Antianxiety drugs
Definition
Antianxiety drugs are medicines that calm and relax people with excessive anxiety, nervousness, or tension, or for short-term control of social phobia disorder or specific phobia disorder.
Purpose
Antianxiety agents, or anxiolytics, may be used to treat mild transient bouts of anxiety as well as more pronounced episodes of social phobia and specific phobia. Clinically significant anxiety is marked by several symptoms. The patient experiences marked or persistent fear of one or more social or performance situations in which he or she is exposed to unfamiliar people or possible scrutiny by others, and may react in a humiliating or embarrassing way. The exposure to the feared situation produces an anxiety attack. Fear of these episodes of anxiety leads to avoidance behavior, which impairs normal social functioning, including working or attending classes. The patient is aware that these fears are unjustified.
Antianxiety drugs, particularly the injectable benzodiazepines lorazepam (Ativan) and midazolam (Versed), are also used for preoperative sedation in surgery. Used for this purpose, they may induce relaxation, provide sedation, and also reduce memory of an unpleasant experience. They offer the combined benefits of relaxing the patient, and reducing the need for other agents including analgesics , anesthetics, and muscle relaxants .
Description
In psychiatric practice, treatment of anxiety has largely turned from traditional antianxiety agents, anxiolytics, to antidepressant therapies. In current use, the benzodiazepines, the best-known class of anxiolytics, have been largely supplanted by serotonin-specific reuptake inhibitors (SSRIs, including citalopram, fluoxetine, fluvoxamine, and others), which have a milder side effect profile and less risk of dependency. However, traditional anxiolytics remain useful for patients who need a rapid onset of action, or whose frequency of exposure to anxiety-provoking stimuli is low enough to eliminate the need for continued treatment. While SSRIs may require three to five weeks to show any effects, and must be taken continuously, benzodiazepines may produce a response within 30 minutes, and may be dosed on an as-needed basis.
The intermediate-action benzodiazepines, alprazolam (Xanax), and lorazepam (Ativan), are the appropriate choice for treatment of mild anxiety and social phobia. Diazepam (Valium) is still widely used for anxiety,
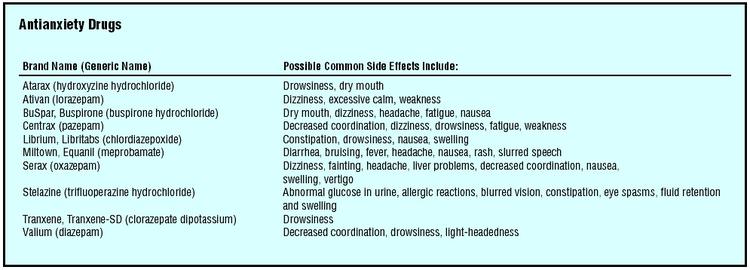
| Brand Name (Generic Name) | Possible Common Side Effects Include: |
| Atarax (hydroxyzine hydrochloride) | Drowsiness, dry mouth |
| Ativan (lorazepam) | Dizziness, excessive calm, weakness |
| BuSpar, Buspirone (buspirone hydrochloride) | Dry mouth, dizziness, headache, fatigue, nausea |
| Centrax (pazepam) | Decreased coordination, dizziness, drowsiness, fatigue, weakness |
| Librium, Libritabs (chlordiazepoxide) | Constipation, drowsiness, nausea, swelling |
| Miltown, Equanil (meprobamate) | Diarrhea, bruising, fever, headache, nausea, rash, slurred speech |
| Serax (oxazepam) | Dizziness, fainting, headache, liver problems, decreased coordination, nausea, swelling, vertigo |
| Stelazine (trifluoperazine hydrochloride) | Abnormal glucose in urine, allergic reactions, blurred vision, constipation, eye spasms, fluid retention and swelling |
| Tranxene, Tranxene-SD (clorazepate dipotassium) | Drowsiness |
| Valium (diazepam) | Decreased coordination, drowsiness, light-headedness |
but its active metabolite, desmethyldiazepam, which has a long half-life, may make this a poorer choice than other drugs in its class. There is considerable variation between individuals in the metabolism of benzodiazepines, so patient response may not be predictable. As a class, benzodiazepines are used not only as anxiolytics, but also as sedatives, muscle relaxants, and in treatment of epilepsy and alcoholism. The distinctions between these uses are largely determined by onset and duration of action, and route of administration.
Buspirone (BuSpar), which is not chemically related to other classes of central nervous system drugs, is also a traditional anxiolytic, although it is now considered either a third-line or adjunctive agent for use after trials of SSRIs and benzodiazepines. It is appropriate for use in patients who have either failed trials of other treatments, or who should not receive benzodiazepines because of a history of substance abuse problems. Buspirone, in common with antidepressants, requires a two- to three-week period before there is clinical evidence of improvement, and must be continuously dosed to maintain its effects.
In surgery, antianxiety drugs may be used to provide relaxation and reduce fear of surgery. They may reduce the need for anesthetics and muscle relaxants. In addition, some antianxiety drugs may impair memory, which is a benefit since it reduces concern about an unpleasant experience. Short-acting benzodiazepines such as midazolam (Versed) and lorazepam (Ativan) are most often used for this purpose.
Benzodiazepines are controlled drugs under federal law. Buspirone is not a controlled substance and has no established abuse potential.
Recommended dosage
Pre-surgical dosing of midazolam varies with the route of administration, the age and physical condition of the patient, and the other drugs to be used. For patients under the age of 60, who have not received narcotic analgesics, a dose of 2–3 mg is normally adequate, but some elderly patients may respond to a dose as low as 1 mg. The usual dose of lorazepam is up to 4 mg, administered by intramuscular injection at least two hours prior to surgery. If the drug is given intravenously, a dose of up to 2 mg may be given 15–20 minutes before surgery.
Benzodiazepines should be administered 30–60 minutes before exposure to the anticipated stress. Dosage should be individualized to minimize sedation. The normal dose of alprazolam is 0.25–0.5 mg. The usual dose of lorazepam is 2–3 mg. Doses may be repeated if necessary.
Buspirone is initially dosed at 5 mg three times a day. The dosage should be increased 5 mg/day, at intervals of two to three days, as needed. A dosage of 60 mg/day should not be exceeded. Two to three weeks may be required before a satisfactory response is observed.
Precautions
Precautions and warnings apply to the use of antianxiety agents for use over long periods of time. They are unlikely to occur in patients who have only received a single dose prior to surgery.
Benzodiazepines should not be used in patients with psychosis, acute narrow-angle glaucoma, or liver disease. The drugs can act as respiratory depressants and should be avoided in patients with respiratory conditions. Benzodiazepines are potentially addictive and should not be administered to patients with substance abuse disorders. Because benzodiazepines are sedatives, they should be avoided in patients who must remain alert. Their use for periods over four months has not been documented. These drugs should not be used during the second and third trimester of pregnancy, although use during the first trimester appears to be safe. They should not be taken while breastfeeding. Specialized references for use in children should be consulted.
Buspirone is metabolized by the liver and excreted by the kidney, and should be used with care in patients with hepatic or renal disease. The drug is classified as schedule B during pregnancy, but should not be taken during breastfeeding. Its use in children under the age of 18 years has not been studied.
Interactions
The metabolism of alprazolam may be increased by cimetidine, oral contraceptives, disulfiram, fluoxetine, isoniazid, ketoconazole, metoprolol, propoxyphene, propranolol, and valproic acid. The absorption of all benzodiazepines is inhibited by concomitant use of antacids. Benzodiazepines may increase blood levels of digoxin, and reduce the efficacy of levodopa. Other drug interactions have been reported.
Buspirone levels will be increased by concomitant use of erythromycin, itraconazole, and nefazadone. Doses should be adjusted based on clinical response. Use of buspirone at the same time as monoamine oxidase inhibitors (MAOIs, including phenelzine and tranycypromine) may cause severe blood pressure elevations. Use of buspirone with MAOIs should be avoided.
Side effects
The most common side effects of benzodiazepines are secondary to their central nervous system (CNS) effects and include sedation and sleepiness; depression; lethargy; apathy; fatigue; hypoactivity; lightheadedness; memory impairment; disorientation; anterograde amnesia; restlessness; confusion; crying or sobbing; delirium; headache; slurred speech; aphonia; dysarthria; stupor; seizures; coma; syncope; rigidity; tremor; dystonia; vertigo; dizziness; euphoria; nervousness; irritability; difficulty in concentration; agitation; inability to perform complex mental functions; akathisia; hemiparesis; hypotonia; unsteadiness; ataxia; incoordination; weakness; vivid dreams; psychomotor retardation; "glassy-eyed" appearance; extrapyramidal symptoms; and paradoxical reactions. Other reactions include changes in heart rate and blood pressure, changes in bowel function, severe skin rash, and changes in genitourinary function. Other adverse effects have been reported.
Buspirone has a low incidence of side effects. Dizziness and drowsiness are the most commonly reported adverse effects. Other CNS effects include dream disturbances; depersonalization, dysphoria, noise intolerance, euphoria, akathisia, fearfulness, loss of interest, disassociative reaction, hallucinations, suicidal ideation, seizures; feelings of claustrophobia, cold intolerance, stupor and slurred speech, and psychosis. Rarely, heart problems, including congestive heart failure and myocardial infarction, have been reported. Other adverse effects have been reported.
Resources
books
AHFS: Drug Information. Washington, DC: American Society of Healthsystems Pharmaceuticals, 2003.
Brody, T.M., J. Larner, K.P. Minneman, and H.C. Neu. Human Pharmacology: Molecular to Clinical, 2nd ed. St. Louis: Mosby Year-Book, 1998.
Karch, A.M. Lippincott's Nursing Drug Guide. Springhouse, PA: Lippincott Williams & Wilkins, 2003.
Racagni, G, C. Massotto, and L. Steardo. Pharmacology of Anxiolytic Drugs. Who Expert Series on Neuroscience. Vol. 3. Cambridge, MA: Hogrefe and Huber, 1997.
Reynolds, J.E.F., ed. Martindale: The Extra Pharmacopoeia, 31st ed. London: The Pharmaceutical Press, 1993.
other
"Anxiolytic Drugs." West Virginia University Health Sciences College. [cited May 2003]. http://www.hsc.wvu.edu/som/physio/P&P%20750/Woodfork/Anxiolytics%20PP%2002.pdf .
"Benzodiazepines (Systemic)." Medline Plus Drug Information. [cited May 2003]. http://www.nlm.nih.gov/medlineplus/druginfo/uspdi/202084.html .
Samuel Uretsky, PharmD
I have been having anxiety attacks for about 4 years and I have never been on medication for it because mine caused me to have nausia and reflux issues and the meds after effects cause that so there is no point really.
I also think it's an appropriate choice namely because from suffering you learn the best and greatest lessons in life. If you learn your triggers it is more effective then any medication. You also see a side of yourself you thought you would never see otherwise and you truly appriciciate your moments of sanity... there is my preaching for this afternoon.
The Logic od Rudie is incorrect. More teens get in car accidents that older adults, but banning cars is not the answer either.
As always, there will be responsible people and those less so, for whatever reasons. People desperate to get high will even breath glue fumes... There's no practical way to prevent these problems. Life is not that "perfect"...