Endoscopic sinus surgery
Definition
Functional endoscopic sinus surgery (FESS) is a minimally invasive surgical procedure that opens up sinus air cells and sinus ostia (openings) with an endoscope.
The use of FESS as a sinus surgical method has now become widely accepted; and the term "functional" is meant to distinguish this type of endoscopic surgery from nonendoscopic, more conventional sinus surgery procedures.
Purpose
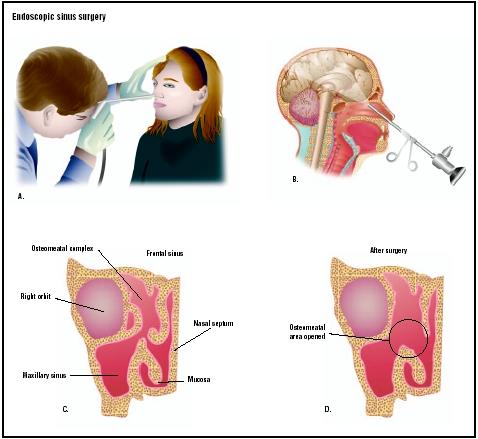
The purpose of FESS is to restore normal drainage of the sinuses. Normal function of the sinuses requires ventilation through the ostia (mouth-like opening) and is facilitated by a mucociliary transport process that maintains a constant flow of mucus out of the sinuses. All sinuses need ventilation to prevent infection and inflammation, a condition known as sinusitis. In healthy individuals, sinus ventilation occurs through the ostia into the nose. The sinuses open into the middle meatus (curved passage in each nasal cavity) under the middle turbinate (thin, bony process that is the lower portion of the ethmoid bone in each nasal cavity), which together are known as the osteomeatal complex, the key area of the nose. The hair-like cilia direct the flow of mucus toward the ostia.
Sinusitis develops when there is a problem in the area where the maxillary and frontal sinuses meet near the nose or, occasionally, by dental infection. When sinusitis occurs, the cilia work less efficiently, preventing the flow of mucus. The mucous membranes of the sinuses become engorged, resulting in ostia closure. Poor ventilation and accumulation of mucus then produce the conditions required for bacterial infection.
Demographics
Sinusitis is a very common condition, affecting 31 million Americans each year; 30% of the United States population have sinusitis at some point in their lives. The average adult has three to four upper respiratory infections a year; 1% of these infections are complicated by sinusitis, accounting for 16 million visits to the doctor each year.
Description
After inducing adequate vasoconstriction with cocaine or ephedrine, the surgeon locates the middle turbinate, the most important landmark for the FESS procedure. On the side of the nose at the level of the middle turbinate lies the uncinate process, which the surgeon removes. The surgeon opens the back ethmoid air cells, to allow better ventilation, but leaves the bone covered with the mucous membrane. Following this step, the ostium located near the jaw is checked for obstruction and, if necessary, opened with a middle meatal antrostomy. This surgical procedure often greatly improves the function of the osteomeatal complex and provides better ventilation of the sinuses.
FESS offers several advantages:
- It is a minimally invasive procedure.
- It does not disturb healthy tissue.
- It is performed in less time with better results.
- It minimizes bleeding and scarring.
Diagnosis/Preparation
As with many diseases, the history of a patient with sinusitis represents a key part of the preoperative evaluation. Before considering FESS, the ear, nose and throat (ENT) specialist will proceed with a thorough diagnostic examination. The development of such diagnostic tools as the fiberoptic endoscope and CT scanning has greatly improved the treatment of sinus disease. The fiberoptic endoscope is used to examine the nose and all its recesses thoroughly. The specific features the physician must examine and evaluate are the middle turbinate and the middle meatus, any anatomic obstruction, and the presence of pus and nasal polyps.
CT scanning can also be used to identify the diseased areas, a process that is required for planning the surgery. It shows the extent of the affected sinuses, as well as any abnormalities that may make a patient more susceptible to sinusitis.
FESS is usually performed under local anesthesia with intravenous sedation on an outpatient basis with patients going home one to two hours after surgery. It usually does not cause facial swelling or bruising, and does not generally require nasal packing.
Aftercare
FESS usually does not cause severe postoperative sinus pain. After the procedure, it is important to keep the nose as free from crust build-up as possible. To achieve this, the surgeon may perform a lengthy cleaning two to three times per week or the patient may perform a simple nasal douching several times a day. Normal function usually reappears after one or two months. In patients with severe sinusitis or polyps, a short course of systemic steroids combined with antibiotics may quicken recovery.
Risks
The most serious risk associated with FESS is blindness resulting from damage to the optic nerve. The chances of this complication occurring, however, are extremely low. Cerebrospinal fluid leak represents the most common major complication of FESS, but it occurs in only about 0.2% of cases in the Unites States. The leak is usually recognized at the time of surgery and can easily be repaired. Other less serious and rare complications include orbital hematoma and nasolacrimal duct stenosis. All of these complications are also associated with conventional sinus surgery and not only with FESS.
Normal results
The FESS procedure is considered successful if the patient's sinusitis is resolved. Nasal obstruction and facial pain are usually relieved. The outcome has been compared with that of the Caldwell-Luc procedure and, although both methods are considered effective, there is a strong patient preference for FESS. The extent of the disease before surgery dictates the outcome, with the best results obtained in patients with limited nasal sinusitis.
Morbidity and mortality rates
According to the American Academy of Family Physicians (AAFP), FESS usually has a good outcome, with most studies reporting an 80–90% rate of success. Good results have also been obtained in patients who have had previous sinus surgery.
Alternatives
- Image-guided endoscopic surgery. This method uses image guidance techniques that feature a three-dimensional mapping system combining CT scanning and real-time data acquisition concerning the location of the surgical instruments during the procedure. It allows surgeons to navigate more precisely in the affected area. The surgeon can monitor the exact location of such vital organs as the brain and eyes as well as positively identifying the affected areas.
- Caldwell-Luc procedure. This procedure is directed at improving drainage in the maxillary sinus region located below the eye. The surgeon reaches the region through the upper jaw above one of the second molars. He or she creates a passage to connect the maxillary sinus to the nose in order to improve drainage.
Resources
books
Bhatt, N. J. Endoscopic Sinus Surgery: New Horizons. Independence, KY: Singular Publishing Group, 1997.
Bhatt, N. J. The Frontal Sinus: Advanced Surgical Techniques. Independence, KY: Singular Publishing Group, 2002.
Marks, S. C., and W. A. Loechel. Nasal and Sinus Surgery. Philadelphia: W. B. Saunders Co., 2000.
periodicals
Engelke, W., W. Schwarzwaller, A. Behnsen, and H. G. Jacobs. "Subantroscopic laterobasal sinus floor augmentation (SALSA): an up-to-5-year clinical study." International Journal of Oral and Maxillofacial Implants 18 (January-February 2003): 135–143.
Graham, S. M., and K. D. Carter. "Major complications of endoscopic sinus surgery: a comment." British Journal of Ophthalmology 87 (March 2003): 374–377.
Larsen, A. S., C. Buchwald, and S. Vesterhauge. "Sinus baro trauma—late diagnosis and treatment with computeraided endoscopic surgery." Aviation & Space Environmental Mediciine 74 (February 2003): 180–183.
Ramadan, H. H. "Relation of age to outcome after endoscopic sinus surgery in children." Archives of Otolaryngology & Head and Neck Surgery 129 (February 2003): 175–177.
Wormald, P. J. "Salvage frontal sinus surgery: the endoscopic modified Lothrop procedure." Laryngoscope 113 (February 2003): 276–283.
organizations
American Academy of Otolaryngology-Head and Neck Surgery. One Prince St., Alexandria, VA 22314-3357. (703) 836-4444. http://www.entnet.org/ .
Association for Research in Otolaryngology. 19 Mantua Rd., Mt. Royal, NJ 08061. (856) 423-0041. (301) 733-3640. http://www.aro.org/index.html .
North American Society for Head and Neck Pathology. Department of Pathology, H179, P.O. Box 850, Milton S. Hershey Medical Center, Penn State University School of Medicine, Hershey, PA 17033. (717) 531-8246. http://www.headandneckpathology.com/ .
other
"Factsheet: Sinus Surgery." American Academy of Otolaryn gology—Head and Neck Surgery [cited May 5, 2003]. http://www.entlink.org/healthinfo/sinus/sinus_surgery.cfm .
Slack, R. and G. Bates. "Sinus Surgery." American Family Physician . 1 September 1998 [cited May 5, 2003]. http://www.aafp.org/afp/980901ap/slack.html .
Monique Laberge, Ph.D.
WHO PERFORMS THE PROCEDURE AND WHERE IS IT PERFORMED?
This procedure is usually performed on an outpatient basis by an ear, nose, and throat (ENT) specialist, such as an otolaryngologist or an ophthalmic surgeon. ENT physicians are graduates of a school of medicine and typically undergo an otolaryngology residency with further specialization in sinus disease and endoscopic sinus surgery.
QUESTIONS TO ASK THE DOCTOR
- Why is sinus surgery required?
- What are the risks involved?
- How many endoscopic sinus surgery procedures do you perform in a year?
- How much time will I need to recover from the procedure?
- Is the procedure painful?
- What are the alternatives?
i have problem of post nasal drip and allergic rhinitis.
and also have nasal septum and large bone in my right nose.
can nasal surgery will be effected for me.
Regards
Zafar Iqbal
Thanks a lot!!!
I think you are the ringt one to ask.....My husband is having sever headaches every day.He had his maxillary sinus surgery in 2002.Now his frontal sinuses are blocked.But on the other hand he is not having any symtums of sinus like runny nose and watery eyes.Doctors told us to go for surgery,but are saying that they don,t think his headaches are related to sinus.They said there is 50-50 chances if his headaces will go off or get lesser... I am worring about the leakage risk during this surgery..pl.tell me percentage of that risk and also tell me if the surgery will help his headache??????
I do not have any benefit out of the surgery. Now I have to suffer all my life.
Sinustis was harmless for living. It was just temporaly situation when I had a cold simptom,I think.
Try alternative treatment without operation, I suggest you patients.
firnena.com/eng
Just trying to help. Because i know how suffer it is to let be operate and then not to have the right antidote to prevent it from breeding again.
I had surgery in 2001. The purpose was to remove polops by"scraping"
After the surgery I had severe and painful headaches. They went away after a few weeks, but they can recur anytime, especially after a bad cold or flu.
I still get them every few years and they are awful. I recently went to a neurologist and He was quite sure they are the result of sensitivity of the scar tissue. Apparently the situation is not curable.
Also my sense of smell has been terrible since the operation
Wish me luck all. I have seen the best I am told with Dr. David Kennedy at University of Pennsylvania. His staff was wonderful, extremely thorough and reviewed my scans and MRI even from 20 years ago. I feel VERY comfortable going into this surgery.
Any comments or helpful hints or suggestions to help me prepare for after care/post operative pain or help needed?
I was told no work for at least a week or two. Is this true? Has anyone seen this take that long?
Side effects other than above?
I wear contacts so hopefully my old glasses will work for me. I do not plan to drive and have taken the week off work to stay and get better.
Thanks all
For past 4 month I been very sick with headache, took all kinds of antibiotic and storied with no result. The cat scan showed upper left sinus blockage. My ent who is well known in NYC referred me to another ENT to do the surgery and open up the blockage. I would like to know if anyone has done this and what is the success rate? Also could anyone refer a good ENT in NYC area that specialized in upper sinius surgery.
Thank you
I have suffered from chronic sinusitis for many many years. At first it was treatable with antibiotics but due to the frequency of the infections I became allergic to the antibiotics. After that my ENT Dr began treating me with steroids in the step down dosage packs. This helped a lot but I did not want to have to take steroids so much. Finally he recommended that I have a septoplasty. That surgery was wonderful for the first 3 years, I had almost no sinus infection and I could breath for for the first time. The only issue I had at first was that the incision in my nostril never healed right the scar tissue would scab up and it would cause mild pain and pulling in my nostril. At year 3 I began having sinus infections again, not as bad as before the surgery but enough to be bothered by them. I also started getting upper respiratory infections with the sinus infections. The URI's were the worst. My ENT Dr explained that the septum has whats called memory and over time it can begin to revert to its original shape (my was in the shape of an S almost completely blocking one nostril). It is not 4 1/2 years since my septoplasty and its now very noticeable that my septum is curved, it has cause my nose to become crocked. I spoke with my ENT about the problem and she does not suggest redoing the surgery as it will weaken the septum which could cause me additional issues. I have consulted a plastic surgeon about having my nose restructured to aid in my breathing along with having the openings to my sinus fractured to widen them. I belive it is similar to FESS but I'm not exactly sure as the surgeon did not mention FESS during our consultation. Has any one had the openings to there sinus fractured to help with sinusitis?
Since FESS and Septaplasmy surgery last Aug, I have experienced the following complications:
Hole in Septum
More blocked on left side than previously
Severe dry/bluury eyes that I cannot get control of
loss of smell and taste
Ecoli od sinuses
Loud rattles nose with whistle
More catarrh than previously
Tinnitus
Vertigo
Painful Nerve damage to roof of mouth
Emotional shut down as trapped in a world of my own
Desperation for something to resolve
I live in the UK and although we have the benefit of NHS, I have to wait 4/5 months between consultant apps and so far nearly a year on I am getting worse and nothing being resolved.
I was perfectly healthy 48 year old woman before surgery who other than experiencing chronic catarrh and scans revealing diseased sinuses! I led a healthy and active life. I am trying to start up physical activity again but I am struggling big time and no one will take responsibility in helping. My GPni fell is despairing on my behalf. I currently take a steroid spray and decongestant for my nose and constant lubrication for my eyes with now trying heat pad therapy.
I would not recommend surgery unless is the last resort as has wrecked my life.
Any suggestions or shared experiences would help greatly.
Only consider FESS/Septaplasmy as last resort.
I had op a year ago and as a result have experienced the following complications:
Hole made in my Septum
Permanent nerve damage to the roof of my mouth
Ecoli infection in my nose
Tinnitus after the Ecoli infection that remains with me for 10 months now
Extremely dry/blurry eyes since post op day two
Worse congestion
Lost my smell
Lost my taste
Lost my emotions and something has now shut down on me
Vertigo
Unfortunately I was not for warned of any of this, which is why you need to know.
So if it is not life threatening or seriously affecting your life try any other alternative treatment eg. acupuncture etc
DO NOT RISK THE SURGERY!
i am having very major sinus problem my doctor said to me for FESS surgery for drainage nasal way but i am confused. it is 100% cure.
I Feel guilty for putting my son thru all this
If anyone out there is thinking about this surgery, do not do it! Doctors only care about money. I have never found one that actually cared about helping me.
What are the risks involved?
How many endoscopic sinus surgery procedures do you perform in a year?
How much time will I need to recover from the procedure?
Is the procedure painful?
What are the alternatives?
After surgery i was in agony for a while had lost alot of feeling around my face head and neck but i didnt see how my personalty and stuff had changed but i got back to my old self soon enough then i discovered i was still getting csf leaks got myself an appointment with surgeon who said it cant be his procedure worked so i collected some in a urine sample bottle and had them test it and it turned out to be csf got more scans discovered hole was still ther got put on emergency list for another procedure i waited 4 years and got surgery when i moved to scotland the surgery went well but i wasnt impressed with 3 very visible lumps on my forehead like horns had been cut off but was lead to believe would be less visible once things settled after a few weeks my head filled with fluid and a hard circle lump i had in middle of head had disslodged and got stuck on top of head few weeks later this lump of acrylic was removed now 10 years later i still get leaks but have had headache for weeks and my skull looks like it has caved in along what im assuming are previous surgery faults