Stress test
Definition
A stress test is primarily used to identify coronary artery disease. It requires patients to exercise on a treadmill or exercise bicycle while their heart rate, blood pressure, electrocardiogram (ECG), and symptoms are monitored.
Purpose
The body requires more oxygen during exercise than at rest. To deliver more oxygen during exercise, the heart has to pump more oxygen-rich blood. Because of the increased stress on the heart, exercise can reveal coronary problems that are not apparent when the body is at rest. This is why the stress test, though not perfect, remains the best initial noninvasive practical coronary test.
The stress test is particularly useful for detecting ischemia (inadequate supply of blood to the heart muscle) caused by blocked coronary arteries. Less commonly, it is used to determine safe levels of exercise in people with existing coronary artery disease.
Description
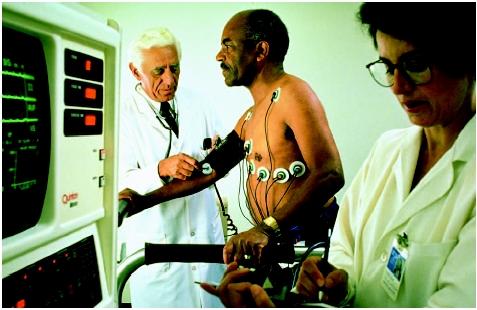
A technician affixes electrodes to the patient's chest, using adhesive patches with a special gel that conducts electrical impulses. Typically, electrodes are placed under each collarbone and each bottom rib, and six electrodes are placed across the chest in a rough outline of the heart. Wires from the electrodes are connected to an ECG, which records the electrical activity picked up by the electrodes.
The technician runs resting ECG tests while the patient is lying down, then standing up, and then breathing heavily for half a minute. These baseline tests can later be compared with the ECG tests performed while the patient is exercising. The patient's blood pressure is taken and the blood pressure cuff is left in place so that blood pressure can be measured periodically throughout the test.
The patient begins riding a stationary bicycle or walking on a treadmill. Gradually the intensity of the exercise is increased. For example, if the patient is walking on a treadmill, then the speed of the treadmill increases and the treadmill is tilted upward to simulate an incline. If the patient is on an exercise bicycle, then the resistance or "drag" is gradually increased. The patient continues exercising at increasing intensity until reaching the target heart rate (generally set at a minimum of 85% of the maximal predicted heart rate based on the patient's age) or experiences severe fatigue, dizziness, or chest pain. During the test, the patient's heart rate, ECG, and blood pressure are monitored.
Sometimes such other tests, as echocardiography or thallium scanning, are used in conjunction with the exercise stress test. For instance, recent studies suggest that women have a high rate of false negatives (results showing no problem when one exists) and false positives (results showing a problem when one does not exist) with the stress test. They may benefit from another test, such as exercise echocardiography. People who are unable to exercise may be injected with such drugs, as adenosine, which mimic the effects of exercise on the heart, and then given a thallium scan. The thallium scan or echocardiogram are particularly useful when the patient's resting ECG is abnormal. In such cases, interpretation of exercise-induced ECG abnormalities is difficult.
Preparation
Patients are usually instructed not to eat or smoke for several hours before the test. They should be advised to inform the physician about any medications they are taking, and to wear comfortable sneakers and exercise clothing.
Aftercare
After the test, the patient should rest until blood pressure and heart rate return to normal. If all goes well,
and there are no signs of distress, the patient may return to his or her normal daily activities.
Risks
There is a very slight risk of myocardial infarction (a heart attack) from the exercise, as well as cardiac arrhythmia (irregular heart beats), angina, or cardiac arrest (about one in 100,000). The exercise stress test carries a very slight risk (one in 100,000) of causing a heart attack. For this reason, exercise stress tests should be attended by health care professionals with immediate access to defibrillators and other emergency equipment.
Patients are cautioned to stop the test should they develop any of the following symptoms:
- unsteady gait
- confusion
- skin that is grayish or cold and clammy
- dizziness or fainting
- a drop in blood pressure
- angina (chest pain)
- cardiac arrhythmias (irregular heart beat)
Normal results
A normal result of an exercise stress test shows normal electrocardiogram tracings and heart rate, blood pressure within the normal range, and no angina, unusual dizziness, or shortness of breath.
A number of abnormalities may appear on an exercise stress test. Examples of exercise-induced ECG abnormalities are ST segment depression or heart rhythm disturbances. These ECG abnormalities may indicate deprivation of blood to the heart muscle (ischemia) caused by narrowed or blocked coronary arteries. Stress test abnormalities generally require further diagnostic evaluation and therapy.
Patient education
Patients must be well prepared for a stress test. They should not only know the purpose of the test, but also signs and symptoms that indicate the test should be stopped. Physicians, nurses, and ECG technicians can ensure patient safety by encouraging them to immediately communicate discomfort at any time during the stress test.
Resources
books
Ahya, Shubhada N., Kellie Flood, and Subramanian Paranjothi. The Washington Manual of Medical Therapeutics, 30th edition. Philadelphia: Lippincott Williams & Wilkins, 2001, pp. 96–100.
organizations
American Heart Association. 7272 Greenville Avenue, Dallas, TX 75231. (214) 373-6300. http://www.amhrt.org .
National Heart, Lung, and Blood Institute. Information Center. PO Box 30105, Bethesda, MD 20824-0105. (301) 951-3260. http://www.nhlbi.nih.gov .
Barbara Wexler Lee A. Shratter, M.D.
TREADMILL STRESS TEST. THE ONLY CONCERN I HAVE IS THAT THIS TEST WAS RECOMMENDED BY MY HEART DOCTOR AFTER I HAD TAKEN A CARDIAC CT ANGIOGRAPHY
WHICH INDICATED CALCIUM SCORES OF WHICH THE HIGHEST WAS 863. THIS WAS NOTICED IN THE LEFT INTERIOR DECENDING ARTERY WHICH WAS THE SAME ONE I HAD BI-PASSED 12 YEARS AGO. THE OTHER READINGS FOR THE OTHER ARTERIES WERE NOT OF IMMEADIATE CONCERN. ALSO I HAVE ATRIAL FIBRILLATION WHICH
WOULD BE CLASSIFIED AS ONE OF THE CONCERNS THAT YOU MENTION IN THIS ARTICLE. THANK YOU FOR THE ARTICLE & ANY OTHER INFORMATION THAT YOU MAY
FORWARD TO ME CONCERNING THIS.
My eyes were fluttering and they were calling my name.
I don't remember much for a few minutes.
I have a pre- existing disability.
Plus I had surgery on the base of my skull.
What does the tightness in my chest mean.
I don't know if I can handle yet another procedure.
I also have exercise induced asthma. Can you tell me why this happens?
five hours later. It is unusually fast according to my blood pressure machine.
Has anyone else experienced fast pulse rate and if so, how long does it last?