Electroencephalography
Definition
Electroencephalography, or EEG, is a neurological test that involves attaching electrodes to the head of a person to measure and record electrical activity in the brain over time.
Purpose
The EEG, also known as a brain wave test, is a key tool in the diagnosis and management of epilepsy and other seizure disorders. It is also used to assist in the diagnosis of brain damage and diseases such as strokes, tumors, encephalitis, mental retardation, and sleep disorders. The results of the test can distinguish psychiatric conditions such as schizophrenia, paranoia, and depression from degenerative mental disorders such as Alzheimer's and Parkinson's diseases. An EEG may also be used to monitor brain activity during surgery to assess the effects of anesthesia. It is also used to determine brain status and brain death.
Demographics
The number of EEG tests performed each year can only be estimated. It is not a reportable event and is used in the diagnostic workup for a number of disorders. The number of EEG tests per year is estimated to be in the range of 10–25 million.
Description
Before an EEG begins, a nurse or technologist attaches approximately 16–21 electrodes to a person's scalp
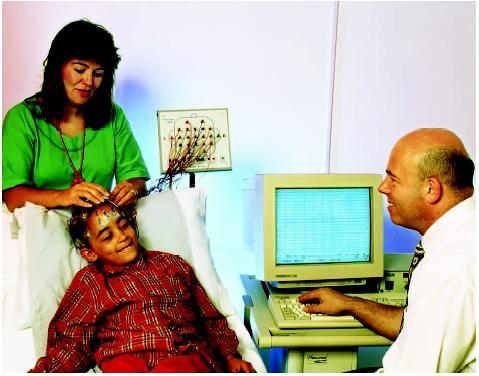
For the test, a person lies on a bed, padded table, or comfortable chair and is asked to relax and remain still while measurements are being taken. An EEG usually takes no more than one hour, although long-term monitoring is often used for diagnosis of seizure disorders. During the test procedure, a person may be asked to breathe slowly or quickly. Visual stimuli such as flashing lights or a patterned board may be used to stimulate certain types of brain activity. Throughout the procedure, the electroencephalography unit makes a continuous graphic record of the person's brain activity, or brain waves, on a long strip of recording paper or computer screen. This graphic record is called an electroencephalogram. If the display is computerized, the test may be called a digital EEG, or dEEG.
The sleep EEG uses the same equipment and procedures as a regular EEG. Persons undergoing a sleep EEG are encouraged to fall asleep completely rather than just relax. They are typically provided a bed and a quiet room conducive to sleep. A sleep EEG lasts up to three hours, or up to eight or nine hours if it is a night's sleep.
In an ambulatory EEG, individuals are hooked up to a portable cassette recorder. They then go about normal activities and take normal rest and sleep for a period of up to 24 hours. During this period, individuals and their family members record any symptoms or abnormal behaviors, which can later be correlated with the EEG to see if they represent seizures.
An extension of the EEG technique, called quantitative EEG (qEEG), involves manipulating the EEG signals with a computer using the fast Fourier transform algorithm. The result is then best displayed using a colored gray scale transposed onto a schematic map of the head to form a topographic image. The brain map produced in this technique is a vivid illustration of electrical activity in the brain. This technique also has the ability to compare the similarity of the signals between different electrodes, a measurement known as spectral coherence. Studies have shown the value of this measurement in diagnosis of Alzheimer's disease and mild closed head injuries. The technique can also identify areas of the brain having abnormally slow activity when the data are both mapped and compared to known normal values. The result is then known as a statistical or significance probability map (SPM). This allows differentiation between early dementia (increased slowing) or otherwise uncomplicated depression (no slowing).
Diagnosis/Preparation
An EEG is generally performed as one test in a series of neurological evaluations. Rarely does the EEG form the sole basis for a particular diagnosis.
Full instructions should be given to individuals receiving an EEG when they schedule their test. Typically, individuals taking medications that affect the central nervous system, such as anticonvulsants, stimulants, or antidepressants, are told to discontinue their prescription for a short time prior to the test (usually one to two days). However, such requests should be cleared with the treating physician. EEG test candidates may be asked to avoid food and beverages that contain caffeine, a central nervous system stimulant. They may also be asked to arrive for the test with clean hair that is free of styling products to make attachment of the electrodes easier.
Individuals undergoing a sleep EEG may be asked to remain awake the night before their test. They may be given a sedative prior to the test to induce sleep.
Aftercare
If an individual has suspended regular medication for the test, the EEG nurse or technician should advise as to when to begin taking it again.
Risks
Being off certain medications for one to two days may trigger seizures. Certain procedures used during EEG may trigger seizures in persons with epilepsy. Those procedures include flashing lights and deep breathing. If the EEG is being used as a diagnostic for epilepsy (i.e., to determine the type of seizures an individual is experiencing) this may be a desired effect, although the person needs to be monitored closely so that the seizure can be aborted if necessary. This type of test is known as an ictal EEG.
Normal results
In reading and interpreting brain wave patterns, a neurologist or other physician will evaluate the type of brain waves and the symmetry, location, and consistency of brain wave patterns. Brain wave response to certain stimuli presented during the EEG test (such as flashing lights or noise) will also be evaluated.
The four basic types of brain waves are alpha, beta, theta, and delta, with the type distinguished by frequency. Alpha waves fall between 8 and 13 Hertz (Hz), beta are above 13 Hz, theta between 4 and 7 Hz, and delta are less than 4 Hz. Alpha waves are usually the dominant rhythm seen in the posterior region of the brain in older children and adults, when awake and relaxed. Beta waves are normal in sleep, particularly for infants and young children. Theta waves are normally found during drowsiness and sleep and are normal in wakefulness in children, while delta waves are the most prominent feature of the sleeping EEG. Spikes and sharp waves are generally abnormal; however, they are common in the EEG of normal newborns.
Different types of brain waves are seen as abnormal only in the context of the location of the waves, a person's age, and one's conscious state. In general, disease typically increases slow activity, such as theta or delta waves, but decreases fast activity, such as alpha and beta waves.
Not all decreases in wave activity are abnormal. The normal alpha waves seen in the posterior region of the brain are suppressed merely if a person is tense. Sometimes the addition of a wave is abnormal. For example, alpha rhythms seen in a newborn can signify seizure activity. Finally, the area where the rhythm is seen can be telling. The alpha coma is characterized by alpha rhythms produced diffusely, or, in other words, by all regions of the brain.
Some abnormal beta rhythms include frontal beta waves that are induced by sedative drugs. Marked asymmetry in beta rhythms suggests a structural lesion on the side lacking the beta waves. Beta waves are also commonly measured over skull lesions, such as fractures or burr holes, in activity known as a breach rhythm.
Usually seen only during sleep in adults, the presence of theta waves in the temporal region of awake, older adults has been tentatively correlated with vascular disease. Another rhythm normal in sleep, delta rhythms, may be recorded in the awake state over localized regions of cerebral damage. Intermittent delta rhythms are also an indication of damage of the relays between the deep gray matter and the cortex of the brain. In adults, this intermittent activity is found in the frontal region whereas in children, it is in the occipital region.
The EEG readings of persons with epilepsy or other seizure disorders display bursts, or spikes, of electrical activity. In focal epilepsy, spikes are restricted to one hemisphere of the brain. If spikes are generalized to both hemispheres of the brain, multifocal epilepsy may be present. The EEG can be used to localize the region of the brain where the abnormal electrical activity is occurring. This is most easily accomplished using a recording method, or montage, called an average reference montage. With this type of recording, the signal from each electrode is compared to the average signal from all the electrodes. The negative amplitude (upward movement, by convention) of the spike is observed for the different channels, or inputs, from the various electrodes. The negative deflection will be greatest as recorded by the electrode that is closest in location to the origin of the abnormal activity. The spike will be present but of reduced amplitude as the electrodes move farther away from the site producing the spike. Electrodes distant from the site will not record the spike occurrence.
A final variety of abnormal result is the presence of slower-than-normal wave activity, which can either be a slow background rhythm or slow waves superimposed on a normal background. A posterior dominant rhythm of 7 Hz or less in an adult is abnormal and consistent with encephalopathy (brain disease). In contrast, localized theta or delta rhythms found in conjunction with normal background rhythms suggest a structural lesion.
Morbidity and mortality rates
There are few adverse conditions associated with an EEG test. Persons with seizure disorders may induce seizures during the test in reaction to flashing lights or by deep breathing. Mortality from an EEG has not been reported.
Alternatives
There are no equivalent tests that provide the same information as an EEG.
Resources
books
Chin, W. C., and T. C. Head. Essentials of Clinical Neurophysiology, 3rd ed. London: Butterworth-Heinemann, 2002.
Daube, J. R. Clinical Neurophysiology, 2nd edition. New York: Oxford University Press, 2002.
Ebersole, J. S., and T. A. Pedley. Current Practice of Clinical Electroencephalography, 3rd ed. Philadelphia: Lippincott Williams & Wilkins, 2002.
Rowan, A. J., and E. Tolunsky. Primer of EEG. London: Butterworth-Heinemann, 2003.
periodicals
De Clercq, W., P. Lemmerling, S. Van Huffel, and W. Van Paesschen. "Anticipation of Epileptic Seizures from Standard EEG Recordings." Lancet 361, no. 9361 (2003): 971–972.
Harden, C. L., F. T. Burgut, and A. M. Kanner. "The Diagnostic Significance of Video-EEG Monitoring Findings on Pseudoseizure Patients Differs Between Neurologists and Psychiatrists." Epilepsia 44, no. 3 (2003): 453–456.
Stepien, R. A. "Testing for Non-linearity in EEG Signal of Healthy Subjects." Acta Experimental Neurobiology 62, no. 4 (2002): 277–281.
Vanhatalo, S., M. D. Holmes, P. Tallgren, J. Voipio, K. Kaila, and J. W. Miller. "Very Slow EEG Responses Lateralize Temporal Lobe Seizures: An Evaluation of Non-invasive DC-EEG." Neurology 60, no. 7 (2003): 1098–1104.
organizations
American Association of Electrodiagnostic Medicine. 421 First Avenue SW, Suite 300 East, Rochester, MN 55902. (507) 288–0100, Fax: (507) 288–1225. aaem@aaem.net. http://www.aaem.net/ .
American Board of Registration for Electroencephalographic Technologists. P.O. Box 916633, Longwood, FL 32791-6633 .
American Board of Registration of EEG and EP Technologists. PO Box 891663, Longwood, FL 32791. (407) 788–6308. http://www.abret.org/index.htm .
American Society of Electroneurodiagnostic Technologists Inc. 204 W. 7th Carroll, IA 51401. (712) 792–2978. http://www.aset.org/ .
Epilepsy Foundation. 4351 Garden City Drive, Landover, MD 20785-7223. (800) 332–1000 or (301) 459–3700. http://www.efa.org .
Joint Review Committee on Electroneurodiagnostic Technology. 3350 South 198th Rd., Goodson, MO 65659-9110. (417) 253–5810. http://www.caahep.org/about/coas.htm .
other
Hofstra University. "Electroencephalography." [cited April 27, 2003]. http://people.hofstra.edu/faculty/sina_y_rabbany/engg181/EEG.html .
Bergey, Gregory K., and Piotr J. Franaszczuk. "Epileptic Seizures are Characterized by Changing Signal Complexity." [cited April 17, 2003]. http://erl.neuro.jhmi.edu/pfranasz/CN00/cn00.pdf .
Rutherford, Kim, M.D. "EEG (Electroencephalography)." Kid's Health For Parents. June 2001 [cited April 27, 2003]. http://kidshealth.org/parent/system/medical/eeg.html .
National Society for Epilepsy. "Epilepsy Information: Electroencephalography." September 2002 [cited April 27, 2003]. http://www.epilepsynse.org.uk/pages/info/leaflets/eeg.cfm .
L. Fleming Fallon, Jr., MD, DrPH
WHO PERFORMS THE PROCEDURE AND WHERE IS IT PERFORMED?
Electroencephalography is often administered by specially trained technicians who are supervised by a neurologist or other physician with specialized training in administering and interpreting the test. Because of the equipment involved, an EEG is usually administered in a hospital setting. It may be conducted in a professional office.
QUESTIONS TO ASK THE DOCTOR
- How many EEG procedures has the technician performed?
- What preparations are being made to treat an induced seizure?
- Is the supervising physician appropriately certified to interpret an EEG?
my son is 7 years old stdying inclass second in KV since last six
months he has occassionaly some fits like symtoms spl during sleeping
time he thorws his legs for two mts during sleep and cries but again
h lseep well till up to morning
he sleep well and day time he is quite okpalye swell eats well
eveything but he is very lazy in his dyudy workssmewhat dent ant to do
any study excpet compauter games and tv etc and outside play etc
such events has come six times iregreguarly as we observed innight
time during sleep only
we have shwn to nuerologists they have given one medicine after EEG
test shows slight sub abnormality inright brain they adivisd us it
will be cured by medicne
may I please let meknow your kind advice in this regard
what steps we have to take is it
her grand mother has eplipse problem mother side he is negative
grupmothere is also o negative i have one more boy who is 11 years
old and he is ok in all matters
AWAITING YOUR KIND ADVICE
my son is 7 years old stdying inclass second in KV since last six
months he has occassionaly some fits like symtoms spl during sleeping
time he thorws his legs for two mts during sleep and cries but again
h lseep well till up to morning
he sleep well and day time he is quite okpalye swell eats well
eveything but he is very lazy in his dyudy workssmewhat dent ant to do
any study excpet compauter games and tv etc and outside play etc
such events has come six times iregreguarly as we observed innight
time during sleep only
we have shwn to nuerologists they have given one medicine after EEG
test shows slight sub abnormality inright brain they adivisd us it
will be cured by medicne
may I please let meknow your kind advice in this regard
what steps we have to take is it
her grand mother has eplipse problem mother side he is negative
grupmothere is also o negative i have one more boy who is 11 years
old and he is ok in all matters
AWAITING YOUR KIND ADVICE
My seven yr old had shuddering episode after an esp exciting week and lack of sleep. An EEG was suggested - 1 hr sleep deprived. A slight abnormality was noted in the left frontal lobe - 5 spikes during EEG. He was not very cooperative toward the end of the procedure and the technician needed to re align the wires... Neurologist recommended either to do nothing and watch or do more testing; MRI or 24 hr video EEG. He is bright, normal, healthy boy with no other issues. Unsure as to how to proceed. Any advice would be appreciated. Thank you.
BLOOD TESTS INDICATED A BACTERIAL INFECTION. A LUMBER PUNCTURE WAS PERFORMED.
MENINGITIS AND TB WERE ELIMINATED BUT THE SEIZURES CONTINUED. AN EEG IS GOING TO BE INFORMED WHAT ARE THE IMPLICATIONS? COULD IT BE EPILEPSY? CAN IT BE CURED? PLEASE HELP.