Cyclocryotherapy
Definition
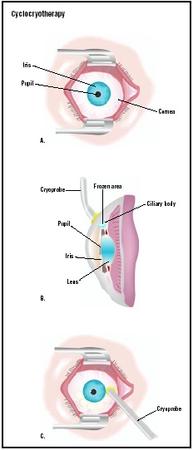
Cyclocryotherapy (CCT) is a procedure that employs temperatures as low as -112°F (-80°C) to destroy the ciliary body, an organ in the anterior chamber of the eye behind
Glaucoma is a general term used to describe a group of potentially blinding diseases, the main sign of which is a relatively high intraocular pressure. This increase in IOP causes damage to the optic nerve and the surrounding retinal tissue. In end-stage glaucoma, a patient's visual field is severely restricted. The increased intraocular pressure usually is caused by increased aqueous fluid in the eye. Treatment of glaucoma involves medical or surgical strategies to either increase the outflow of fluid from the eye, or to decrease the production of fluid in the eye, in an attempt to lower the IOP. The objective of glaucoma treatment is to attain an intraocular fluid level low enough such that damage to the optic nerve does not occur, yet is high enough such that the integrity of the eye is not sacrificed.
CCT is a last-resort treatment for patients in whom conventional medical and surgical techniques to control glaucoma have failed. Medical treatment involves the use of eyedrops that may be administered from one to four times a day. Surgical techniques are used to treat glaucoma when the number of eyedrops becomes cumbersome to the patient, or if patient compliance with medical therapy is difficult, or if medical therapy is not effective in lowering the IOP. One non-cyclodestructive surgical technique is filtration surgery, a procedure in which an outlet for the aqueous fluid is made through the sclera, the white fibrous covering of the anterior part of the eye. Another such procedure is argon laser trabeculoplasty, in which laser burns are made on the trabecular meshwork, the major drainage system to increase the number of drainage ports from the eye. Both these procedures promote outward flow of the intraocular fluid, decreasing the IOP.
In congenital glaucoma, other procedures that open up the fluid flow within the eye such as goniotomy or trabeculotomy are performed. Many patients with congenital glaucoma, due to a defect in the interior structure of the eye, have a limited ability to drain the aqueous fluid sufficiently. For pediatric patients, trabeculoplasty is not successful because the maturing eye will attempt to close the outlet. CCT may be performed on patients for which cyclophotocoagulation, another method of cyclodestruction, is not an option or not available. Many patients on whom this technique is employed have neovascular glaucoma, a type of glaucoma that is a result of uncontrolled diabetes or hypertension.
Purpose
The main purpose of CCT is to treat uncontrolled or refractory glaucoma. It is also used to reduce pain in some patients with end-stage glaucoma. This procedure lowers the intraocular pressure by destroying the source of intraocular fluid, the ciliary body, and subsequently lowering the intraocular pressure, as well as decreasing the pain of patients with some glaucomas, the most notable of which is neovascular glaucoma.
Demographics
Patients who undergo CCT are patients for whom certain techniques such as filtration surgery are contraindicated or for which other medical and surgical procedures have not been successful. Patients with neovascular glaucoma and congenital glaucoma make up a large percentage of the patients who undergo CCT. Because of the risks involved, cyclocryotherapy should not be performed on patients who have the potential for good vision, or on individuals who have had cataract surgery with intraocular lens implantation. CCT is a last-resort technique employed on patients for whom all other strategies have failed.
Description
Cyclocryotherapy is usually performed while the patient is awake and supine (laying down on the back). Prior to doing CCT, the doctor will inject an anesthetic into the posterior part of the eye; however, CCT may be performed under general anesthesia for anxious adults and for children. In performing the procedure, the surgeon locates the ciliary body with a lighted instrument and then applies a cryoprobe with a temperature of -112°F (-80°C) to the sclera of the eye. This probe is applied to the eye several times in a clockwise manner, using moderate pressure, carefully avoiding the area of the eye where the extraocular muscles, which control movement of the eye, attach to the eye. Each application by the probe lasts 50–60 seconds and usually only half of the eye is treated during the initial attempt; for less severe glaucoma and in older patients who respond better to this treatment, only a quarter of the eye will be treated. The surgeon leaves at least one quadrant of the eye untreated.
Immediately after surgery, a steroid is injected into the eye to reduce inflammation, and an eyedrop or ointment such as atropine is applied to the eye to maintain dilation of the eye. Some surgeons may inject into the eye an anesthetic that numbs the entire eye, including the muscles. This injection has many risks associated with it, such as a droopy eyelid and an increased risk of corneal ulcers.
Diagnosis/Preparation
Cyclocryotherapy is a procedure of last resort in glaucoma patients. When all other therapies available to the patient have failed, CCT is considered, especially if the patient's vision is poor, i.e., less than 20/200, since there is a high risk of vision loss associated with this procedure. Patients and/or legal guardians of the patient are informed of the inherent risks and benefits, and CCT is performed only after informed consent . In preparation for CCT, the patient continues with all glaucoma medications up to the day of the procedure.
Aftercare
It is important that the patient continue with most topical glaucoma medications after surgery because a significant spike in IOP is expected after cyclocryotherapy. Glaucoma medications that should not be continued include miotics, which constrict the pupil and thus act in opposition to atropine, and drops derived from prostaglandins, which have very limited effect in some forms of glaucoma, especially neovascular glaucoma. Steroids are administered to the eye to reduce the risk of inflammation. Atropine, which dilates or enlarges the pupil and decreases post-operative discomfort, may be used a few times a day. Atropine and steroids are continued for a month after surgery.
As the retrobulbar anesthesia wears off, usually within 12 hours, acetaminophen (Tylenol) may be required for pain. In patients for whom the potential for good vision is unlikely and in whom the CCT is done to eliminate pain, the doctor may inject alcohol into the eye for continued pain relief.
Patients are seen for follow-up visits at a minimum of one day, one week, and one month after surgery. Sometimes the procedure needs to be repeated and, if this is the case, it should be done no sooner than one month after the first attempt. The area that was treated initially is treated again and may be expanded to include a third quadrant.
Risks
The risks of this procedure are greater than for other types of glaucoma treatment. The most common side effect is pain after the procedure. A common risk of CCT is hypotony, which is a low level of fluid in the eye that can lead to phthisis bulbi, a condition in which the fluid level in the eye reaches a dangerously low level, such that the integrity of the eye is compromised. Other risks to consider are retinal detachment, inflammation of the iris, cataract formation, macular edema, and swelling of the cornea. The risk of inflammation within the eye is greater for diabetics. Loss of visual acuity, including total vision loss, is an associated risk of any of the previously mentioned risks and occurs in up to 67% of patients.
Patients with darker irises will have more side effects from this procedure, and pediatric patients with aniridia, or no iris, also have an increased rate of complications. Individuals who are aphakic, meaning they have had cataract extraction without a subsequent intraocular lens implantation, have fewer complications than patients with an intact lens.
Normal results
Normal results of cyclocryotherapy would be a reduction in the IOP and decreased intraocular pain. The overall success rate of CCT to reduce IOP in glaucoma patients is reported to be from 34% to 92%. Approximately 70% of patients with neovascular glaucoma have an IOP reduction of at least 50%. A determination of whether or not the surgery has been effective may not be clear until a month after CCT is performed; retreatment is required in up to one-third of adult patients. Repeated procedures increase the success of the surgery. CCT is successful in 90% of patients after a second surgery and in 95% after the third treatment. Among pediatric patients who undergo CCT, the success rate is only 30–44%, as the ciliary body of the child is more resistant to damage by cryotherapy, and thus repeat applications are more common.
Morbidity and mortality rates
Within four years of treatment, hypotony will occur in up to 12% of all patients who undergo CCT, but is seen in up to 40% of patients with neovascular glaucoma. Up to two-thirds of patients will lose some visual acuity after CCT; many of them will have vision worse than 20/400. About 20% of patients who have had cyclocryotherapy will develop cataracts.
Alternatives
An alternative to cyclocryotherapy is cyclophotocoagulation. This is another cyclodestructive procedure that employs the thermal energy of a laser instead of the freezing temperature of cryotherapy to ablate, or destroy, a part of the ciliary body. Cyclophotocoagulation is performed with the patient seated at the slit lamp biomicroscope. The eye is anesthesized prior to performing the procedure. In one type of cyclophotocoagulation, a fiberoptic laser endoscope is passed into the eye to help the surgeon visualize the interior of the eye. The energy of a laser passes through the endoscope and destroys the ciliary body directly. In another type of cyclodestruction, the energy of a diode laser is applied to the ciliary body through the sclera without the use of an endoscope.
Cyclophotocoagulation is as effective as CCT without as many of the complications inherent in CCT. The risks of transient elevation of intraocular inflammation and intraocular inflammation itself are decreased with this procedure over CCT for adult patients, but the risks associated with this procedure for pediatric patients are comparable to CCT. The cyclophotocoagulation procedure is not as painful as CCT.
Surgical removal of the part of the ciliary body is another alternative that is not often used. It is effective in lowering IOP, but the rate of complications such as hemorrhages in the vitreous, hypotony, and retinal detachment is high.
Therapeutic ultrasound can also be used to reduce the IOP in glaucoma patients, though the mechanism in which the IOP is lowered in this procedure is not clear.
In end-stage neovascular glaucoma patients who have no useful vision, medical treatment of pain control may sometimes be attained with the use of atropine and topical steroids alone. Retrobulbar injection of alcohol is sometimes necessary and, as a last resort in painful eyes without useful vision, enucleation, or removal, of the eye is required.
Resources
books
Albert, Daniel M. Principles and Practice of Ophthalmology, 2nd Ed. Philadelphia, PA: W.B. Saunders Company, 2000.
Azuara-Blanco, Augusto. Handbook of Glaucoma. London: Martin Dunitz Ltd., 2002.
Epstein, Daniel, et al. Glaucoma. Baltimore, MD: Williams and Wilkins, 1997.
Jaffe, Norman S. Atlas of Ophthalmic Surgery, London: Mosby-Wolfe, 1996.
Kanski, Jack. Glaucoma: A Colour Manual of Diagnosis and Treatment, 2nd Ed. Oxford: Butterworth Heinemann, 1996.
Ritch, Robert, et.al The Glaucomas, Vol. 2 Clinical Sciences. St Louis, MO: Mosby Yearbook, 1996.
Ritch, Robert, et.al The Glaucomas, Vol.3 Glaucoma Therapies. St Louis, MO: Mosby Yearbook, 1996.
periodicals
Deepak, Gupta. "Surgical Update, Part III The Fallback Options When IOP Won't Drop." Review of Optometry (February 15, 2003): 79–86.
Sivak-Calcott, M. D., et al. "Evidence-based Recommendations for the Diagnosis and Treatment of Neovascular Glaucoma." Ophthalmology 108 (October 2001): 1767–1778.
Wagle, Nikhil. "Long-term Outcome of Cyclocryotherapy for Refractory Pediatric Glaucoma." Ophthalmology 105 (October 1998): 1921–7.
other
Cyclotherapy for Endstage Glaucoma. http://http.wills-glaucoma.org/cyclo.htm .
Pediatric Glaucoma. http://www.childrens.org/MSO/dept/lnav/view.asp?nav+554 .
Martha Reilly, OD
WHO PERFORMS THE PROCEDURE AND WHERE IS IT PERFORMED?
This procedure is performed by an ophthalmologist in an office setting. Many ophthalmologists who perform glaucoma surgery have had an additional year of subspecialty training specific to the treatment of glaucoma.
QUESTIONS TO ASK THE DOCTOR
- How many of these procedures have you performed?
- Do you have advanced training in glaucoma surgery?
- Is CCT the best surgical procedure to treat my glaucoma or that of my child?
- What will vision be like after surgery?
THANK YOU