Peripheral vascular bypass surgery
Definition
A peripheral vascular bypass, also called a lower extremity bypass, is the surgical rerouting of blood flow around an obstructed artery that supplies blood to the legs and feet. This surgery is performed when the buildup of fatty deposits (plaque) in an artery has blocked the normal flow of blood that carries oxygen and nutrients to the lower extremities. Bypass surgery reroutes blood from above the obstructed portion of an artery to another vessel below the obstruction.
A bypass surgery is named for the artery that will be bypassed and the arteries that will receive the rerouted blood. The three common peripheral vascular bypass surgeries are:
- Aortobifemoral bypass surgery, which reroutes blood from the abdominal aorta to the two femoral arteries in the groin.
- Femoropopliteal bypass (fem-pop bypass) surgery, which reroutes blood from the femoral artery to the popliteal arteries above or below the knee.
- Femorotibial bypass surgery, which reroutes blood between the femoral artery and the tibial artery.
A substitute vessel or graft must be used in bypass surgeries to reroute the blood. The graft may be a healthy segment of the patient's own saphenous vein (autogenous graft), a vein that runs the entire length of the thigh. A synthetic graft may be used if the patient's saphenous vein is not healthy or long enough, or if the vessel to be bypassed is a larger artery that cannot be replaced by a smaller vein.
Purpose
Peripheral vascular bypass surgery is performed to restore blood flow (revascularization) in the veins and arteries of people who have peripheral arterial disease (PAD), a form of peripheral vascular disease (PVD). People with PAD develop widespread hardening and narrowing of the arteries (atherosclerosis) from the gradual build-up of plaque. In advanced PAD, plaque accumulations (atheromas) obstruct arteries in the lower abdomen, groin, and legs, blocking the flow of blood, oxygen, and nutrients to the lower extremities (legs and feet). Rerouting blood flow around the blockage is one way to restore circulation. It relieves symptoms in the legs and feet, and helps avoid serious consequences such as heart attack, stroke, limb amputation , or death.
Demographics
Approximately 8–10 million people in the United States have PAD caused by atherosclerosis. These people are at high risk of arterial occlusion, and are candidates for peripheral vascular bypass surgery. Occlusive arterial disease is found in 15–20% of men and women older
Description
The circulatory system delivers blood, oxygen, and vital nutrients to the limbs, organs, and tissues throughout the body. This is accomplished via arteries that deliver oxygen-rich blood from the heart to the tissues and veins that return oxygen-poor blood from organs and tissues back to the heart and lungs for re-oxygenation. In PAD, the gradual accumulation of plaque in the inner lining (endothelium) of the artery walls results in widespread atherosclerosis that can occlude the arteries and reduce or cut off the supply of blood, oxygen, and nutrients to organ systems or limbs.
Peripheral vascular bypass surgery is a treatment option when PAD affects the legs and feet. PAD is similar to coronary artery disease (CAD), which leads to heart attacks and carotid artery disease (CAD), which causes stroke. Atherosclerosis causes each of these diseases. Most often, atherosclerotic blockage or narrowing (stenosis) occurs in the femoral arteries that supply the thighs with blood or in the common iliac arteries, which are branches of the lower abdominal aorta that also supplies the legs. The popliteal arteries (a portion of the femoral arteries near the surface of the legs) or the posterior tibial and peroneal arteries below the knee (portions of the popliteal artery) can be affected.
Just as coronary artery disease can cause a heart attack when plaque blocks the arteries of the heart, or blockage in the carotid artery leading to the brain can cause a stroke, occlusion of the peripheral arteries can create life-threatening conditions. Plaque accumulation in the peripheral arteries blocks the flow of oxygen-carrying blood, causing cells and tissue in the legs and feet to die from lack of oxygen (ischemia) and nutrition. Normal growth and cell repair cannot take place, which can lead to gangrene in the limbs and subsequent amputation. If pieces of the plaque break off, they can travel from the legs to the heart or brain, causing heart attack, stroke, or death.
The development of atherosclerosis and PAD is influenced by heredity and also by lifestyle factors, such as dietary habits and levels of exercise . The risk factors for atherosclerosis include:
- high levels of blood cholesterol and triglycerides.
- high blood pressure (hypertension)
- cigarette smoking or exposure to tobacco smoke
- diabetes, types 1 and 2
- obesity
- inactivity, lack of exercise
- family history of early cardiovascular disease
Sometimes the body will attempt to change the flow of blood when a portion of an artery is narrowed by plaque. Smaller arteries around the blockage begin to take over some of the blood flow. This adaptation of the body (collateral circulation) is one reason for the absence of symptoms in some people who have PAD. Another reason is that plaque develops gradually as people age. Symptoms usually don't occur until a blockage is over 70%, or when a piece of plaque breaks off and blocks an artery completely. Blockage in the legs reduces or cuts off circulation, causing painful cramping during walking, which is relieved on rest (intermittent claudication). The feet may ache even when lying down at night.
When narrowing of an artery occurs gradually, symptoms are not as severe as they are when sudden, complete blockage occurs. Sudden blockage does not allow time for collateral vessels to develop, and symptoms can be severe. Gradual blockage creates muscle aches and pain, cramping, and sensations of fatigue or numbness in the limbs; sudden blockage may cause severe pain, coldness, and numbness. At times, no pulse can be felt, a leg may become blue (cyanotic) from lack of oxygen, or paralysis may occur.
When the lower aorta, femoral artery, and common iliac arteries (all in the lower abdominal and groin areas) are blocked, gradual narrowing may produce cramping pain and numbness in the buttocks and thighs, and men may become impotent. Sudden blockage will cause both legs to become painful, pale, cold, and numb, with no pulse. The feet may become painful, infected, or even gangrenous when gradual or complete blockage limits or cuts off circulation. Feet may become purple or red, a condition called rubor that indicates severe narrowing. Pain in the feet or legs during rest is viewed as an indication for bypass surgery because circulation is reduced to a degree that threatens survival of the limb.
Early treatment for PAD usually includes medical intervention to reduce the causes of atherosclerosis, such as lowering cholesterol and blood pressure, smoking cessation , and reducing the likelihood of clot formation. When these measures are not effective, or an artery becomes completely blocked, lower extremity bypass surgery may be performed to restore circulation, reduce foot and leg symptoms, and prevent limb amputation.
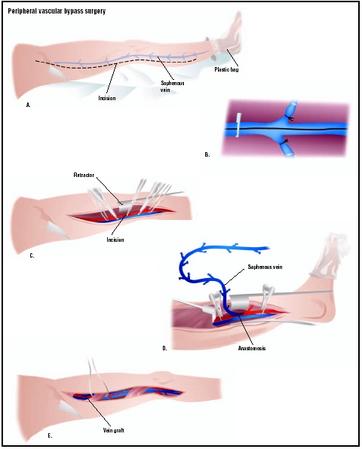
Bypass surgery is an open procedure that requires general anesthesia. In femoropopliteal bypass or femorotibial bypass, the surgeon makes an incision in the groin and thigh to expose the affected artery above the blockage, and another incision (behind the knee for the popliteal artery, for example) to expose the artery below the blockage. The arteries are blocked off with vascular clamps. If an autogenous graft is used, the surgeon passes a dissected (cut and removed) segment of the saphenous vein along the artery that is being bypassed. If the saphenous vein is not long enough or is not of good quality, a tubular graft of synthetic (prosthetic) material is used. The surgeon sutures the graft into an opening in the side of one artery and then into the side of the other. In a femoropopliteal bypass, for example, the graft extends from the femoral artery to the popliteal artery. The clamps are then removed and the flow of blood is observed to make sure it bypasses the blocked portion of the affected artery.
Aortobifemoral bypass surgery is conducted in much the same way, although it requires an abdominal incision to access the lower portion of the abdominal aorta and both femoral arteries in the groin. This is generally a longer and more difficult procedure. Synthetic grafts are used because the lower abdominal aorta is a large conduit, and its blood flow cannot be handled by the smaller saphenous vein. Vascular surgeons prefer the saphenous vein graft for femoropopliteal or femorotibial bypass surgery because it has proven to stay open and provide better performance for a longer period of time than synthetic grafts. Bypass surgery patients will be given heparin, a blood thinner, immediately after the surgery to prevent clotting in the new bypass graft.
Diagnosis/Preparation
Diagnosis
After obtaining a detailed history and reviewing symptoms, the physician examines the legs and feet, and orders appropriate tests or procedures to evaluate the vascular system. Diagnostic tests and procedures may include:
- Blood pressure and pulses—pressure measurements are taken in the arms and legs. Pulses are measured in the arms, armpits, wrists, groin, ankles, and behind the knees to determine where blockages may exist, since no pulse is usually felt below a blockage.
- Doppler ultrasonography—direct measurement of blood flow and rates of flow, sometimes performed in conjunction with stress testing (tests that incorporate an exercise component).
- Angiography—an x ray procedure that provides clear images of the affected arteries before surgery is performed.
- Blood tests—routine tests such as cholesterol and glucose, as well as tests to help identify other causes of narrowed arteries, such as inflammation, thoracic outlet syndrome, high homocycteine levels, or arteritis.
- Spiral computed tomography (CT angiography ) or magnetic resonance angiography (MRA)—less invasive forms of angiography.
Preparation
If not done earlier in the diagnostic process, ultrasonography or angiography procedures may be performed when the patient is admitted to the hospital. These tests help the physician evaluate the amount of plaque and exact location of the narrowing or obstruction. Any underlying medical condition, such as high blood pressure, heart disease, or diabetes is treated prior to bypass surgery to help obtain the best surgical result. Regular medications, such as blood pressure drugs or diuretics , may be discontinued in some patients. Routine pre-operative blood and urine tests are performed when the patient is admitted to the hospital.
Aftercare
After bypass surgery, the patient is moved to a recovery area where blood pressure, temperature, and heart rate are monitored for an hour or more. The surgical site is checked regularly. The patient is then transferred to a concentrated care unit to be observed for any signs of complications. The total hospital stay for femoropopliteal bypass or femorotibial bypass surgery may be two to four days. Recovery is slower with aortobifemoral bypass surgery, which involves abdominal incisions, and the hospital stay may extend up to a week. Walking will begin immediately for patients who have had femoropopliteal or femorotibial bypasses, but patients who have had aortobifemoral bypass may be kept in bed for 48 hours. When bypass patients go home, walking more each day, as tolerated, is encouraged to help maintain blood flow and muscle strength. Feet and legs can be elevated on a footstool or pillow when the patient rests. Some swelling of the leg should be expected; it does not indicate a problem and will resolve within a month or two.
During recuperation, the patient may be given pain medication if needed, and clot prevention (anticoagulant) medication. Any redness of the surgical site or other signs of infection will be treated with antibiotics . Patients are advised to reduce the risk factors for atherosclerosis in order to avoid repeat narrowing or blockage of the arteries. Repeat stenosis (restenosis) has been shown to occur frequently in people who do not make the necessary lifestyle modifications, such as changes in diet, exercise, and smoking cessation. The benefits of the bypass surgery may only be temporary if underlying disease, such as atherosclerosis, high blood pressure, or diabetes, is not also treated.
Risks
The risks associated with peripheral vascular bypass surgery are related to the progressive atherosclerosis that led to arterial occlusion, including a return of pre-operative symptoms. In patients with advanced PAD, heart attack or heart failure may occur. Build up of plaque has also taken place in the patient's arteries of the heart. Restenosis, the continuing build up of plaque, can occur within months to years after surgery if risk factors are not controlled. Other complications may include:
- clot formation in a saphenous vein graft
- failed grafts or blockages in grafts
- reactions to anesthesia
- breathing difficulties
- embolism (clot from the surgical site traveling to vessels in the heart, lungs, or brain)
- changes in blood pressure
- infection of the surgical wound
- nerve injury (including sexual function impairment after aortobifemoral bypass)
- post-operative bleeding
- failure to heal properly
Normal results
A femoropopliteal or femorotibial bypass with an autogenous graft of good quality saphenous vein has been shown to have a 60–70% chance of staying open and functioning well for five to 10 years. Aortobifemoral bypass grafts have been shown to stay open and reduce symptoms in 80% of patients for up to 10 years. Pain and walking difficulties should be relieved after bypass surgery. Success rates improve when the underlying causes of atherosclerosis are monitored and managed effectively.
Morbidity and mortality rates
The risk of death or heart attack is about 3–5% in all patients undergoing peripheral vascular bypass surgery. Following bypass surgery, amputation is still an outcome in about 40% of all surgeries performed, usually due to progressive atherosclerosis or complications caused by the patient's underlying disease condition.
Alternatives
Peripheral vascular bypass surgery is a mechanical way to reroute blood, and there is no alternative method. Alternative ways to prevent plaque build-up and reduce the risk of narrowing or blocking the peripheral arteries include nutritional supplements and alternative therapies, such as:
- Folic acid can help lower homocysteine levels and increase the oxygen-carrying capacity of red blood cells.
- Vitamins B 6 and B 12 can help lower homocysteine levels.
- Antioxidant vitamins C and E work together to promote healthy blood vessels and improve circulation.
- Angelica, an herb that contains coumadin, a recognized anticoagulant, which may help prevent clot formation in the blood.
- Essential fatty acids, as found in flax seed and other oils, to help reduce blood pressure and cholesterol, and maintain blood vessel elasticity.
- Chelation therapy, used to break up plaque and improve circulation.
Resources
books
Cranton, Elmer M.D., ed. Bypassing Bypass Surgery: Chelation Therapy: A Non-Surgical Treatment for Reversing Arteriosclerosis, Improving Blocked Circulation, and Slowing the Aging Process. Hampton Roads Pub. Co., 2001.
McDougal, Gene. Unclog Your Arteries: How I Beat Atherosclerosis. 1st Books Library, 2001.
organizations
American Heart Association (AHA). 7272 Greenville Ave., Dallas, TX 75231. (800) 242-8721. http://www.americanheart.org .
Vascular Disease Foundation. 3333 South Wadsworth Blvd. B104-37, Lakewood, CO 80227. (303) 949-8337 or (866)PADINFO (723-4636). http://www.vdf.org .
other
Bypass Surgery for Peripheral Arterial Disease. Patient Information, Vascular Disease Foundation, 2003. http://www.vdf.org.
Hirsch, M.D., Alan T. "Occlusive Peripheral Arterial Disease." The Merck Manual of Medicine—Home Edition, Heart and Blood Vessel Disorders 34:3. http://www.merck.com/pubs .
L. Lee Culvert
WHO PERFORMS THE PROCEDURE AND WHERE IS IT PERFORMED?
Peripheral vascular bypass surgery is performed by a vascular surgeon in a hospital operating room .
QUESTIONS TO ASK THE DOCTOR
- Why is this surgery necessary?
- How will the surgery improve my condition?
- What kind of anesthesia will be given?
- How many of these procedures has the surgeon performed?
- How many surgical patients had complications after the procedure?
- How can the patient expect to feel after surgery?
- How soon will the patient be able to walk?
- How long will it take to recover completely?
- What are the chances of this problem recurring after surgery?
- What can be done to help prevent this problem from developing again?
He relayed the message through her that he was seting up an appointment with a specialist!
Shouldn't my doctor go over the results of the test and explain them to me before sending me to another doctor?I am very upset about this procedure.
Thank,
Jean
email me at home:jebutler@dave-and-barb.com
plz contact me on my email ayat_ismaeel@hotmail.com
i am in the 4th grade of the faculty of medicine.kasr alainy.cairo university..just attended that surgery today in general surgery..thanks alot
Thank you for the knowledge.
Bonnie
have no feeling inside of calf and most of ankle
did my doctor cut a nerve
thanks very much for the info
keep up the great work
(because she lives alone)she will need to go into a nursing/convalescant home(temporarily)to fully
recover
My question is for how long?what is the recovery time
do you know of any other circulation treatments? Please Help?
i had stients put in my heart in now 2010 will this affect my heart
My Dad was just moved to a private room an hour ago. He's progressing well. He stayed in the ICU for 4 days since surgery on Tuesday. Tough surgery as expected .. Here's the website for clear explanation about the surgical procedures. Thanks for keeping him in thoughts and prayers.
Love,
JB
Please respond as to what can be done to assess this ongoing circulation issue and prevent any further exacerbation as the physiotherapy will become more extensive with attempting to weight bare very soon.
Thank you (PS my profession involves alot of walking and I have never had any issues until my knee accident tearing my knee cartilage, acl an meniscus). SDMature
To answer Buddy question yes it is normal to have some numbness
Looking at the nurses notes, 3 weeks ago it was commented '4 sutures visible' (which I guess suggests that they should not be!).
Following day, different nurse, 'sutures snipped'!!!
I am really worried now that the sutures 'snipped' were the graft (PTFE) sutures themselves, which should never be removed. Is that level of incompetence really possible or am I clutching at straws??
now pleasw suggess me what to do
my Email id is bs27575@yahoo.co.in
Email me please about the answer
(peripheral vascular bypass )
Thanks
Carmeline
There was no appreciable relief from the operation, and again, my right foot is always 'half asleep' and is dark colored when I get up in the morning.
Is there any recourse for failed operations? My insurance and I paid a substantial sum for this!
My operation cured the rest pain for now,but i can not walk any great distance,the Surgeon told me that my operation was a salvage operation but when I tell him that my walking is very limited without numbness in the buttocks and my feet soles are numb after the operation(but was OK before the operation) the surgeon seems uninterested to investigate any further to help.
I only wished I had gone sooner to the Doctor at the first signs of the disease but I was working and based abroad at that time until I had to give up my very well paid job, and a job I loved because I just could not stand the pain in my legs any more.So for me the PVB operation helped rest pain,but as i can not walk any great distance i am fighting weight problems even though my food intake is small because the circulation in my legs is very poor.
THANKS,
NADINE
I would appreciate feedback to assure myself that all of this is normal and will eventually fade.
thanks
bob
Thanks
Do you agree the numbness will slowly go away and feeling will return?
Everything I read about this procedure indicates such pain levels at this time would be unlikely and unexpected. If there are no indications of occlusion or decreased perfusion or infection, what might explain the severe pain?
for the vascular team to monitor my progress and before I was discharged the change of colour of my toes to a healthy pink and the positive sounds from a sensor
indicated that that the operation had been a success. I have now spent a week at home in recovery where, on occasions I have had to take painkillers to reduce pain and
to help reduce swelling and tenderness. As it is now 12 days since my operation, how much longer can I expect to endure discomfort before the leg has settled down and
I can resume outdoor pursuits and other activities involving my legs?
I have a blocked artery between thigh and knee. I have got to have I believe it is called an angeagram X Ray.
This occurred about 6 weeks ago and the initial symptom was aching of the calf muscle and is very limiting.
I really don't fancy a bypass but if it is the only way, so be it.
I just wandered whether the veins, arteries could compensate and take over the original flow without the need for an operation.
The aching is less frequent and I can walk further.
Is there anyone out there, that has any good comments and personal experiences that may have paralleled my journey?
I am hoping that there is a doctor who knows what in the world is going on in my body, because I have been seen many, many, times by my General practitioner, Vascular Surgeon, Rheumatologist, Cardiologist, Urologist, Neurologist, and not one of them for the past almost 12 months can tell me what is wrong in my body and how to fix it, if it was possible??? All I know is everyday and evening I have to swollen 10 -15 pills each day and night.
Please feel free in communicating with me if you have factual and helpful info. Thank you very much for taking time in reading my message.
My husband had a femoral and tibial By Pass. He is 52 years old., aneurysm was genetic in cause.
Surgery was 3 month ago, he recovered quickly and resumed normal life.
My question is can he ski or bike?
I need some help understanding how doctors think. My husband had a fem-pop last year in September, he is 52 years old. In February is year we noticed that is something wrong with the leg, sure enough, went to the doctor and initially he said that the bypass is clogged at the calf portion of the leg. Today, after months of walking and no improvement, we find out that the bypass is completely clogged, and the aneurysm is getting blood from somewhere? In my humble opinion, the surgery was botched, but I am open to any suggestions and/ or advice..
please and Thank you