Trabeculectomy
Definition
Trabeculectomy is a surgical procedure that removes part of the trabeculum in the eye to relieve pressure caused by glaucoma.
Purpose
Glaucoma is a disease that injures the optic nerve, causing progressive vision loss. Glaucoma is a major cause of blindness in the United States. If caught early, glaucoma-related blindness is easily prevented. However, because it does not produce symptoms until late in its cycle, periodic tests for the disease are necessary.
Glaucoma is usually associated with an increase in the pressure inside the eye, called intraocular pressure (IOP). This increase occurs in front of the iris in a fluid called the aqueous humor. Aqueous humor exits through tiny channels between the iris and the cornea, in an area called the trabeculum. When the trabeculum is blocked, pressure from the build up of aqueous humor either increases rapidly with pain and redness, or builds slowly with no symptoms until there is a significant loss of vision. Trabeculectomy is the last treatment employed for either type of glaucoma. It is used only after medications and laser trabeculoplasty have failed to alleviate IOP.
Demographics
Glaucoma can develop at any age, but people over 45 are at higher risk. African Americans are more likely to develop glaucoma, especially primary open-angle glaucoma. Other factors, such as a family history of glaucoma, greatly increase the risk of contracting the disease. Diabetes and previous eye injury also increase chances of developing glaucoma.
Description
The procedure is performed in an operating room , usually under local anesthetic. However, some ophthalmologists give patients only a topical anesthetic. A trabeculectomy involves removing a tiny piece of the eye-ball,
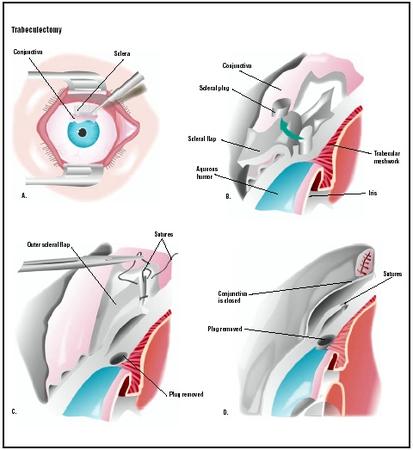
Sometimes, an additional piece is taken from the iris so that anterior chamber fluid can also flow backward into the vitreous. This procedure is called an iridectomy .
Diagnosis/Preparation
The procedure is fully explained and any alternative methods to control intraocular pressure are discussed. Antiglaucoma drugs are prescribed before surgery. Added pressure on the eye caused from coughing or sneezing should be avoided.
Several eye drops are applied immediately before surgery. The eye is sterilized, and the patient draped. A speculum is inserted to keep the eyelids apart during surgery.
Aftercare
Eye drops, and perhaps patching, will be needed until the eye is healed. Driving should be restricted until the ophthalmologist grants permission. The patient may experience blurred vision. Severe eye pain, light sensitivity, and vision loss should be reported to the physician.
Antibiotic and anti-inflammatory eye drops must be used for at least six weeks after surgery. Additional medicines may be prescribed to reduce scarring.
Risks
Infection and bleeding are risks of any surgery. Scarring can cause the drainage to stop. One-third of trabeculectomy patients will develop cataracts.
Normal results
Trabeculectomy will delay the progression of glaucoma. In many cases, people still require medication to lower IOP.
Morbidity and mortality rates
Trabeculectomy is considered a safe procedure. Infection is a complication that could lead to more serious medical problems; however, it is controllable with eye drops.
Alternatives
Physicians will first try to lower IOP with glaucoma medications. Several types of eye drops are effective for this use. Sometimes a patient must instill more than one eye drop, several times a day. Compliance is very important when using these eye drops; missed dosages will raise IOPs.
Lasers are now used to treat both closed-angle and open-angle glaucoma. Peripheral iridectomy is used for people with acute angle-closure glaucoma attacks and chronic closed-angle glaucoma. The procedure creates a hole to improve the flow of aqueous humor.
Laser trabeculoplasty uses an argon laser to create tiny burns on the trabecular meshwork, which lowers IOP. The effects, however, are not permanent, and the patient must be retreated.
Transscleral cyclophotocoagulation treats the ciliary body with a laser to decrease production of aqueous humor, which reduces IOP.
A tube shunt might be implanted to create a drainage pathway in patients who are not candidates for trabeculectomy.
Resources
books
Cassel, Gary H., M.D., Michael D. Billig, O.D., and Harry G. Randall, M.D. The Eye Book: A Complete Guide to Eye Disorders and Health. Baltimore, MD: Johns Hopkins University Press, 1998.
Daly, Stephen, ed. Everything You Need to Know About Medical Treatments. Springhouse, PA: Springhouse Corp., 1996.
Sardegna, Jill, et. al. The Encyclopedia of Blindness and Vision Impairment, 2nd ed. New York: Facts on File, Inc., 2002.
Vaughan, Daniel, Ed. General Ophthalmology, 13th ed. Stamford, CT: Appleton & Lange, 1993.
organizations
The Glaucoma Foundation. 116 John Street, Suite 1605 New York, NY 10038. (212) 285-0080. info@glaucomafoundation.org. http://www.glaucomafoundation.org
other
"Glaucoma Filtration Procedure." EyeMdLink.com . [cited May 18, 2003] http://www.eyemdlink.com/EyeProcedure.aspEyeProcedureID=44> .
J. Ricker Polsdorfer, M.D. Mary Bekker
WHO PERFORMS THE PROCEDURE AND WHERE IS IT PERFORMED?
Ophthalmologists and optometrists may detect and treat glaucoma; however, only ophthalmologists can perform surgery. Ophthalmologists who are glaucoma subspecialists may have an additional two years of fellowship training.
The outpatient surgery is performed in a hospital or surgery suite designed for ophthalmic surgery.
QUESTIONS TO ASK THE DOCTOR
- Will IOP-lowering medication be needed after the surgery?
- How long will it take to determine if the surgery was a success?
- Can cataracts be treated in conjunction with glaucoma surgery?
- When will vision return to normal?
This is the surgery I am having. I hope you get this. Love,N
my right eye pressure was 38, and my left eye is still 33, so I will have to have the left eye done as well.
I have had all laser treatments, which didn't work for longer than two years.
My pressure in the operated eye is 11 post -operatively.
My eye looks diferent than the other: it droops a little, but not much.
Where do you go to have the droopy eye corrected, and who does the surgery.
I don't know if I want my left eye done, but I will need to save my sight, so i will have to.
I had a lot of pain for week after op and my sight was awful for 3 weeks.
However it has improved a lot in last two weeks pain nearly all gone and sight almost back to normal. Pressure down to 12.
I did hace v low pressure post op, which led to choroidal leak and black lines, another issue they fail to warn you about, all gone now.
The op is essential in most cases so all one needs to be is well prepared and have a clear understanding of what is going to happen
kinds of drops failed to bring the pressure down. Surgery for my other eye is scheduled for Sept. 14th.
I'm hopng for the best outcome from this proceedure, but feeling discouraged because of the comments I've
read. Let's hear from others who have had better results.
kinds of drops failed to bring the pressure down. Surgery for my other eye is scheduled for Sept. 14th.
I'm hopng for the best outcome from this proceedure, but feeling discouraged because of the comments I've
read. Let's hear from others who have had better results.
So far it's been answered prayers. Some discomfort, but I wouldn't call it pain. Vision was bad before and after a couple of days it's still the same. The eye is red, co-worker told me it's perfect for Halloween next week, it does look scarey. Pressure is down to a 7. Today he checked it again. First reading was 14. Doc pressed just under the eye and did a second reading, a 7.
Hindsight, because of the vision loss I should have asked for the op sooner. My right eye, 20/25 corrected, pressure is in the mid teens. If that starts going up, I'll ask for surgery ASAP. At 63, I'm still working as an accountant. It's slow but I can do it with one eye, but can't if the good eye goes bad.
Praying complete healing for everyone on this thread. Aloha Ke Akua.
Aren’t us human’s marvellous creatures?
Pity we could not all help one another instead of the mindless and senseless stupidity we see around the world.
What is good pressure.My pressure is 15 in the left eye and 17 in the right eye. My doctor is recommending a Trabeculectomy in the right eye. I have not had laser surgery. Just used drops
What is good pressure.My pressure is 15 in the left eye and 17 in the right eye. My doctor is recommending a Trabeculectomy in the right eye. I have not had laser surgery. Just used drops
Are the discoloration and the droopiness permanent?
I had a trabeculectomy 9 months ago.Doctor said I got glaucoma as a result of taking prednisone(solupred) for treatment of ulcerative colitis.Now I see like a tearing/opening in the top periphery of my iris beside the operated area(triangular).I went to an ophthalmologist to check that tearing/fissure making an opening in my iris, and I was told it's a result of trabeculectomy and not to worry about it.
Can you please tell me if that's normal??Why now am seeing that tearing of iris?
Is it serious?Can you please explain what happened to my iris?
Thanks,
Roshan.
Not really sure what I want to do - hate the thought of taking drops again as my eyes look so much healthier - feel like going with prayer thinking it will work best
Three years after surgery on left eye the right one needs same thing. Doctor recommends a canaloplasty. Insurance denies payment but I do it anyway since have so many issues with the other procedure. It turns out perfectly. No side effects and normal pressures for 15 months now. In my third appeal with the insurance company (Anthem Blue Cross).
I'm 54 in good health otherwise. One other note is I was adopted so have no family history of medical issues. It may have helped to know but the social system does not allow me access. Too bad, it may have helped me be more preventative with some of this.
eye drops (pred forte and vigamox) was done on an hourly basis after the patch was removed the next of the surgery...
June 22, 1st post surgery check up - eyes very swollen but expected tho...trabec covered with contact lens for protection
June 24, 2nd post surgery check up - continue hourly eye drops
June 27, 3rd post surgery check up - contact lens remove and - eye pressure at 10!!!
June 30, 4th post surgery check up - 1 suture removed and eye pressure at 14. eye drops every other hour.
July 7, next check up...
...TRABECULECTOMY was an answer to my prayers to control the total loss of my BF's eye sight...
Source: inflatu
My doc is one of those who did original research and studies on the iStent. I was hoping to get one of those instead of a trab, but the FDA is being slow with its final approval (supposedly coming "any day now").
it comes and goes very quickly .the docs were unsure, said it may be a drop in pressure occasionaly and put me on anti biotics.
anyone had these dents appear ?
The first trabeculectomy was very uncomfortable for a few months, and remained at a mild level of discomfort for about a year, but the pressure has stabilized at around 11.
The second one, 6 days ago, is surprising in its lack of discomfort. Vision won't return to normal for a while, but I am able to drive again.
The worst I can say is that I developed a cataract in the first eye and will have that taken care of when the last trab has healed sufficiently for my surgeon to give the go-ahead.
My best wishes to all who are thinking of this surgery - my your surgeon be as good as the ones I had and may your eyes have all of the right characteristics for a successful surgery.
But I am fortifying myself by reading, reading, reading from appropriate sources - ie nothing alarmist, more like medical journals.
I can't encourage everyone enough to READ, READ, READ about your condition. Accept NOTHING the surgeons say. Question everything, take second, third and fourth opinions. The medical journals confirm it is the experienced individual surgeon who has many years of experience doing trabbies who offer you the best chance for a successful procedure.
Prior to the trab, on initial diagnosis of high IOP (intraocular pressure should be between 10 - 21; anything higher and you will be treated - first for Ocular Hyper Tension, then gradually the doctors might acknowledge you have glaucoma and, as your vision decreases, they will consider surgical intervention).
Trabeculectomy is the gold standard, but other less-invasive, more frequently repeatable procedures are offered to older patients, such as Selective Laser Trabeculoplasty. All I can say is, DO YOUR RESEARCH. Know what is happening to your eye!
If you've been told you have Ocular Hyper Tension, high IOP or suspected glaucoma, monitor your vision every day! Look for extended blind spots, go for regular check-ups, and take the eye drops scrupulously. Be aware they have sometimes have very depressing side effects.
Ask about everything, don't just accept everything your doctors tell you!
My surgeon has done 2,000+ trabs. Find a specialist. Find someone who will extensively use antibiotics and steroids post-surgery. I am hopeful that I will need no drops at all and that my pressures will remain low. She already discussed future cataract surgery (cataracts generally grow more quickly after trabs) and said that I most likely would not need to wear glasses in the future.
If I had known that the surgery was going to be so successful, I would not have put it off as long as I did. I was diagnosed with advanced glaucoma on June 7, 2012. 75% of the vision in my right eye was gone, even though I had had field tests for seven years and my optometrist never discussed them with me or told me I had glaucoma or blindness. The ophthalmologist I saw quickly ordered an MRI (which showed no issues) and upped my one "preglaucoma" drop (according to my optometrist) to three drops a day, then six drops a day and then performed two laser surgeries last August. None of these succeeded in keeping down my IOP. In October 2012, I met with a specialist at Washington University in St. Louis. She added another drop and closely monitored me until surgery became necessary.
I stress this again: Do diligent research and find a specialist with a lot of experience!!
The fluid is now copious, tinged with blood and filling my sclera so that it looks like my eye is filled with bloody tears. I have called the emergency line twice, but the calm doctor on call tells me each time that is NORMAL and not to worry unless there is deep seated pain. So I wait. Gotta make it through the weekend to see the surgeon on Monday. At least it isn't hurting. Just uncomfortable. The surgeon told me to stop the antibiotics and cut the steroids in half to try to stop the scarring blocking the flow from the blob. I am concerned about the lack of antibiotics so soon after surgery. 9 days. I will post again on Monday and let everyone know what he says.
To Sylvia, pain after this many months I would say is not normal, and you should see another doctor, I think. I wish you well!
The left eye has just been done - just mild discomfort owing an end of the stitches catching lid pressure down to 12
A praises to one amazing surgeon
Can somebody advise whether i should go ahead. Thanks.
and the pressure coming back. Got to try another surgery which is to install a small tube in the eyes. God bless me and everyone is this forum.
Vision still a little blurred and I go back this Thursday to have an injection to reduce scarring problems. I was very nervous on the days leading up to the operation and
I told them this they were very understanding. At this stage I can only say thank you NHS I firmly believe if they had not taken this action I would have eventually lost my
sight.
I have just had my surgery (surprisingly quick and pain free) , and I have just had my post op visit the day after surgery. My pressure must have been high. The doctor lasered a stitch (I had five sutures) at his office (OWWW it hurt!! Made me jump!!), then my pressure was 16 after he massaged the eye (sore from the surgery, ugh). Going to see him again later this week for another follow up, taking the steroid drops and the anti-bacterial drops as prescribed. Eye is red, but I can see out of it and only some discomfort from the external sutures, which I'm told eventually I won't notice.
I'm young for this (just turned 49), but I don't want to slowly go blind in either eye. If the trabeculectomy works as it should, I will only have to use a drop a day in the left eye, and no further drops int he right. The treb operation may last decades if it maintains correctly. I am going to be taught later how to massage my eye to keep the filter flowing.
Until this problem arose I was very pleased with the way things were going.. I am just hoping the setback will turn out to be temporary. In spite of everything I can still use ny computer (obviously, since I am typing this myself), so that at least is grounds for optimism.