Pelvic ultrasound
Definition
Pelvic ultrasound is a procedure in which high-frequency sound waves create images of the pelvic organs. The sound waves are projected into the pelvis, and measure how they reflect—or echo—back from the different tissues.
Purpose
Ultrasound is a preferred method of examining the pelvis, and functions as an extension of a physical examination , particularly for obese patients. It is a common initial step after physical examination when a patient complains of pelvic pain or abnormal vaginal bleeding. The procedure is performed routinely during pregnancy and examinations to determine the cause of infertility. Ultrasound has the ability to detect the size and shape of pelvic organs, such as the bladder, and is useful in evaluating the cause of bladder dysfunction. In women, pelvic ultrasound is used to examine the uterus, ovaries, cervix, and vagina. In general, ultrasound can detect inflammation, free fluid, cysts (abnormal fluid-filled spaces), and tumors in the pelvic region.
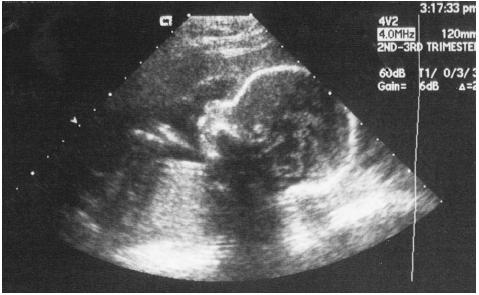
A primary use of pelvic ultrasound is during pregnancy. In early pregnancy (about five to seven weeks), ultrasound may determine the size of the fetus to confirm the suspected due date, detect multiple fetuses, or confirm that the fetus is alive (viable). Ultrasound is particularly useful in distinguishing between intrauterine (within the uterus) and ectopic (outside the uterus) pregnancies. Toward the middle of the pregnancy (about 16–20 weeks), the procedure can confirm fetal growth, reveal defects in the anatomy of the fetus, and check the placenta and amniotic fluid. Toward the end of pregnancy, it may be used to evaluate fetal size, position, growth, or to check the placenta.
Doctors may use ultrasound to guide the biopsy needle during amniocentesis and chorionic villus sampling. The imaging allows precise placement of the long needle that is inserted into the patient's uterus to collect cells from the placenta or amniotic fluid.
Description
Depending on the goal of the procedure, a pelvic ultrasound can also be called a bladder ultrasound, pelvic gynecologic sonogram, or obstetric sonogram. Ultrasound examinations are usually done in a doctor's office, clinic, or hospital setting. Typically, the patient will lie on an examination table with the pelvis exposed. Special gel is applied to the area to make sure that there is no air between the hand-held transducer and the skin, and to facilitate transducer movement. The physician or technologist guides the transducer over the abdomen. The transducer both creates and receives the echoes of the high-frequency sound waves (usually in the range of 3.5–10.0 megahertz). An ultrasound scan reveals the shape and densities of organs and tissues. By performing repeated scans over time, much like the frames of a movie, ultrasound can also reveal movement, such as the motions of a fetus. This technique is called real-time ultrasound.
Using a computerized tool, called a caliper, the ultrasound technologist can measure various structures shown in the image. For example, the length of the upper thigh bone (femur) or the distance between the two sides of the skull can indicate the age of the fetus.
Ultrasound technology has been safely used in medical settings for over 30 years, and several significant extensions to the procedure have made it even more useful. A specially designed transducer probe can be placed in the vagina to provide better ultrasound images. This transvaginal or endovaginal scan is particularly useful in early pregnancy or in cases where ectopic pregnancy is suspected. It is also routinely used to provide better anatomic delineation of the endometrium and pelvic masses. In men, transrectal scans, where the probe is placed in the rectum, are done to check the prostate. Doppler ultrasound has the ability to follow the flow of blood through veins and arteries, and can be useful in detecting disorders such as abnormal blood flow associated with ovarian torsion (a twisted blood supply that causes pelvic pain). Color enhancement is particularly useful in Doppler imaging, where shades of red signify flow away from the transducer and shades of blue signify flow toward it.
Hysterosonography is another variant ultrasound procedure. It involves the injection of saline solution into the uterus during an endovaginal scan. The saline distends the uterine cavity (or endometrium) and simplifies the identification of polyps, fibroids, and tumors. The saline outlines the lesion, making it easier to find and evaluate. Hysterosonography can also be used in the testing of patency (openness) of the fallopian tubes during infertility evaluations.
Preparation
Before undergoing a pelvic ultrasound, the patient may be asked to drink several glasses of water and to avoid urinating for about one hour prior to exam time. When the bladder is full, it forms a convenient path, called an acoustic window, for the ultrasonic waves. A full bladder is not necessary for an endovaginal examination, sometimes making it a preferred choice in emergency situations. Women usually empty their bladders completely before an endovaginal exam.
Aftercare
For a diagnostic ultrasound, the lubricating gel applied to the abdomen is wiped off at the end of the procedure and the patient can immediately resume normal activities.
Risks
Ultrasound carries with it almost no risk for complications.
Normal results
A normal scan reveals no abnormalities in the size, shape, or density of the organs scanned. During pregnancy, a normal scan reveals a viable fetus of expected size and developmental stage. Although ultrasound is an extremely useful tool, it cannot detect all problems in the pelvic region. If a tumor or other lesion is very small or if it is masked by another structure, it may not be detected. When used during pregnancy, patients should be advised that ultrasound does not reveal all fetal abnormalities. Additionally, the reliability of ultrasound readings can depend on the skill of the technologist or physician performing the scan.
An abnormal scan may show the presence of inflammation, cysts, tumors, or abnormal blood flow patterns. These results may suggest further diagnostic procedures, or surgical or pharmacological treatment. Obstetrical ultrasound examinations may alter the anticipated due date or detect abnormalities or defects in the fetus. This information may reveal that the fetus cannot survive on its own after birth, or that it will require extensive treatment or care. The technologist performing the ultrasound should consult with a radiologist or other physician if any questionable results appear.
Resources
books
Sanders, Roger C. Clinical Sonography: A Practical Guide. Boston: Little, Brown and Company, 1998.
periodicals
Galen, Barbara A. "Diagnostic Imaging: An Overview." Primary Care Practice 3 (September/October 1999).
Jorizzo, J. "Sonohysterography: The Next Step in the Evaluation of the Abnormal Endometrium." Radiographics 117 (Oct. 1999).
Kaakagi, Y. "Sonography of Obstetric and Gynecologic Emergencies: Part II, Gynecologic Emergencies." American Journal of Roetgenology 661 (Mar. 2000).
Wooldridge, Leslie. "Ultrasound Technology and Bladder Dysfunction." American Journal of Nursing Supplement 100 (June 2000).
organizations
American Institute of Ultrasound in Medicine. 14750 Sweiter Lane, Suite 100, Laurel, MD 20707-5906. (301) 498-4100 or (800) 638-5352. http://www.aium.org .
American Registry of Diagnostic Medical Sonographers (ARDMS). 600 Jefferson Plaza, Suite 360, Rockville, MD 20852-1150. (301) 738-8401 or (800) 541-9754. http://www.ardms.org .
other
Valley, Verna T. "Ultrasonography, Pelvic." Emedicine. January 17, 2001. [cited May 6, 2001] http://www.emedicine.com/emerg/topic622.htm .
Michelle L. Johnson, M.S., J.D. Lee A. Shratter, M.D.
Amy Benton, Nationally Registered Certified Medical Assistant
I feel back pain, after 1 or 2 days later, bleeding starts like the sme of menses, Not too much. But sooner, i feel like I am getting baby birthing (Painful).
I haven't had any medicin except abtibiotics,like - Amoxicillin, and Treorex Bills.
I am worried about my health and life, so dear dr. what should i do?
Thanks
yasmiin,
It is very easy to read and understand and very informative. Now,I can go in with a clear picture and understanding of my procedure. THANK YOU!.
Mild ache similar to cramps.
I am way past menapause.
New hire I think because she took such a long time to do the ultrasound.
Worried.