized with abdominal pain following a bout of vomittin, I still have dumping syndrome. I was transfered from the hospital I was in to the Cleveland Clinic where I stayed for another week. I had a pic line and 24 TPM. Didn't really get clear answers aside from I have alot of lesions, adhesions and scar tissue. I am home now yet barely able to eat without vomitting which really hurts. I have followup with one of the cleveland Doctors soon and hope to have answers but feel another nightmare is just beginning. Trying to stay positive.
I too am leading up to a total Gastectomy. I have had all of the feelings that you have described to the letter.
A year ago I was 220 lbs of rock solid weight lifting linebacker. Now I'm 179 lbs and dropping with my wardrobe all but swapped out for mediums.
After 6 months of avoiding the warning signs of pain after eating and a doctors warning that I had stomach cancer, I tried a natural route for 5 weeks of carrot juice and a special diet.
But with my stomach swelling almost to the point of covering my Pyloris on my last Endiscopy, The Homeopathic Christian that sold me on the diet tells me that it has to swell before it gets better. Well, I can't take the chance any longer.
I'm undergoing the last of my blood & barium scans etc and then I will probably get my self gutted like a fish. And I am on board with you that why would I ever want to do this to myself and subject myself to all of the above pain and suffering.
I can barely eat now without pain so whats have I got to lose. My other reason to live is a my son. If not for him and my wife, I'd go as far as I could and pull the trigger on my 9.
Pretty sure life is gonna suck if I do this but if I'm lucky I can meditate my way through it. If not, There's always a round in the chamber.
Life's not fair sometimes and these are the cards I've been dealt. I didn't care so much when I was swilling a 5th of Jim Beam a night and eating a steak at 2 in the morning. Life was good.
At 49 I often reflect back on what my father always said, If I only knew then what I know now.
Good luck to all.
It is still a very scary thought as my surgery will be in about 2-3 weeks time, and i have never had surgery before. When I read about the post-op adjustments that have to be made, it seems too much to bear. But the decision came from within me - trusting ones intuition will always lead to the correct action. And I am now wanting to go on with my life without this hanging over my head.
For all who have been through this, thank you for sharing your stories - they are so valuable to people like me. To those who are still going to have their 'adventure', may everything go perfectly well.
Praying that we are ALL healthy and HAPPY!
1. Do not drink after eating for at least 1/2 an hour and wait 1/2 hour after drinking before eating.
2. Stay away from fatty foods, highly refined foods (eg cake and white bread, high carbs) and food with lots of sugar.
3. Yes, eating lots of small meals a day is frustrating but I cope now as single mum of a teenager and working fulltime. The day I was able to eat 2 whole poached eggs was a celebration!!
4. When eating, do it slowly and chew everything very well.
5. Do not expect to much from yourself. Losing your stomach and adapting is a huge learning curve.
6. Gastric dumping is awful and can be very debilitating. There are varying degrees of gastric dumping - mild (feeling tired) to severe with dizziness, severe vomiting, awful stomach cramping and diahorrea.
7. I have found that one of the best ways reduce the effect of dumping is to lay down - this slows the process of the food passing through your intestines. Dumping is basically the body working to get rid of the food quickly and it can happen just after a meal or a few hours later. For me its usually because I have eaten a bit to much or had something I should not have. Remember that one extra mouthful can push you over the edge. It takes time to know how much you can tolerate in a meal. See the wikipedia site for more information on gastric dumping syndrome.
Because this only lets me put in a maximum of 4000 characters I will do this in 2 parts - see more below.
9. See your dietician regularly, the information they have is invaluable. I see mine every 3 months now, mainly just to monitor my weight.
10. Vitamin supplements are now essential for me. Daily I take a multi vitamin and iron tablet. Every three months I have a B12 injection (by the time 3 months is up I know I need it).
11. Stay positive, say I am not going to let this beat me, ok that food did not suit me what else can I try now. Look for solutions and I know, some days its hard to be positive.
12. I now cook a number of casserole or stew type meals with lots of different vegetables and often throw in a handful of chick peas or lentils. This softens all the foods - it is difficult to impossible for the duodenal to absorb nutrients from some raw vegetables.
13. One of my favourite meals is made in muffin tins. I line them with puff pastry and fill with pre cooked minced pork & veal, lots of chopped vegetables, one egg to bind it, sweet chilli sauce and tomato sauce. Cook them for about 25 mins in the oven. Two of these are a great meal, taste great and are good for me. Generally I make about 24 and this only takes a few sheets of puff pastry. I cut each sheet into 9 pieces and they fit nicely into the muffin tin.
14. Have lots of different meals in the freezer, its just so handy to pull something nice out.
15. My food of a day is usually; Porridge with milk (buy one of those nice flavoured ones but not with to much sugar), cup of tea, wedge of brie cheese, cup of coffee, banana, cup of tea, lunch (usually one of my frozen meals - stew etc), glass of water, apple (chew this very well), cup of tea, dinner (I make the meal as I would have done pre surgery and freeze the remainder), yoghurt and then warm milk before going to bed.
16. I find that I cannot drink or eat anything that is icy cold. Plus, if I have too much in the way of milk products the new stomach system lets me know its uncomfortable.
GOOD LUCK ALL.
my husbud was suffering from a serious gastric ulcer, his Doctor has remover the part which was bleeding just befor a month but till now he didn't get any relief, and also I need ur recomendation as what are the diet given to him after this operation. thank you
Anybody can suggest some diet for him to increase weight? My dad is taking vitamins supplements such as folic acid, ferrous for his blood, zinc, vit B, Vit B-12 injection once a month and vit C also.
Kindly advise me...
I am eating solid foods, yes in small quantities, several times a day, and tolerating it well. I have not experienced dumping syndrome. My only problem now is that I have contacted pneumonia, a condition though treatable and curable has left me very discouraged. This gastrectomy was my second procedure for gastric cancer. I had a partial gastrectomy in 2007 for gastric cancer. At that time I was told that all surrounding areas were cancer free. This year I was told the same, that all surrounding lymphnodes were clear. As I said, very discouraging.
How to meassure these complications accurately?
Thank you.
Dr. Francisco Fonseca
There appears to be no magic formula for if/when I would develop cancer. My surgeon has indicated to me that if I was 75+ years old or in poor health, she would just recommend enjoying your remaining time and hope for the best rather than risking dying on the operating table having a gastrectomy.
While there are a number of potential complications, my surgeon (and another second-opinion surgeon) express optimism that while it may take 6 months and dietary changes, I should be able to return to some semblance of normalcy (work, mobility, independence).
However, it's hard to make such huge decisions with so much "grey" areas. I'm extremely lucky to not have cancer (at least yet), but it is difficult to come to terms to accept a gastrectomy for future risk when I presently am reasonably healthy.
Thanks to all who have shared their experiences and my best wishes for your future health.
For me I have had difficulty eating which seems to be common and difficulty sleeping more then a few hours at a time. As far as eating goes I eat small portions, very slowly, chewing lots. After the first little bit goes down a few minutes later the pain starts as well as the burping. ONce that passes I can eat more and the process repeats. The difficulty sleeping is what may drive me over the edge. IN the last 6 years I haven't had a solid nights sleep cause of the nausea I experience after sleeping a few hours. I use an adjustable bed so I am propped up and have tried all sorts of meds and eating patterns but nothing has worked thus far.
There is certainly an emotional drain going through the cancer diagnosis, chemo, radiation, surgery and recovery, but that is to be expected. Patients and their caregivers ought to seek counseling from the very start to avoid problems; much better than waiting for depression, anxiety or other problems to develop. I suggest going to a cancer center of excellence if possible. They are listed on the National Cancer Institute website.