Vasectomy
Definition
A vasectomy is a surgical procedure performed on adult males in which the vasa deferentia (tubes that carry sperm from the testicles to the seminal vesicles) are cut, tied, cauterized (burned or seared), or otherwise interrupted. The semen no longer contains sperm after the tubes are cut, so conception cannot occur. The testicles continue to produce sperm, but they die and are absorbed by the body.
Purpose
The purpose of the vasectomy is to provide reliable contraception. Research indicates that the level of effectiveness is 99.6%. Vasectomy is the most reliable method of contraception and has fewer complications and a faster recovery time than female sterilization methods.
The cost of a vasectomy ranges between $400 and $550 in most parts of the United States. Some insurance plans will cover the cost of the procedure.
Demographics
Approximately 500,000 vasectomies are performed annually in the United States. About one out of every six men over the age of 35 has had a vasectomy. Higher vasectomy rates are associated with higher levels of education and income.
Description
Vasectomies are often performed in the doctor's office or an outpatient clinic using local anesthesia. The area around the patient's scrotum (the sac containing the testicles that produce sperm) will be shaved and cleaned with an antiseptic solution to reduce the chance of infection. A small incision is made into the scrotum. Each of the vasa deferentia (one from each testicle) is tied in two places with nonabsorbable (permanent) sutures and the tube is severed between the ties. The ends may be cauterized (burned or seared) to decrease the chance that they will leak or grow back together.
"No scalpel" vasectomies are gaining in popularity. Instead of an incision, a small puncture is made into the
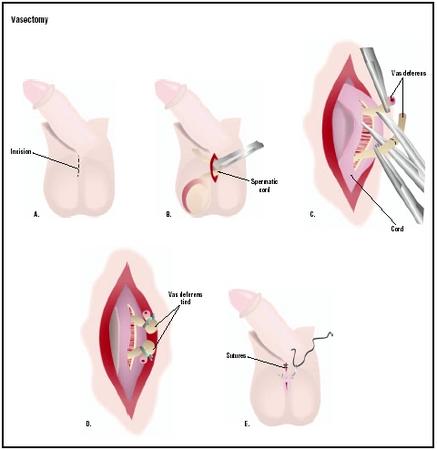
The patient is not sterile immediately after the procedure is finished. Men must use other methods of contraception until two consecutive semen analyses confirm that there are no sperm present in the ejaculate. It takes about four to six weeks or 15–20 ejaculations to clear all of the sperm from the tubes.
In some cases vasectomies may be reversed by a procedure known as a vasovasostomy . In this procedure, the surgeon reconnects the ends of the severed vasa deferentia. A vasectomy should be considered permanent, however, as there is no guarantee of successful reversal. Vasovasostomies are successful in approximately 40–50% of men.
Diagnosis/Preparation
No special physical preparation is required for a vasectomy. The physician will first assess the patient's general health in order to identify any potential problems that could occur. The doctor will then explain the possible risks and side effects of the procedure. The patient is asked to sign a consent form which indicates that he understands the information he has received, and gives the doctor permission to perform the operation.
Aftercare
Following the surgery, ice packs are often applied to scrotum to decrease pain and swelling. A dressing (or athletic supporter) which supports the scrotum can also reduce pain. Mild over-the-counter pain medication such as aspirin or acetaminophen (Tylenol) should be able to control any discomfort. Activities may be restricted for one to two days, and sexual intercourse for three to four days.
Risks
There are very few risks associated with vasectomy other than infection, bruising, epididymitis (inflammation of the tube that carries the sperm from the testicle to the penis), and sperm granulomas (collections of fluid that leaks from a poorly sealed or tied vas deferens). These complications are easily treated if they do occur. Patients do not experience difficulty achieving an erection, maintaining an erection, or ejaculating. There is no decrease in the production of the male hormone (testosterone), and the patient's sex drive and ability are not altered. Vasectomy is safer and less expensive than tubal ligation (sterilization of a female by cutting the Fallopian tubes to prevent conception).
According to both the World Health Organization (WHO) and the National Institutes of Health (NIH), there is no evidence that a vasectomy will increase a man's long-term risk of testicular cancer, prostate cancer, or heart disease.
Normal results
Vasectomies are 99% successful in preventing conception. As such, male sterilization is one of the most effective methods of contraception available to consumers.
Morbidity and mortality rates
Complications occur in approximately 5% of vasectomies. The rates of incidence of some of the more common complications are:
- mild bleeding into the scrotum: one in 400
- major bleeding into the scrotum: one in 1000
- infection: one in 100
- epididymitis: one in 100
- sperm granuloma: one in 500
- persistent pain: one in 1,000
Fournier gangrene is a very rare but possible complication of vasectomy in which the lining of tissue underneath the skin of the scrotum becomes infected (a condition called fasciitis). Fournier gangrene progresses very rapidly and is treated with aggressive antibiotic therapy and surgery to remove necrotic (dead) tissue. Despite treatment, a mortality rate of 45% has been reported for this condition.
Alternatives
There are numerous options available to couples who are interested in preventing pregnancy. The most common methods are female sterilization, oral contraceptives, and the male condom. Female sterilization has a success rate of 99.5%; oral contraceptives, 95–99.5%; and the male condom, 86–97%.
Resources
books
"Family Planning: Sterilization." Section 18, Chapter 246 in The Merck Manual of Diagnosis and Therapy , edited by Mark H. Beers, MD, and Robert Berkow, MD. Whitehouse Station, NJ: Merck Research Laboratories, 1999.
periodicals
Hartanto, Victor, Eric Chenven, David DiPiazza, et al. "Fournier Gangrene Following Vasectomy." Infections in Urology 14, no.3 (2001): 80-82.
organizations
Alan Guttmacher Institute. 1120 Connecticut Ave., NW, Suite 460, Washington, DC 20036. (202) 296-4012. http://www.agiusa.org .
Planned Parenthood Federation of America. 810 Seventh Ave., New York, NY 10019. (212) 541-7800. http://www.plannedparenthood.org .
other
The Alan Guttmacher Institute. "Contraceptive Use." 1999 [cited February 28, 2003]. http://www.agi-usa.org/pubs/fb_contr_use.html .
"Facts About Birth Control." Planned Parenthood Federation of America. January 2001 [cited February 28, 2003]. http://www.plannedparenthood.org/bc/bcfacts1.html .
"Facts About Vasectomy Safety." National Institute of Child Health and Human Development. September 3, 2002 [cited February 28, 2003]. http://www.nichd.nih.gov/publications/pubs/vasect.htm .
"Vasectomy: Questions and Answers." EngenderHealth. 2000 [cited February 28, 2003]. http://www.engenderhealth.org/wh/fp/cvas2.html .
VasectomyMedical.com . February 4, 2003 [cited February 28, 2003]. http://www.vasectomymedical.com .
Donald G. Barstow, RN Stephanie Dionne Sherk
WHO PERFORMS THE PROCEDURE AND WHERE IS IT PERFORMED?
Vasectomy is a minor procedure that can be performed in a clinic or doctor's office on an outpatient basis. The procedure is generally performed by a urologist, who is a medical doctor who has completed specialized training in the diagnosis and treatment of diseases of the urinary tract and genital organs.
QUESTIONS TO ASK THE DOCTOR
- How often do you perform vasectomies?
- What is your rate of complications?
- How long will the procedure take?
- What will the procedure cost? Will my insurance cover the cost?
- Do you perform vasectomy reversal? What is your success rate?
visit worldpharmarx . com
SO PLEASE ADVICE ME
I have no children in past 4 years
and my problem was sperm route tube is nil
any chance to tube fittment in artificial?
because I am try two times for ICSI treatment and no result in each time
for best mortgage service in Vancouver lendingexperts.ca
pains or a fever.
What should I do also im really concerned about Fournier gangrene, can it develop over a year later ?