Cleft lip repair
Definition
Cleft lip repair (cheiloplasty) is surgical procedure to correct a groove-like defect in the lip.
Purpose
A cleft lip does not join together (fuse) properly during embryonic development. Surgical repair corrects the defect, preventing future problems with breathing, speaking, and eating, and improving the person's physical appearance.
Demographics
Cleft lip is the second most common embryonic (congenital) deformity. (Club foot is the most common congenital deformity.) Cleft lip occurs in approximately one in 750–1,000 live births. The highest incidence exists in North American Indians and Japanese (approximately one in 350 births). African Americans and Africans represent the lowest incidence of cleft lip deformity (approximately one in 1,500 births). There is a higher frequency of clefting in certain populations of Scandinavia and Middle European countries.
Cleft lip occurs more commonly in males, while cleft palate is more likely to occur in females. Cleft lip alone (without cleft palate) occurs in approximately 20% of cases across both genders. The majority of cases—80%—have both cleft lip and cleft palate. A unilateral cleft lip, commonly occurring on the left side, is more common than a bilateral cleft lip.
Potential causes
Most cases of cleft lip have no known cause. However, there is a strong genetic correlation. Other single gene defects that are associated with cleft lip include: Van der Woude syndrome, Opitz Syndrome, Aarskog syndrome, Fryns syndrome, Waardenburg syndrome, and Coffin-Siris syndrome. Approximately 5% of cleft conditions are associated with a genetic syndrome. Most of these syndromes do not include mental retardation.
Facial cleft has been implicated with maternal exposure to environmental causes, such as rubella or medications that can harm the developing embryo. These medications include steroids, antiseizure drugs, vitamin A, and

Risk of cleft lip increases with paternal age, especially over 30 years at the time of conception. Generally, the risk is higher when both parents are over 30 years of age. However, most cases seem to be isolated within the family with no obvious causation.
When the affected child has unilateral cleft lip and palate, the risk for subsequent children increases to 4.2%. Advances in high resolution ultrasonography (prenatal ultrasound exam) have made it possible to detect facial abnormalities in the developing embryo (in utero).
Description
Developmental anatomy
Important structures of the embryo's mouth form at four to seven weeks of gestation. Development during this period entails migration and fusion of mesenchymal cells with facial structures. If this migration and fusion is interrupted (usually by a combination of genetic and environmental factors), a cleft can develop along the lip. The type of clefting varies with the embryonic stage when its development occurred.
There are several types of cleft lip, ranging from a small groove on the border of the upper lip to a larger deformity that extends into the floor of the nostril and part of the maxilla (upper jawbone).
Unilateral cleft lip results from failure of the maxillary prominence on the affected side to fuse with medial nasal prominences. The result is called a persistant labial groove. The cells of the lip become stretched and the tissues in the persistent groove break down, resulting in a lip that is divided into medial (middle) and lateral (side) portions. In some cases, a bridge of tissue (simart band) joins together the two incomplete lip portions.
Bilateral cleft lip occurs in a fashion similar to the unilateral cleft. Patients with bilateral cleft lip may have varying degrees of deformity on each side of the defect. An anatomical structure (intermaxillary segment) projects to the front and hangs unattached. Defects associated with bilateral cleft lip are particularly problematic due to discontinuity of the muscle fibers of the orbicularis oris (primary muscle of the lip.) This deformity can result in closure of the mouth and pursing of the lip.
Classification
In addition to classification as unilateral or bilateral, cleft lips are further classified as complete or incomplete. A complete cleft involves the entire lip, and typically the alveolar arch. An incomplete cleft involves only part of the lip. The Iowa system (which also classifies cleft palate) classifies cleft lip in five groups:
- Group I—clefts of the lip only
- Group II—clefts of palate only
- Group III—clefts of lip, alveolus, and palate
- Group IV—clefts of lip and alveolus
- Group V—miscellaneous
Another widely accepted cleft lip classification is based on recommendations of the American Cleft Palate Association. This classification divides cleft lip into unilateral or bilateral (right, left or extent) in thirds—(i.e., one-third, two-thirds, three-thirds), or median cleft lip, the extent of which is also measured in thirds.
Surgical procedure
Cleft lip repair can be initiated at any age, but optimal results occur when the first operation is performed between two and six months of age. Surgery is usually scheduled during the third month of life.
While the patient is under general anesthesia, the anatomical landmarks and incisions are carefully demarcated with methylene blue ink. An endotracheal tube prevents aspiration of blood. The surgical field is injected with a local anesthestic to provide further numbing and blood vessel constriction (to limit bleeding). Myringotomy (incisions in one or both eardrums) is performed, and myringotomy tubes are inserted to permit fluid drainage.
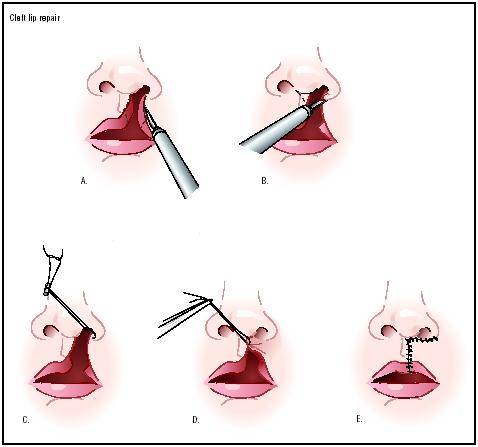
There are several operative techniques for cleft lip reconstruction. The Millard rotation advancement (R-A) technique is the most widely accepted form of repair. This method involves rotation of the entire philtral dimple (groove in the upper lip) and Cupid's bow (double curve of the upper lip). The scar falls along the new philtral column (central section of the upper lip), and is adjusted as required since the procedure allows for flexibility.
The Millard procedure begins with an incision on the edge of the cleft side of the philtrum, and the cutting continues upward, medially, and to the side. A second incision extends to the buccal sulcus (top part of the upper jaw). The length of this incision depends on the size of the gap to be closed. In this second incision, the surgeon frees soft tissue, which allows him or her to completely lift the lip from the underlying bone. This dissection should be tested to ensure free advancement toward the middle (inadequate dissection is the root cause of poor results). Nasal deformity can be dealt with by a procedure known as the McComb nasal tip plasty, which elevates the depressed nasal dome and rim. Cartilage from the cleft side is freed from the opposite side, and is positioned and reshaped using nylon sutures.
Advantages of the Millard rotation advancement technique (include:
- It is the most common procedure (i.e., surgeons more familiar with it).
- The technique is adaptable and flexible.
- It permits construction of a normal-looking Cupid's bow.
- A minimal amount of tissue is discarded.
- The suture line is camouflaged.
The disadvantage of the Millard rotation advancement technique is the possible development of a vermilion notch (shortening of the entire lip in the vertical direction), resulting from contracture of the vertical scar.
Cupid's bow is a critical part of the repair, making it very important to accurately determine the high point of Cupid's bow on the lateral lip.
Diagnosis/Preparation
Facial clefting has a wide range of clinical presentations, ranging from a simple microform cleft to the complete bilateral cleft involving the lip, palate, and nose. A comprehensive physical examination is performed immediately after birth, and the defect is usually evident by visual inspection and examination of the facial structures.
Care must be taken to diagnose other physical problems associated with a genetic syndrome. Weight, nutrition, growth, and development should be assessed and closely monitored.
Presurgical tests include a variety of procedures, such as hemoglobin studies. It is important for the pateint's parents and physician to discuss the operation prior to surgery.
Aftercare
The postoperative focus is on ensuring proper nutrition, as well as lip care and monitoring the activity level. Breast milk or full-strength formula is encouraged immediately after surgery or shortly thereafter. Lip care for patients with sutures should include gentle cleansing of suture lines with cotton swabs and diluted hydrogen peroxide. Liberal application of topical antibiotic ointment several times a day for 10 days is recommended. There will be some scar contracture, redness, and firmness of the area for four to six weeks after surgery. Parents should gently massage the area, and avoid sunlight until the scar heals.
The patient's activities may be limited. Some surgeons use elbow immobilizers to minimize the risk of accidental injury to the lip. Immobilizers should be removed several times a day in a supervised setting, allowing the child to move the restricted limb(s).
Interaction between the orthodontist and surgeon as part of the treatment team begins in the neonatal period, and continues through the phases of mixed dentition.
Risks
There may be excessive scarring and contraction of the lips. Two types of scars, hypertrophic or keloid, may develop. Hypertrophic scars appear as raised and red areas that usually flatten, fade in color, and soften within a few months. Keloids form as a result of the accelerated growth of tissue in response to the surgery or trauma to the area. The keloid can cause itching and a burning sensation. Scratching must be avoided because it can lead to healing problems. Some patients require minimal revision surgery, but in most cases, the initial redness and contracture is part of the normal healing process.
Normal results
Ideal surgical results for cleft lip include symmetrically shaped nostrils, and lips that appear as natural as possible and have a functional muscle. Many characteristics of the natural lip can be achieved; however, the outcome ultimately depends on a number of factors, including the skill of the surgeon, accurate presurgery markings, alignment of bones within the affected area, uncomplicated healing of the initial repair, and the effect of normal growth on the repaired lip. Additional surgical correction to reconstruct nasal symmetry is sometimes necessary.
Morbidity and mortality rates
Generally, cleft lip repair is well-tolerated in healthy infants. There are no major health problems associated with this reconstructive surgery. Depending on the results, it may be necessary to perform additional operations to achieve desired functional and cosmetic outcomes.
Alternatives
There are no alternatives for this surgery. Obvious deformity and impairments of speech, hearing, eating, and breathing occur as a direct result of the malformation. These issues can not be corrected without surgery.
Resources
books
Aston, S.J., R.W. Beasley, C.H.M. Thorne, Grabb and Smith's Plastic Surgery 5th ed. Philadelphia, PA: Lippincott-Raven Publishers, 1997.
Bluestone, Charles. Pediatric Otolaryngology. Philadelphia, PA: Saunders, 2003.
Cohen, M. Mastery of Plastic and Reconstructive Surgery. Little, Brown & Company, Boston, MA: 1994.
Georgiade, N. Pediatric Plastic Surgery. C. V. Mosby, Co., St Louis, MO: 1984.
Millard, Ralph, D. Principlization of Plastic Surgery. Boston, MA: Little, Brown & Company, 1986.
Papel, Ira. Facial Plastic and Reconstructive Surgery 2nd ed. Thieme Medical Pub., 2002.
periodicals
Byrd, H.S. "Selected Readings in Plastic Surgery: Cleft Lip I: Primary Deformities." Baylor University Medical Center 8 (1997): 221.
Salomon, J. and P.C. Hobar. "Selected Readings in Plastic Surgery: Cleft Lip II: Secondary Deformities." Baylor University Medical Center 2, no.22 (1997).
organizations
American Board of Plastic Surgery,Inc. Seven Penn Center, Suite 400, 1635 Market Street, Philadelphia, PA 19103-2204. (215) 587-9322. http://www.abplsurg.org .
International Birth Defects Information Systems. http://ibisbirthdefects.org/start/index.htm .
The International Craniofacial Institute. http://www.craniofacial.net/additional_services/additional_services.asp .
Laith Farid Gulli, M.D.,M.S. Robert Ramirez, B.S. Randall J. Blazic, M.D.,D.D.S. Bilal Nasser, ,M.D., M.S.
WHO PERFORMS THE PROCEDURE AND WHERE IS IT PERFORMED?
A plastic and reconstructive surgeon performs the procedure in a hospital equipped with a surgical department. Plastic surgeons typically have five years of training in general surgery (or orthopedic surgical training), and two additional years of specialized plastic and reconstructive surgery training. A plastic surgeon should be certified by the American Board of Plastic and Reconstructive Surgery.
Many plastic surgeons who operate on cleft lip (or palate) patients have received additional surgical training in pediatric plastic surgery. However, completion of a surgical training program does not guarantee clinical expertise, and parents should seek surgeons who having both training and experience.
QUESTIONS TO ASK THE DOCTOR
- How many cleft palate surgeries has the surgeon performed?
- How is nutrition managed after surgery?
- What lip care will be required after surgery?
- How much activity will be allowed, and will the patient be immobilized following the surgery?
- How much follow-up is required?
- What cosmetic and functional results are expected?
- How long is the surgical procedure?
- What follow-up reconstructive surgery is anticipated?
My medical bills have been a horror though, so please, if you can find anyone to make donations to the michael shwartz fund... I'd appreciate it. Thankyou. I am at the age of 43 and it is so difficult to take care of my infant son.
Also, we were horribly offended by the film, "Rubber Johnny".
This is an abomination.
I'm mother of a grat kid that was norn with cleft lip and palate. we know thar at 20 weeks pregnancy too. It was horrible ... we didn't knew the problem. Let me tell you that's no easy ... he have 6 months and made already the lip orrection. A lot of things will be done .. that's no easy, but all kids deserve have a life. our son will note hate you. He will apppreciate your lofer for him! Think about!
There is a note about Millard's operayion.
The main important thing in this operation is The Zigzag incision from the apex of the cleft to bare cleft edges. and also the principle of any operation is closing the defect 3 layers closure.and to lenghthen the lip by interposition of skin flaps from both.
Thanks for the topic.
I was born with a cleft lip, I had a few surgeries but my most recent was 6 weeks ago. The surgeon re-opened my lip and did some work on my nose. My lip is still very swollen, how long should I expect this to remain like this? Thanks.
well I wanted to know if you have another way to correct cleft lips people have q
not be the basis of medical surgeries, because I live in a community neither I nor my family is able to pay a plastic surgeon, I can not stand people looking at me strangely fikam nor q is people putting me nicknames, so we wanted to know if you have another way I can fix my lips.
thanks
I live in Rio De Janeiro
I hope you can help me
please advice me that my upper lip may get the shape as original once. if yes then what type of operation is required and what will be the approx. expences, and yes what will be the guarntee that my face will be look like others.
Thank you very much for all your advices, help, times and God bless all your babies!